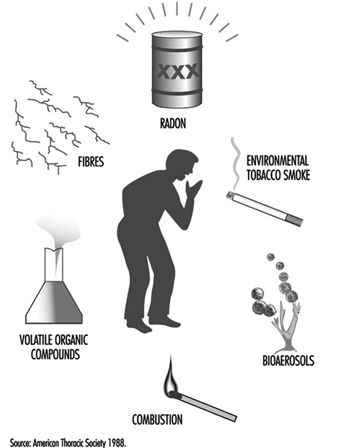
Air Pollution
The problem of air pollution has grown steadily since the Industrial Revolution began 300 years ago. Four major factors have exacerbated air pollution: growing industrialization; increasing traffic; rapid economic development; and higher levels of energy consumption. The available information shows that the WHO guidelines for the major air pollutants are regularly exceeded in many major urban centres. Although progress has been made in controlling air pollution problems in many industrialized countries over the last two decades, air quality—particularly in the larger cities in the developing world—is worsening. Of major concern are the adverse health effects of ambient air pollutants in many urban areas, where levels are sufficiently high to contribute to increased mortality and morbidity, deficits in pulmonary function and cardiovascular and neurobehavioural effects (Romieu, Weizenfeld and Finkelman 1990; WHO/UNEP 1992). Indoor air pollution due to domestic combustion products is also a major issue in developing countries (WHO 1992b), but it is not part of this review, which considers only the sources, dispersion and health effects of outdoor air pollution, and includes a case study of the situation in Mexico.
Source of Air Pollutants
The most common air pollutants in urban environments include sulphur dioxide (SO2), suspended particulate matter (SPM), the nitrogen oxides (NO and NO2, collectively termed NOX), ozone (O3), carbon monoxide (CO) and lead (Pb). Combustion of fossil fuels in stationary sources leads to the production of SO2, NOX and particulates, including sulphate and nitrate aerosols formed in the atmosphere following gas to particle conversion. Petrol-fuelled motor vehicles are the principal sources of NOX, CO and Pb, whereas diesel-fuelled engines emit significant quantities of particulates, SO2 and NOX. Ozone, a photochemical oxidant and the main constituent of photochemical smog, is not emitted directly from combustion sources but is formed in the lower atmosphere from NOX and volatile organic compounds (VOCs) in the presence of sunlight (UNEP 1991b). Table 1 presents the major sources of outdoor air pollutants.
Table 1. Major sources of outdoor air pollutants
Pollutants Sources
Sulphur oxides Coal and oil combustion, smelters
Suspended particulate matter Combustion products (fuel, biomass), tobacco smoke
Nitrogen oxides Fuel and gas combustion
Carbon monoxide Incomplete petrol and gas combustion
Ozone Photochemical reaction
Lead Petrol combustion, coal combustion, producing batteries, cables, solder, paint
Organic substances Petrochemical solvents, vaporization of unburnt fuels
Source: Adapted from UNEP 1991b.
Dispersion and Transport of Air Pollutants
The two major influences on the dispersion and transport of air pollutant emissions are the meteorology (including microclimate effects such as “heat islands”) and the topography in relation to the population distribution. Many cities are surrounded by hills which may act as a downwind barrier, trapping pollution. Thermal inversions contribute to a particulate problem in temperate and cold climates. Under normal dispersion conditions, hot pollutant gases rise as they come into contact with colder air masses with increasing altitude. However, under certain circumstances the temperature may increase with altitude, and an inversion layer forms, trapping pollutants close to the emission source and delaying their diffusion. Long-range transport of air pollution from large urban areas may have national and regional impacts. Oxides of nitrogen and sulphur may contribute to acid deposition at great distances from the emission source. Ozone concentrations are often elevated downwind of urban areas due to the time lag involved in photochemical processes (UNEP 1991b).
Health Effects of Air Pollutants
Pollutants and their derivatives can cause adverse effects by interacting with and impairing molecules crucial to the biochemical or physiological processes of the human body. Three factors influence the risk of toxic injury related to these substances: their chemical and physical properties, the dose of the material that reaches the critical tissue sites and the responsiveness of these sites to the substance. The adverse health effects of air pollutants may also vary across population groups; in particular, the young and the elderly may be especially susceptible to deleterious effects. Persons with asthma or other pre-existing respiratory or cardiac diseases may experience aggravated symptoms upon exposure (WHO 1987).
Sulphur Dioxide and Particulate Matter
During the first half of the twentieth century, episodes of marked air stagnation resulted in excess mortality in areas where fossil-fuel combustion produced very high levels of SO2 and SMP. Studies of long-term health effects have also related the annual mean concentrations of SO2 and SMP to mortality and morbidity. Recent epidemiological studies have suggested an adverse effect of inhalable particulate levels (PM10) at relatively low concentrations (not exceeding the standard guidelines) and have shown a dose-response relationship between exposure to PM10 and respiratory mortality and morbidity (Dockery and Pope 1994; Pope, Bates and Razienne 1995; Bascom et al. 1996) as shown in table 2.
Table 2. Summary of short-term exposure-response relationship of PM10 with different health effects indicators
|
Health effect |
% changes for each 10 μg/m3 |
|
|
Mean |
Range |
|
|
Mortality |
||
|
Total |
1.0 |
0.5-1.5 |
|
Cardiovascular |
1.4 |
0.8-1.8 |
|
Respiratory |
3.4 |
1.5-3.7 |
|
Morbidity |
||
|
Hospital admission for respiratory condition |
1.1 |
0.8-3.4 |
|
Emergency visits for respiratory conditions |
1.0 |
0.5-4 |
|
Symptom exacerbations among asthmatics |
3.0 |
1.1-11.5 |
|
Changes in peak expiratory flow |
0.08 |
0.04-0.25 |
Nitrogen Oxides
Some epidemiological studies have reported adverse health effects of NO2 including increased incidence and severity of respiratory infections and increase in respiratory symptoms, especially with long-term exposure. Worsening of the clinical status of persons with asthma, chronic obstructive pulmonary disease and other chronic respiratory conditions has also been described. However, in other studies, investigators have not observed adverse effects of NO2 on respiratory functions (WHO/ECOTOX 1992; Bascom et al. 1996).
Photochemical Oxidants and Ozone
The health effects of photochemical oxidants exposure cannot be attributed only to oxidants, because photochemical smog typically consists of O3, NO2, acid and sulphate and other reactive agents. These pollutants may have additive or synergistic effects on human health, but O3 appears to be the most biologically active. Health effects of ozone exposure include decreased pulmonary function (including increased airway resistance, reduced air flow, decreased lung volume) due to airway constriction, respiratory symptoms (cough, wheezing, shortness of breath, chest pains), eye, nose and throat irritation, and disruption of activities (such as athletic performance) due to less oxygen availability (WHO/ECOTOX 1992). Table 3 summarizes the major acute health effects of ozone (WHO 1990a, 1995). Epidemiological studies have suggested a dose-response relationship between exposure to increasing ozone levels and the severity of respiratory symptoms and the decrement in respiratory functions (Bascom et al. 1996).
Table 3. Health outcomes associated with changes in peak daily ambient ozone concentration in epidemiological studies
|
Health outcome |
Changes in |
Changes in |
|
Symptom exacerbations among healthy children |
||
|
25% increase |
200 |
100 |
|
50% increase |
400 |
200 |
|
100% increase |
800 |
300 |
|
Hospital admissions for respiratory |
||
|
5% |
30 |
25 |
|
10% |
60 |
50 |
|
20% |
120 |
100 |
a Given the high degree of correlation between the 1-h and 8-h O3 concentrations in field studies, an improvement in health risk associated with decreasing 1- or 8-h O3 levels should be almost identical.
Source: WHO 1995.
Carbon Monoxide
The main effect of CO is to decrease oxygen transport to the tissues through the formation of carboxyhaemoglobin (COHb). With increasing levels of COHb in blood, the following health effects can be observed: cardiovascular effects in subjects with previous angina pectoris (3 to 5%); impairment of vigilance tasks (>5%); headache and dizziness (≥10%); fibrinolysis and death (WHO 1987).
Lead
Lead exposure principally affects haem biosynthesis, but also may act on the nervous system and other systems such as the cardiovascular system (blood pressure). Infants and young children less than five years old are particularly sensitive to lead exposure because of its effect on neurological development at blood lead levels close to 10 μg/dl (CDC 1991).
Several epidemiological studies have investigated the effect of air pollution, especially ozone exposure, on the health of the population of Mexico City. Ecological studies have shown an increase in mortality with respect to exposure to fine particulates (Borja-Arburto et al. 1995) and an increase in emergency visits for asthma among children (Romieu et al. 1994). Studies of the adverse effect of ozone exposure conducted among healthy children have shown an increase in school absenteeism due to respiratory illnesses (Romieu et al. 1992), and a decrease in lung function after both acute and subacute exposure (Castillejos et al. 1992, 1995). Studies conducted among asthmatic children have shown an increase in respiratory symptoms and a decrease in peak expiratory flow rate after exposure to ozone (Romieu et al. 1994) and to fine particulate levels (Romieu et al. in press). Although, it seems clear that acute exposure to ozone and particulates is associated with adverse health effects in the population of Mexico City, there is a need to evaluate the chronic effect of such exposure, in particular given the high levels of photo-oxidants observed in Mexico City and the ineffectiveness of control measures.
Case study: Air pollution in Mexico City
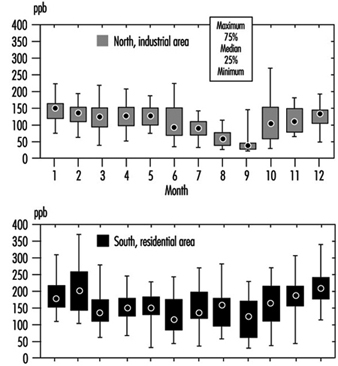
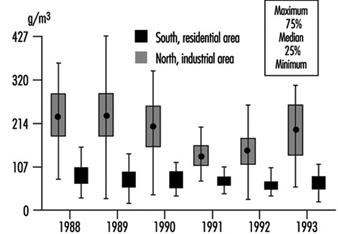
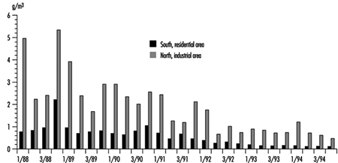
The metropolitan area of Mexico City (MAMC) is situated in the Mexican Basin at a mean altitude of 2,240 metres. The basin covers 2,500 square kilometres and is surrounded by mountains, two of which are over 5,000 metres high. The total population was estimated at 17 million in 1990. Due to the particular geographic characteristics and the light winds, ventilation is poor with a high frequency of thermic inversions, especially during the winter. More than 30,000 industries in the MAMC and the three million motor vehicles circulating daily are responsible for 44% of the total energy consumption. Since 1986, air pollution has been monitored, including SO2, NOx, CO, O3, particulate matter and non-methane hydrocarbon (HCNM). The main air pollutant problems are related to ozone, especially in the southwest part of the city (Romieu et al. 1991). In 1992 the Mexican norm for ozone (110 ppb one-hour maximum) was exceeded in the southwest part more than 1,000 hours and reached a maximum of 400 ppb. Particulate levels are high in the northeast section of the city, close to the industrial park. In 1992, the annual average of inhalable particulate (PM10) was 140 μg/m3. Since 1990, important control measures have been taken by the government to decrease air pollution, including a programme that prohibits use of cars one day a week depending on their terminating licence plate number, the closure of one of the most polluting refineries located in Mexico City, and the introduction of unleaded fuel. These measures have led to a decrease in various air pollutants, mainly SO2, particulate matter, NO2, CO and lead. However the ozone level remains a major problem (see figure 1, figure 2 and figure 3).
Figure 1. Ozone levels in two zones of Mexico City. One-hour daily maximum by month, 1994
Figure 2. Particulates (PM10) in two zones of Mexico City, 1988-1993
Figure 3. Air lead levels in two zones of Mexico City, 1988-1994
Developing Countries and Pollution
Industrial pollution is a more complicated problem in developing countries than in developed economies. There are greater structural obstacles to preventing and cleaning up pollution. These obstacles are largely economic, because developing countries do not have the resources to control pollution to the extent that developed countries can. On the other hand, the effects of pollution may be very costly to a developing society, in terms of health, waste, environmental degradation, reduced quality of life and clean-up costs in the future. An extreme example is concern for the future of children exposed to lead in some megacities in countries where leaded gasoline is still used, or in the vicinity of smelters. Some of these children have been found to have blood lead levels high enough to impair intelligence and cognition.
Industry in developing countries usually operates short of capital compared to industry in developed countries, and those investment funds that are available are first put into the equipment and resources necessary for production. Capital that is applied toward control of pollution is considered “unproductive” by economists because such investment does not lead to increased production and financial return. However, the reality is more complicated. Investment in control of pollution may not bring an obvious direct return on investment to the company or industry, but that does not mean that there is no return on investment. In many cases, as in an oil refinery, control of pollution also reduces the amount of wastage and increases the efficiency of the operation so that the company does benefit directly. Where public opinion carries weight and it is to the advantage of a company to maintain good public relations, industry may make an effort to control pollution in its own interest. Unfortunately, the social structure in many developing countries does not favour this because the people most negatively affected by pollution tend to be those who are impoverished and marginalized in society.
Pollution may damage the environment and society as a whole, but these are “externalized dis-economies” that do not substantially hurt the company itself, at least not economically. Instead, the costs of pollution tend to be carried by society as a whole, and the company is spared the costs. This is particularly true in situations where the industry is critical to the local economy or national priorities, and there is a high tolerance for the damage it causes. One solution would be to “internalize” the external dis-economies by incorporating the costs of clean-up or the estimated costs of environmental damage into the operating costs of the company as a tax. This would give the company a financial incentive to control its costs by reducing its pollution. Virtually no government in any developing country is in a position to do this and to enforce the tax, however.
In practice, capital is rarely available to invest in equipment to control pollution unless there is pressure from government regulation. However, governments are rarely motivated to regulate industry unless there are compelling reasons to do so, and pressure from their citizens. In most developed countries, people are reasonably secure in their health and their lives, and expect a higher quality of life, which they associate with a cleaner environment. Because there is more economic security, these citizens are more willing to accept an apparent economic sacrifice in order to achieve a cleaner environment. However, in order to be competitive in world markets, many developing countries are very reluctant to impose regulation on their industries. Instead, they hope that industrial growth today will lead to a society rich enough tomorrow to clean up the pollution. Unfortunately, the cost of clean-up increases as fast as, or faster than, the costs associated with industrial development. At an early stage of industrial development, a developing country would in theory have very low costs associated with the prevention of pollution, but hardly ever do such countries have the capital resources they need to do so. Later, when such a country does have the resources, the costs are often staggeringly high and the damage has already been done.
Industry in developing countries tends to be less efficient than in developed countries. This lack of efficiency is a chronic problem in developing economies, reflecting untrained human resources, the cost of importing equipment and technology, and the inevitable wastage that occurs when some parts of the economy are more developed than others.
This inefficiency is also based in part on the need to rely on outdated technologies which are freely available, do not require an expensive licence or that do not cost as much to use. These technologies are often more polluting than the state-of-the-art technologies available to industry in developed countries. An example is the refrigeration industry, where the use of chlorofluorocarbons (CFCs) as refrigerant chemicals is much cheaper than the alternatives, despite the serious effects of these chemicals in depleting ozone from the upper atmosphere and thereby reducing the earth’s shield from ultraviolet radiation; some countries had been very reluctant to agree to prohibit the use of CFCs because it would then be economically impossible for them to manufacture and purchase refrigerators. Technology transfer is the obvious solution, but companies in developed countries who developed or hold the licence for such technologies are understandably reluctant to share them. They are reluctant because they spent their own resources developing the technology, wish to retain the advantage they have in their own markets by controlling such technology, and may make their money from using or selling the technology only during the limited term of the patent.
Another problem faced by developing countries is lack of expertise in and awareness of the effects of pollution, monitoring methods and the technology of pollution control. There are relatively few experts in the field in developing countries, in part because there are fewer jobs and a smaller market for their services even though the need may actually be greater. Because the market for pollution control equipment and services may be small, this expertise and technology may have to be imported, adding to the costs. General recognition of the problem by managers and supervisors in industry may be lacking or very low. Even when an engineer, manager or supervisor in industry realizes that an operation is polluting, it may be difficult to persuade others in the company, their bosses or the owners that there is a problem that must be solved.
Industry in most developing countries competes at the low end of international markets, meaning that it produces products that are competitive on the basis of price and not quality or special features. Few developing countries specialize in making very fine grades of steel for surgical instruments and sophisticated machinery, for example. They manufacture lesser grades of steel for construction and manufacturing because the market is much larger, the technical expertise required to produce it is less, and they can compete on the basis of price as long as the quality is good enough to be acceptable. Pollution control reduces the price advantage by increasing the apparent costs of production without increasing output or sales. The central problem in developing countries is how to balance this economic reality against the need to protect their citizens, the integrity of their environment, and their future, realizing that after development the costs will be even higher and the damage may be permanent.
Industrial Pollution in Developing Countries
While industrialization is an essential feature of economic growth in developing countries, industrial practices may also produce adverse environmental health consequences through the release of air and water pollutants and the disposal of hazardous wastes. This is often the case in developing countries, where less attention is paid to environmental protection, environmental standards are often inappropriate or not effectively implemented, and pollution control techniques are not yet fully developed. With rapid economic development, many developing countries, like China and other Asian countries, face some additional environmental problems. One is the environmental pollution from hazardous industries or technologies transferred from developed countries, which are no longer acceptable for occupational and environmental health reasons in developed countries, but still allowable in developing countries due to looser environmental legislation. Another problem is the rapid proliferation of informal small-scale enterprises in townships as well as in rural areas, which often create serious air and water pollution because of lack of sufficient knowledge and funds.
Air Pollution
Air pollution in developing countries is derived not only from stack emission of pollutants from relatively large industries, like iron and steel, non-ferrous metals and petroleum products industries, but also from fugitive emission of pollutants from small-scale factories, such as cement mills, lead refineries, chemical fertilizer and pesticide factories and so on, where inadequate pollution control measures exist and pollutants are allowed to escape to the atmosphere.
Since industrial activities always involve energy generation, the combustion of fossil fuels is a main source of air pollution in the developing countries, where coal is widely used not only for industrial, but also for domestic consumption. For instance, in China, more than 70% of total energy consumption relies on direct coal combustion, from which large amounts of pollutants (suspended particulates, sulphur dioxide, etc.) are emitted under incomplete combustion and inadequate emission controls.
The kinds of air pollutants emitted vary from industry to industry. The concentrations of different pollutants in the atmosphere also vary widely from process to process, and from place to place with different geographic and climatic conditions. It is difficult to estimate specific exposure levels of various pollutants from different industries to the general population in developing countries, as elsewhere. In general, the workplace exposure levels are much higher than that of the general population, because the emissions are rapidly diluted and dispersed by the wind. But the exposure duration of the general population is much longer than that of workers.
The exposure levels of the general population in developing countries are usually higher than that in developed countries, where air pollution is more strictly controlled and resident areas are usually far from industries. As discussed further on in this chapter, a large number of epidemiological studies have already showed the close association of reduction in pulmonary function and increased incidence of chronic respiratory diseases among residents with long-term exposure to the common air pollutants.
A case study of air pollution effects on the health of 480 primary school children in Cubatao, Brazil, where large quantities of mixed pollutants were emitted from 23 industries (steel mill, chemical industries, cement factory, fertilizer plants, etc.), showed that 55.3% of the children had decreases in pulmonary function. Another example of health effects of air pollution appeared in the Ulsan/Onsan special industrial zone, Republic of Korea, where many large-scale plants (mainly petrochemical plants and metal refineries) are concentrated. Local residents complained of a variety of health problems, particularly of the nervous system disorder called “Onsan Disease”.
Accidental releases of toxic substances into the atmosphere resulting in serious health risks are usually more common in developing countries. The reasons include inadequate safety planning, lack of skilled technical personnel to maintain proper facilities, and difficulties in obtaining spare parts and so on. One of the worst of such accidents occurred in Bhopal, India, in 1984, where leaking methyl isocyanide killed 2,000 people.
Water and Soil Pollution
Inappropriate and often careless disposal of industrial wastes—uncontrolled discharge into watercourses and uncontrolled disposal on the land, which often causes water and soil pollution—is another crucial environmental health problem, in addition to industrial air pollution, in developing countries, particularly with numerous small-scale township enterprises, like those in China. Some small-scale factories, such as textile dyeing, pulp and paper, leather tanning, electroplating, fluorescent lamp, lead battery and metal smelting, always produce a large amount of wastes, containing toxic or hazardous substances like chromium, mercury, lead, cyanide and so on, which may pollute the rivers, streams and lakes, and soil as well, when they are untreated. The soil pollution in turn may contaminate groundwater resources.
In Karachi, the Lyan river, which runs through the city, has become an open drain of sewage and untreated industrial effluent from some 300 large and small industries. There is a similar case in Shanghai. Some 3.4 million cubic metres of industrial and domestic waste pour into Suzhou creek and Huangpu river, which flow through the heart of the city. Because of serious pollution, the river and creek have essentially become devoid of life and often produce smells and sights that are unpleasant and offensive to the public living in the surrounding area.
A further problem of water and soil pollution in developing countries is the transfer of toxic or hazardous wastes from developed to developing countries. The cost of transporting these wastes to simple storage sites in developing countries is a mere fraction of the cost required for safely storing or incinerating them in their countries of origin in compliance with the applicable government regulations there. This has occurred in Thailand, Nigeria, Guinea-Bissau and so on. The toxic wastes inside the barrels can leak and pollute the air, water and soil, posing a potential health risk to the people living in the vicinity.
Thus the environmental health problems discussed in this chapter tend to apply to an even greater extent to developing countries.
Food and Agriculture
This article has been prepared by Dr F. Käferstein, Chief, Food Safety, World Health Organization. It is entirely based on the report of a WHO Panel on Food and Agriculture which had supported the WHO Commission on Health and Environment to prepare a report for the United Nations Conference on Environment and Development (UNCED), Rio de Janeiro, 1992. Both reports are available from the WHO.
Production Needs in the Face of Population Pressure and Other Forces
Rapid population growth continues in some regions of the world. As compared with the situation in 1990, by the year 2010 there will be an extra 1,900 million people to be fed, a rise of 36% from 5,300 to 7,200 million people.
Ninety per cent of the entire projected growth over the next 20 years is expected to take place in the countries which are currently classified as developing nations. Progressive urbanization of society is taking place. The urban population of the world will reach 3,600 million, a rise of 62% from the 2,200 million city dwellers in 1990. Moreover the urban population of developing countries will increase by 92% (from 1,400 million to 2,600 million) in the twenty years from 1990, a fourfold increase since 1970. Even if family planning receives the urgent attention that it desperately requires from all rapidly growing populations, population growth and urbanization will continue to dominate the scene for the next two decades.
A 36% increase in food, other agricultural products and potable water will be required over the next twenty years simply to match the rise in population; the need for half a billion people to be properly fed instead of remaining undernourished, and the greater demand from populations with a rising income, will all lead to a vast increase in total food production. An excessive demand for food of animal origin will continue to characterize people in the higher income groups, leading to increases in animal feed production.
The pressure on agriculture and food production, as both population and per capita demand increase, will lead to a greater burden on the environment. This burden will be unevenly generated and have uneven environmental effects. Globally, these will be adverse and will require concerted action.
This increased demand will fall on resources of land and water which are finite, where the most productive areas have already been used, and where the cost of bringing marginal land into production, and of using less readily available water, will be high. Much of this marginal land may have only temporary fertility unless specific measures are taken to maintain it, while the productivity of natural fisheries is also sharply limited. The area of arable land will decrease due to soil erosion from over-grazing; laterization of clearfelled areas; soil salinization and other types of land degradation; and the expansion of urban, industrial and other developments.
Water availability and quality, already totally inadequate in much of the world, will remain major problems for rural areas of developing countries and also for many urban populations, who may face the additional problem of high utilization charges. Needs for water will increase greatly, and for several large cities the meeting of water demands will become increasingly costly as supplies will have to be brought from far away. Re-use of water implies more stringent standards for treatment. The increasing production of wastewater and sewage will require more extensive treatment facilities, as well as large outlays of capital.
The continuing long-term need for industrial development to produce goods, services and employment will lead to more intensive food production, which will itself become more industrialized. Consequently, and especially because of urbanization, the demand for, and the resources employed in, packaging, processing, storage and distribution of food will increase in volume and importance.
The public is becoming much more aware of the need to produce, protect and market food in ways which minimize adverse change in our environment, and is more demanding in this respect. The emergence of revolutionary scientific tools (e.g., biotechnological advances) offers the possibility of significantly increasing food production, reducing waste and enhancing safety.
The principal challenge is to meet the increasing demands for food, other agricultural products and water in ways that foster long-term improvements in health, and which are also sustainable, economical and competitive.
Despite the fact that globally there is at present sufficient food for all, great difficulties have to be overcome to ensure the availability and equitable distribution of safe, nutritious and affordable food supplies to meet health needs in many parts of the world, and notably in areas of rapid population growth.
There is often a failure to take the possible health consequences fully into account in the design and implementation of agricultural and fisheries policies and programmes. An example is the production of tobacco, which has very serious and negative impacts on human health and on scarce land and fuelwood resources. Moreover, the lack of an integrated approach to development of the agriculture and forestry sectors results in failure to recognize the important relationship of both sectors to the protection of wildlife habitats, biological diversity and genetic resources.
If timely and appropriate action is not taken to mitigate the environmental impacts of agriculture, fisheries, food production and water use, then the following situations will prevail:
- As the urban population increases, the difficulty of maintaining and extending an efficient food distribution system will become greater. This may increase the prevalence of household food insecurity, associated malnutrition and health risks among the growing masses of urban poor.
- Microbial, viral and parasitic diseases from contaminated food and water will continue to be serious health problems. New agents of public health importance will continue to emerge. The diarrhoeal diseases related to food and water, causing high infant mortality and universal morbidity, will increase.
- Vector-borne diseases from irrigation, other water resource developments, and uncontrolled wastewater will increase substantially. Malaria, schistosomiasis, filariasis and arbovirus fevers will continue to be major problems.
- The problems outlined above will be reflected in static or rising levels of infant and young child malnutrition and mortality, as well as morbidity at all ages, but predominantly among the poor, the very young, the aged and the sick.
- diseases linked to inappropriate life-styles, smoking and diet (for example, obesity, diabetes or coronary heart disease), which are characteristic of the more affluent countries, are now emerging and becoming significant problems also in developing countries. The increasing urbanization will accelerate this trend.
- As the intensity of food production increases, the risk of occupational diseases and accidents among those working in this and related sectors will increase substantially unless sufficient efforts for safety and prevention are made.
Health Consequences of Biological Contamination and Chemicals in Food
Despite progress in science and technology, contaminated food and water remain to this day major public health problems. Foodborne diseases are perhaps the most widespread health problems in the contemporary world and important causes of reduced economic productivity (WHO/FAO 1984). They are caused by a wide range of agents, and cover all degrees of severity, from mild indispositions to life-threatening illnesses. However, only a small proportion of cases comes to the notice of health services and even fewer are investigated. As a result, it is believed that in industrialized countries only approximately 10% of the cases are reported, whilst in developing countries reported cases probably account for not more than 1% of the total.
Despite these limitations, the data that are available indicate that foodborne diseases are increasing all over the world, both in developing and industrialized countries. Experience in Venezuela illustrates this trend (PAHO/WHO 1989) (figure 1).
Figure 1. Foodborne diseases in Venezuela
Developing countries
Available information clearly indicates that biological contaminants (bacteria, viruses and parasites) are the major causes of foodborne diseases (table 1).
Table 1. Some agents of important foodborne diseases and salient epidemiological features
|
Agents |
Important reservoir/carrier |
Transmissiona by |
Multiplication |
Examples of some incriminated foods |
||
|
Water |
Food |
Person to person |
||||
|
Bacteria |
||||||
|
Baccillus cereus |
Soil |
- |
+ |
- |
+ |
Cooked rice, cooked meats, vegetables, |
|
Brucella species |
Cattle, goats, sheep |
- |
+ |
- |
+ |
Raw milk, dairy products |
|
Campylobacter jejuni |
Chickens, dogs, cats, cattle, |
+ |
+ |
+ |
-b |
Raw milk, poultry |
|
Clostridium botulinum |
Soil, mammals, birds, fish |
- |
+ |
- |
+ |
Fish, meat, vegetables (home preserved), |
|
Clostridium perfringens |
Soil, animals, humans |
- |
+ |
- |
+ |
Cooked meat and poultry, gravy, beans |
|
Escherichia coli |
||||||
|
Enterotoxigenic |
Humans |
+ |
+ |
+ |
+ |
Salad, raw vegetables |
|
Enteropathogenic |
Humans |
+ |
+ |
+ |
+ |
Milk |
|
Enteroinvasive |
Humans |
+ |
+ |
0 |
+ |
Cheese |
|
Enterohaemorrhagic |
Cattle, poultry, sheep |
+ |
+ |
+ |
+ |
Undercooked meat, raw milk, cheese |
|
Listeria monocytogenes |
Environment |
+ |
+ |
-c |
+ |
Cheese, raw milk, coleslaw |
|
Mycobacterium bovis |
Cattle |
- |
+ |
- |
- |
Raw milk |
|
Salmonella typhi and |
Humans |
+ |
+ |
± |
+ |
Dairy products, meat products, shellfish, |
|
Salmonella (non-typhi) |
Humans and animals |
± |
+ |
± |
+ |
Meat, poultry, eggs, dairy products, |
|
Shigella spp. |
Humans |
+ |
+ |
+ |
+ |
Potato/egg salads |
|
Staphylococcus aureus |
- |
+ |
- |
+ |
Ham, poultry and egg salads, cream-filled |
|
|
Vibrio cholerae, 01 |
Humans, marine life |
+ |
+ |
± |
+ |
Salad, shellfish |
|
Vibrio cholerae, non-01 |
Humans, marine life |
+ |
+ |
± |
+ |
Shellfish |
|
Vibrio parahaemolyticus |
Sea water, marine life |
- |
+ |
- |
+ |
Raw fish, crabs, and other shellfish |
|
Vibrio vulnificus |
Sea water, marine life |
+ |
+ |
- |
+ |
Shellfish |
|
Yersinia enterocolitica |
Water, wild animals, pigs, |
+ |
+ |
- |
+ |
Milk, pork, and poultry |
|
Viruses |
||||||
|
Hepatitis A virus |
Humans |
+ |
+ |
+ |
- |
Shellfish, raw fruit and vegetables |
|
Norwalk agents |
Humans |
+ |
+ |
- |
- |
Shellfish, salad |
|
Rotavirus |
Humans |
+ |
+ |
+ |
- |
0 |
|
Protozoa |
+ |
+ |
+ |
+ |
||
|
Cryptosporidium parvum |
Humans, animals |
+ |
+ |
+ |
- |
Raw milk, raw sausage (non-fermented) |
|
Entamoeba histolytica |
Humans |
+ |
+ |
+ |
- |
Vegetables and fruits |
|
Giardia lamblia |
Humans, animals |
+ |
± |
+ |
- |
Vegetables and fruits |
|
Toxoplasma gondii |
Cats, pigs |
0 |
+ |
- |
- |
Undercooked meat, raw vegetables |
|
Helminths |
||||||
|
Ascaris lumbricoides |
Humans |
+ |
+ |
- |
- |
Soil-contaminated food |
|
Clonorchis sinensis |
Freshwater fish |
- |
+ |
- |
- |
Undercooked/raw fish |
|
Fasciola hepatica |
Cattle, goats |
+ |
+ |
- |
- |
Watercress |
|
Opisthorclis viverrini/felinus |
Freshwater fish |
- |
+ |
- |
- |
Undercooked/raw fish |
|
Paragonimus sp. |
Freshwater crabs |
- |
+ |
- |
- |
Undercooked/raw crabs |
|
Taenia saginata and T. solium |
Cattle, swine |
- |
+ |
- |
- |
Undercooked meat |
|
Trichinella spiralis |
Swine, carnivora |
- |
+ |
- |
- |
Undercooked meat |
|
Trichuris trichiura |
Humans |
0 |
+ |
- |
- |
Soil-contaminated food |
a Almost all acute enteric infections show increased transmission during the summer and/or wet months, except infections due to Rotavirus and Yersinia enterocolitica, which show increased transmission in cooler months.
b Under certain circumstances, some multiplication has been observed. The epidemiological significance of this observation is not clear.
c Vertical transmission from pregnant woman to foetus occurs frequently.
+ = Yes; ± = Rare; - = No; 0 = No information.
Adapted from WHO/FAO 1984.
In the developing countries, they are responsible for a wide range of foodborne diseases (e.g., cholera, salmonellosis, shigellosis, typhoid and paratyphoid fevers, brucellosis, poliomyelitis and amoebiasis). Diarrhoeal diseases, especially infant diarrhoea, are the dominant problem and indeed one of massive proportions. Annually, some 1,500 million children under the age of five suffer from diarrhoea and of these over three million die as a result. Formerly it was thought that contaminated water supplies were the main direct source of pathogens causing diarrhoea, but now it has been shown that up to 70% of diarrhoeal episodes may be due to foodborne pathogens (WHO 1990c). However, the contamination of the food may in many cases originate from contaminated water that is used for irrigation and similar purposes.
Industrialized countries
Although the situation regarding foodborne diseases is very serious in developing countries, the problem is not limited to these countries, and in recent years, industrialized countries have experienced a succession of major epidemics. In the United States it is estimated there are 6.5 million cases per year, with 9,000 fatalities, but according to the US Food and Drug Administration this figure is an underestimate and may be as high as 80 million cases (Cohen 1987; Archer and Kvenberg 1985; Young 1987). The estimate for former West Germany was one million cases in 1989 (Grossklaus 1990). A study in the Netherlands found that as many as 10% of the population may be affected by foodborne or waterborne diseases (Hoogenboom-Vergedaal et al. 1990).
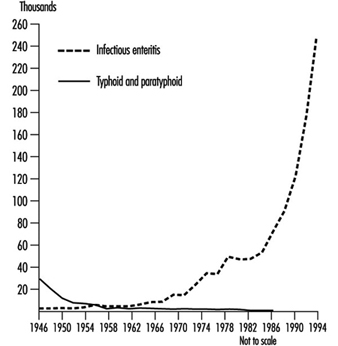
With today’s improvements in standards of personal hygiene, development of basic sanitation, safe water supplies, effective infrastructure and the increasing application of technologies such as pasteurization, many foodborne diseases have been either eliminated or considerably reduced in certain industrialized countries (e.g., milkborne salmonellosis). Nevertheless, most countries are now experiencing an important increase in several other foodborne diseases. The situation in former West Germany (1946-1991) illustrates this phenomenon (figure 2) (Statistisches Bundesamt 1994).
Figure 2. Infectious enteritis, typhoid fever and para-typhoid fever (A, B and C), Germany
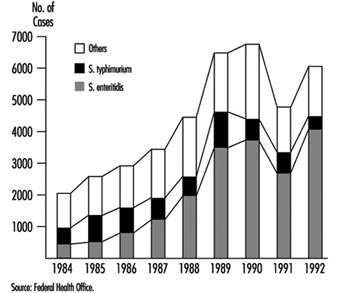
Salmonellosis, specifically, has increased tremendously on both sides of the Atlantic over the past few years (Rodrigue 1990). In many cases it is due to Salmonella enteritidis. Figure 3 shows the increase of this micro-organism in relation to other Salmonella strains in Switzerland. In many countries, poultry meat, eggs and foods containing eggs have been identified as the predominant sources of this pathogen. In certain countries, 60 to 100% of poultry meat is contaminated with Salmonella spp., and meat, frogs’ legs, chocolate and milk have also been implicated (Notermans 1984; Roberts 1990). In 1985, some 170,000 to 200,000 persons were involved in an outbreak of salmonellosis in Chicago which was caused by contaminated pasteurized milk (Ryzan 1987).
Figure 3. Serotypes of Salmonella in Switzerland
Chemicals and toxicants in food
Considerable efforts have been undertaken at the national and international levels to ensure the chemical safety of food supplies. Two joint FAO/WHO committees have, over a period of three decades, evaluated a large number of food chemicals. The Joint FAO/WHO Expert Committee on Food Additives (JECFA) evaluates food additives, contaminants and veterinary drug residues, and the Joint FAO/WHO Meeting on Pesticide Residues (JMPR) evaluates pesticide residues. Recommendations are made on the acceptable daily intake (ADI), on maximum residue levels (MRLs) and maximum levels (MLs). Based on these recommendations, the Codex Alimentarius Commission and governments establish food standards and safe levels for these substances in foodstuffs. Moreover, the Joint UNEP/FAO/WHO Food Contamination Monitoring Programme (GEMS/Food) provides information on the levels of contaminants in food and on time trends of contamination, enabling preventive and control measures.
While information from most of the developing countries is scarce, surveys made in the industrialized countries suggest that the food supply is largely safe from the chemical viewpoint owing to the extensive food safety infrastructure (i.e., legislation, enforcement mechanisms, surveillance and monitoring systems) and the general level of responsibility of the food industry. However, accidental contamination or adulteration does occur, in which case the health consequences may be grave. For example, in Spain in 1981-82, adulterated cooking oil killed some 600 people and disabled—temporarily or permanently—another 20,000 (WHO 1984). The agent responsible for this mass poisoning has not yet been identified in spite of intensive investigations.
Environmental chemicals
A number of chemical substances may occur in the food supply as a result of environmental contamination. Their effects on health may be extremely serious and have caused great concern in recent years.
Serious consequences have been reported when foods contaminated with heavy metals such as lead, cadmium or mercury have been ingested over extended periods of time.
The Chernobyl accident provoked great concern over the health risks to people exposed to accidental radionuclide emissions. People living in the vicinity of the accident were exposed, and this exposure included radioactive contaminants in food and water. In other parts of Europe and elsewhere, at some distance from the accident, this concern focused on contaminated foods as a source of exposure. In most countries, the estimated average dose acquired from eating contaminated foods amounted to only a very small fraction of the dose normally received from background radiation (IAEA 1991).
Other environmental chemicals of interest are polychlorinated biphenyls (PCBs). PCBs are used in various industrial applications. Information on the effects of PCBs on human health were originally noted following from two large-scale incidents which occurred in Japan (1968) and in Taiwan, China (1979). Experience from these outbreaks showed that as well as their acute effects, PCBs may also have carcinogenic effects.
DDT was widely used between 1940 and 1960 as an insecticide for agricultural purposes and for the control of vector-borne diseases. It is now banned or restricted in many countries because of its potential risk to the environment. In many tropical countries, DDT is still an important chemical, used for the control of malaria. No confirmed ill effects have been reported due to residues of DDT in food (UNEP 1988).
Mycotoxins
Mycotoxins, the toxic metabolites of certain microscopic fungi (moulds), may cause serious adverse effects in humans, as well as in animals. Animal studies have shown that besides acute intoxication, mycotoxins are capable of causing carcinogenic, mutagenic and teratogenic effects.
Biotoxins
Intoxication by marine biotoxin (also known as “fish poisoning”) is another problem of concern. Examples of such intoxications are ciguatera and various kinds of shellfish poisoning.
Plant toxicants
Toxicants in edible plants and poisonous plants which resemble them (mushrooms, certain wild green plants) are important causes of ill health in many areas of the world and present a troublesome problem for food safety (WHO 1990b).
Linkages Between Environmental and Occupational Health
Development, and industrialization in particular, have made immense positive contributions to health, including greater personal and social wealth, as well as vastly improved health and education services, transportation and communication. Unquestionably, on the global scale, people are living longer and are healthier than they were centuries and even decades ago. However, industrialization has also had adverse health consequences not only for workforces, but for the general population as well. These effects have been caused either directly by exposure to safety hazards and harmful agents, or indirectly through environmental degradation locally and globally (see “Industrial pollution in developing countries” in this chapter).
This article outlines the nature of environmental health hazards and the reasons for linking environmental health with occupational health.
Environmental health hazards, like occupational health hazards, may be biological, chemical, physical, biomechanical or psychosocial in nature. Environmental health hazards include traditional hazards of poor sanitation and shelter, as well as agricultural and industrial contamination of air, water, food and land. These hazards have resulted in a host of health impacts, ranging from catastrophic direct effects (e.g., the recent cholera epidemic in Latin America and the chemical poisoning outbreak in Bhopal, India), to chronic effects (e.g., in Minamata, Japan), to subtle, indirect, and even disputed effects (e.g., in Love Canal, USA). Table 1 summarizes some of the major notorious disasters in the last half century that have caused “environmental disease” outbreaks. There are undeniably countless other examples of environmental disease outbreaks, some of which are not easily detectable on the macrostatistical level. Meanwhile, over a billion people in the world lack access to safe drinking water (WHO 1992b) and over 600 million are exposed to ambient levels of sulphur dioxide that well exceed recommended levels. Moreover the pressure on agriculture and food production as both population and per capita demand increase, will likely lead to a greater burden on the environment (see “Food and agriculture” in this chapter). Environmental health impacts thus include the indirect effects of industrial disruption of adequate food and housing, as well as the degradation of the global systems on which the health of the planet depends.
Table 1. Selected major "environmental disease" outbreaks
|
Location and year |
Environmental hazard |
Type of disease |
Number affected |
|
London, UK 1952 |
Severe air-pollution with sulphur dioxide and suspended particulate matter (SPM) |
Increase in heart and lung disease manifestations |
3,000 deaths, many others ill |
|
Toyama, Japan 1950s |
Cadmium in rice |
Kidney and bone disease (“Itai-itai disease”) |
200 with severe disease, many more with slight effects |
|
South-east Turkey 1955-61 |
Hexachlorobenzene in seed grains |
Porphyria; neurological disease |
3,000 |
|
Minamata, Japan 1956 |
Methylmercury in fish |
Neurological disease (“Minimata disease”) |
200 with severe disease, 2,000 suspected |
|
USA cities 1960s-70s |
Lead in paint |
Anaemia, behavioural and mental effects |
Many thousands |
|
Fukuoka, Japan 1968 |
Polychlorinated biphenyls (PCBs) in food oil |
Skin disease, general weakness |
Several thousands |
|
Iraq 1972 |
Methylmercury in seed grains |
Neurological disease |
500 deaths, 6,500 hospitalized |
|
Madrid, Spain 1981 |
Aniline or other toxin in food oil |
Various symptoms |
340 deaths, 20,000 cases |
|
Bhopal, India 1985 |
Methylisocyanate |
Acute lung disease |
2,000 deaths, 200,000 poisoned |
|
California, USA 1985 |
Carbamate pesticide in watermelons |
Gastrointestinal, skeletal, muscle, autonomic and central nervous system effects (Carbamate illness) |
1,376 reported cases of illness resulting from consumption, 17 severely ill |
|
Chernobyl, USSR 1986 |
Iodine-134, Caesium-134 and -137 from a reactor explosion |
Radiation illness (including increases in cancer and thyroid diseases in children) |
300 injured, 28 died within 3 months, more than 600 cases of thyroid cancer |
|
Goiánia, Brazil 1987 |
Caesium-137 from an abandoned cancer therapy machine |
Radiation illness (follow-up of in utero exposures continuing) |
Some 240 people were contaminated and 2 died |
|
Peru 1991 |
Cholera epidemic |
Cholera |
139 deaths, many thousand ill |
In many countries large-scale agriculture and the concomitant active use of toxic pesticides is a major health hazard both for workers and for their households. Pollution by fertilizers or biological waste from the food industry, paper industry and so on can also have harmful effects on waterways, reducing fishing and food supplies. The fishermen and gatherers of other seafood may have to travel much further to get their daily catch, with increased risks of drowning accidents and other mishaps. The spread of tropical disease by the environmental changes associated with developments such as the building of dams, roads and so on constitutes another type of environmental health risk. The new dam may create breeding grounds for schistosomiasis, a debilitating disease affecting rice farmers who have to walk in water. The new road may create fast communication between an area with endemic malaria and another area hitherto spared from this disease.
It should be pointed out that the major basis for a harmful environment in the workplace or in the general environment is poverty. The traditional health threats in developing countries or in poor sections of any country include poor sanitation, water and food which spreads communicable diseases, poor housing with high exposures to cooking smoke and high fire risks, as well as high injury risks in small-scale agriculture or cottage industries. Reduction of poverty and improved living and working conditions is a fundamental priority for improved occupational and environmental health for billions of people. Despite efforts for energy conservation and sustainable development, failure to address the underlying inequities in wealth distribution threatens the global ecosystem.
Forests, for example, which represent the culmination of ecological successional processes, are being destroyed at an alarming rate, due to commercial logging and clearance by impoverished peoples for agriculture and firewood. The effects of forest depletion include soil erosion, which, if extreme, can lead to desertification. Loss of biodiversity is an important consequence (see “Species extinction, biodiversity loss and human health” in this chapter). It is estimated that one-third of all carbon dioxide emissions are from the burning of tropical forests (the importance of carbon dioxide in creating global warming is discussed in “Global climate change and ozone depletion” in this chapter). Thus, addressing poverty is imperative with respect to global environmental health as well as individual, community and regional well-being.
Reasons for Linking Environmental and Occupational Health
The main link between the workplace and the general environment is that the source of the hazard is usually the same, whether it is an agricultural activity or an industrial activity. In order to control the health hazard, a common approach may work effectively in both settings. This is particularly so when it comes to the choice of chemical technologies for production. If an acceptable result or product can be produced with a less toxic chemical, the choice of such a chemical can reduce or even eliminate the health risk. One example is the use of safer water-based paints instead of paints made with toxic organic solvents. Another example is the choice of non-chemical pest-control methods whenever this is possible. In fact, in many cases, particularly in the developing world, there is no separation between the home and the workplace; thus the setting is truly the same.
It is now well recognized that the scientific knowledge and training required to assess and control environmental health hazards are, for the most part, the same skills and knowledge required to address health hazards within the workplace. Toxicology, epidemiology, occupational hygiene, ergonomics, safety engineering - in fact, the very disciplines included in this Encyclopaedia - are the basic tools of environmental science. The process of risk assessment and risk management is also the same: identify the hazards, categorize the risks, assess the exposure and estimate risk. This is followed by evaluating control options, controlling the exposure, communicating the risk to the public and establishing an on-going exposure- and risk-monitoring programme. Thus occupational and environmental health are strongly linked by common methodologies, particularly in health assessment and exposure control.
The identification of environmental health hazards has often come from observations of adverse health outcomes among workers; and unquestionably it is in the workplace that the impact of industrial exposures is best understood. Documentation of health effects generally comes from one of three sources: animal or other laboratory experiments (both non-human and controlled human), accidental high-level exposures or the epidemiological studies that usually follow such exposures. To conduct an epidemiological study it is necessary to be able to define both the exposed population and the nature and level of the exposure, as well as to ascertain the negative health effect. It is generally easier to define the members of a workforce than to determine the membership of a community, particularly in a community that is transient; the nature and level of exposure to various members of the cohort are generally more clear-cut in a workplace population than in a community; and the outcomes of high levels of exposure are almost always easier to delineate than more subtle changes attributable to low-level exposure. While there are some examples of exposure outside factory gates approaching the worst occupational exposures (e.g., cadmium exposure from mining in China and Japan; lead and cadmium emissions from smelters in Upper Silesia, Poland), the levels of exposure are generally much higher to a workforce than to the surrounding community (WHO 1992b).
Since adverse health outcomes are more apparent in workers, information on occupational health effects of many toxic exposures (including heavy metals such as lead, mercury, arsenic and nickel, as well as such well-known carcinogens as asbestos) has been used to calculate the health risk to the wider community. With respect to cadmium, for example, as early as 1942 reports began to appear of cases of osteomalacia with multiple fractures among workers in a French factory producing alkaline batteries. During the 1950s and 1960s cadmium intoxication was considered to be strictly an occupational disease. However, the knowledge gained from the workplace helped achieve the recognition that osteomalacia and kidney disease that was occurring in Japan at this time, “Itai-itai” disease, was indeed due to contamination of rice from irrigation of soil with water contaminated with cadmium from industrial sources (Kjellström 1986). Thus occupational epidemiology has been able to make a substantive contribution to knowledge of the effects of environmental exposure, constituting another reason for linking the two fields.
On an individual level, occupational disease affects well-being in the home and the community; and, universally, an individual who is ill from inadequacies in the home and the community cannot be productive in the workplace.
Strictly from a scientific viewpoint, there is a need to consider total (environmental plus occupational) exposures in order to truly assess health impact and establish dose-response relationships. Pesticide exposure is a classic example wherein occupational exposure may be supplemented by considerable environmental exposure, through food and water-source contamination, and through non-occupational airborne exposure. From outbreaks in which over 100 poisonings occurred from contaminated food alone, over 15,000 cases and 1,500 deaths due to pesticide poisoning have been documented by the WHO (1990e). In one study of Central American cotton growers using pesticides, not only did very few of the workers have access to protective clothing, but virtually all of the workers lived within 100 metres of the cotton fields, many in temporary housing with no walls for protection from aerial pesticide spraying. The workers also often washed in irrigation channels containing pesticide residues, resulting in increased exposures (Michaels, Barrera and Gacharna 1985). To understand the relationship between pesticide exposure and any health effects reported, all sources of exposure should be taken into consideration. Thus ensuring that occupational and environmental exposures are evaluated together improves the accuracy of exposure assessment in both areas.
The health problems caused by occupational and environmental hazards are particularly acute in developing countries, where well established methods of hazard control are less likely to be applied because of limited awareness of the hazards, low political priority of health and environment matters, limited resources or lack of appropriate occupational and environmental health management systems. A major impediment to environmental health hazard control in many parts of the world is the lack of people with appropriate training. It has been documented that developing countries suffer from a severe shortage of expert staff in occupational health (Noweir 1986). In 1985 a WHO expert committee also concluded that there is an urgent need for staff trained in environmental health matters; indeed Agenda 21, the internationally agreed upon strategy taken by the United Nations Conference on Environment and Development (UN 1993), identifies training (national “capacity building”) as a key element of promoting human health through sustainable development. Where resources are limited, it is not feasible to train one group of people to look after health concerns within the workplace, and another group to attend to hazards outside the factory gate.
Even in developed countries, there is a strong trend to make most efficient use of resources by training and employing “occupational and environmental health” professionals. Today, businesses must find ways to manage their affairs logically and efficiently within the societal framework of duty, law and financial policy. Combining occupational and environment health under one roof is one way of achieving this goal.
Broad environmental concerns must be taken into consideration in designing workplaces and deciding on industrial hygiene control strategies. Substituting for one substance another one that is less acutely toxic may make good occupational health sense; however, if the new substance is not biodegradable, or damages the ozone layer, it would not be an appropriate exposure control solution—it would only move the problem elsewhere. The use of chlorofluorocarbons, now widely used as a refrigerant instead of the more acutely dangerous substance ammonia, is the classic example of what is now known to have been an environmentally inappropriate substitution. Thus linking occupational and environmental health minimizes unwise exposure control decisions.
While understanding of the health effects of various deleterious exposures has usually come from the workplace, the public health impact of environmental exposures to these same agents has often been a major force in stimulating clean-up efforts both inside the workplace and in the surrounding community. For example, discovery of high lead levels in workers’ blood by an industrial hygienist in a lead foundry in Bahia, Brazil, led to investigations of lead in the blood of children in nearby residential areas. The finding that the children had high lead levels was a major impetus in the company taking action to reduce occupational exposures as well as lead emissions from the factory (Nogueira 1987), although occupational exposures still remain substantially higher than would be tolerated by the general community.
In fact, environmental health standards are usually much stricter than occupational health standards. The WHO’s recommended guideline values for selected chemicals provide an example. The rationale for the difference is generally that the community consists of sensitive populations including the very old, the ill, young children and pregnant women, whereas the workforce is at least healthy enough to work. Also, it is often argued that risk is more “acceptable” to a workforce, as these people are benefiting by having a job, and are therefore more willing to accept the risk. Many political, ethical, as well as scientific, debates rage around the question of standards. Linking occupational and environmental health can be a positive contribution to sorting out these controversies. In this regard, tightening the connection between occupational and environmental health may facilitate greater consistency in approaches to standard setting.
Likely inspired at least in part by the active debate about the environment and sustainable development brought to the forefront by Agenda 21, many occupational health professional organizations have changed their names to “occupational and environmental” organizations in acknowledgement that their members are increasingly devoting their attention to environmental health hazards both inside and outside the workplace. Further, as noted in the chapter on ethics , the International Code of Ethics for Occupational Health Professionals states that the duty to protect the environment is part and parcel of the ethical obligations of occupational health professionals.
In summary, occupational and environmental health are strongly linked by:
- the very fact that the source of the health threat is usually the same
- common methodologies, particularly in health assessment and exposure control
- the contribution that occupational epidemiology makes to knowledge of the effects of environmental exposure
- the effects that occupational disease has on well-being in the home and the community, and conversely the effect of environmental pathology on worker productivity
- the scientific need to consider total exposures in order to determine dose-response relationships
- the efficiency in human resource development and utilization gained by such a linkage
- improvements in exposure control decisions stemming from the broader view
- greater consistency in standard setting facilitated by the link
- the fact that linking environmental and occupational health enhances the incentive for rectification of hazards to both the workforce and the community.
The desirability of bringing together occupational and environmental health notwithstanding, each has a unique and specific orientation that should not be lost. Occupational health must continue to focus on workers’ health, and environmental health must continue to concern itself with the health of the general public. None the less, even where it is desirable for professionals to operate strictly in only one of these fields, having a good appreciation of the other enhances the credibility, knowledge base and effectiveness of the overall endeavour. It is in this spirit that this chapter is presented.
Multiple Chemical Sensitivities
Introduction
Since the 1980s, a new clinical syndrome has been described in occupational and environmental health practice characterized by the occurrence of diverse symptoms after exposure to low levels of artificial chemicals, although as yet it lacks a widely accepted definition. The disorder may develop in individuals who have experienced a single episode, or recurring episodes of a chemical injury such as solvent or pesticide poisoning. Subsequently, many types of environmental contaminant in air, food or water may elicit a wide range of symptoms at doses below those which produce toxic reactions in others.
Although there may not be measurable impairment of specific organs, the complaints are associated with dysfunction and disability. Although idiosyncratic reactions to chemicals are probably not a new phenomenon, it is believed that multiple chemical sensitivities (MCSs), as the syndrome is now most frequently called, is being brought by patients to the attention of medical practitioners far more commonly than in the past. This syndrome is prevalent enough to have generated substantial public controversy as to who should treat patients suffering with the disorder and who should pay for the treatment, but research has yet to elucidate many scientific issues relevant to the problem, such as its cause, pathogenesis, treatment and prevention. Despite this, MCS clearly does occur and causes significant morbidity in the workforce and general population. It is the purpose of this article to elucidate what is known about it at this time in the hope of enhancing its recognition and management in the face of uncertainty.
Definition and Diagnosis
Although there is no general consensus on a definition for MCS, certain features allow it to be differentiated from other well-characterized entities. These include the following:
- Symptoms typically occur after a definitely characterizable occupational or environmental incident, such as an inhalation of noxious gases or vapours or other toxic exposure. This “initiating” event may be a single episode, such as an exposure to a pesticide spray, or a recurrent one, such as frequent solvent overexposure. Often the effects of the apparently precipitating event, or events, are mild and may merge without clear demarcation into the syndrome which follows.
- Acute symptoms similar to those of the preceding exposure begin to occur after re-exposures to lower levels of various materials, such as petroleum derivatives, perfumes and other common work and household products.
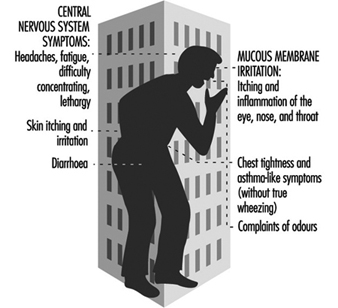
- Symptoms are referrable to multiple organ systems. Central nervous system complaints, such as fatigue, confusion and headache, occur in almost every case. Upper and lower respiratory, cardiac, dermal, gastrointestinal and musculoskeletal symptoms are common.
- It is generally the case that very diverse agents may elicit the symptoms at levels of exposure orders of magnitude below accepted TLVs or guidelines.
- Complaints of chronic symptomatology, such as fatigue, cognitive difficulties, gastrointestinal and musculoskeletal disturbances are common. Such persistent symptoms may predominate over reactions to chemicals in some cases.
- Objective impairment of the organs which would explain the pattern or intensity of complaints is typically absent. Patients examined during acute reactions may hyperventilate or demonstrate other manifestations of excess sympathetic nervous system activity.
- No better established diagnosis easily explains the range of responses or symptoms.
While not every patient precisely meets the criteria, each point should be considered in the diagnosis of MCS. Each serves to rule out other clinical disorders which MCS may resemble, such as somatization disorder, sensitization to environmental antigens (as with occupational asthma), late sequelae of organ system damage (e.g., reactive airways dysfunction syndrome after a toxic inhalation) or a systemic disease (e.g., cancer). On the other hand, MCS is not a diagnosis of exclusion and exhaustive testing is not required in most cases. While many variations occur, MCS is said to have a recognizable character which facilitates diagnosis as much or more than the specific criteria themselves.
In practice, diagnostic problems with MCS occur in two situations. The first is with a patient early in the course of the condition in whom it is often difficult to distinguish MCS from the more proximate occupational or environmental health problem which precedes it. For example, patients who have experienced symptomatic reactions to pesticide spraying indoors may find that their reactions are persisting, even when they avoid direct contact with the materials or spraying activities. In this situation a clinician might assume that significant exposures are still occurring and direct unwarranted effort to altering the environment further, which generally does not relieve the recurrent symptoms. This is especially troublesome in an office setting where MCS may develop as a complication of sick building syndrome. Whereas most office workers will improve after steps are taken to improve air quality, the patient who has acquired MCS continues to experience symptoms, despite the lower exposures involved. Efforts to improve the air quality further typically frustrate patient and employer.
Later in the course of MCS, diagnostic difficulty occurs because of the chronic aspects of the illness. After many months, the MCS patient is often depressed and anxious, as are other medical patients with new chronic diseases. This may lead to an exaggeration of psychiatric manifestations, which may predominate over chemically stimulated symptoms. Without diminishing the importance of recognizing and treating these complications of MCS, nor even the possibility that MCS itself is psychological in origin (see below), the underlying MCS must be recognized in order to develop an effective mode of management which is acceptable to the patient.
Pathogenesis
The pathogenic sequence which leads in certain people from a self-limited episode or episodes of an environmental exposure to the development of MCS is not known. There are several current theories. Clinical ecologists and their adherents have published extensively to the effect that MCS represents immune dysfunction caused by accumulation in the body of exogenous chemicals (Bell 1982; Levin and Byers 1987). At least one controlled study did not confirm immune abnormalities (Simon, Daniel and Stockbridge 1993). Susceptibility factors under this hypothesis may include nutritional deficiencies (e.g., lack of vitamins or antioxidants) or the presence of subclinical infections such as candidiasis. In this theory, the “initiating” illness is important because of its contribution to lifelong chemical overload.
Less well developed, but still very biologically oriented, are the views that MCS represents unusual biological sequelae of chemical injury. As such, the disorder may represent a new form of neurotoxicity due to solvents or pesticides, injury to the respiratory mucosae after an acute inhalational episode or similar phenomena. In this view, MCS is seen as a final common pathway of different primary disease mechanisms (Cullen 1994; Bascom 1992).
A more recent biological perspective has focused on the relationship between the mucosae of the upper respiratory tract and the limbic system, especially with respect to the linkage in the nose (Miller 1992). Under this perspective, relatively small stimulants to the nasal epithelium could produce an amplified limbic response, explaining the dramatic, and often stereotypic, responses to low-dose exposures. This theory also may explain the prominent role of highly odoriferous materials, such as perfumes, in triggering responses in many patients.
Conversely, however, many experienced investigators and clinicians have invoked psychological mechanisms to explain MCS, linking it to other somatoform disorders (Brodsky 1983; Black, Ruth and Goldstein 1990). Variations include the theory that MCS is a variant of post-traumatic stress disorder (Schottenfeld and Cullen 1985) or a conditioned response to an initial toxic experience (Bolle-Wilson, Wilson and Blecker 1988). One group has hypothesized MCS as a late-life response to early childhood traumas such as sexual abuse (Selner and Strudenmayer 1992). In each of these theories, the precipitating illness plays a more symbolic than biological role in the pathogenesis of MCS. Host factors are seen as very important, especially the predisposition to somaticize psychological distress.
Although there is much published literature on the subject, few clinical or experimental studies have appeared to support strongly any of these views. Investigators have not generally defined their study populations nor compared them with appropriately matched groups of control subjects. Observers have not been blinded to subject status or research hypotheses. As a result, most available data are effectively descriptive. Furthermore, the legitimate debate over the aetiology of MCS has been distorted by dogma. Since major economic decisions (e.g., patient benefit entitlements and physician reimbursement acceptance) may hinge upon the way in which cases are viewed, many physicians have very strong opinions about the illness, which limit the scientific value of their observations. Caring for MCS patients requires a recognition of the fact that these theories are often well known to patients, who may also have very strong views on the matter.
Epidemiology
Detailed knowledge of the epidemiology of MCS is not available. Estimates of its prevalence in the US population (from where most reports continue to come) range as high as several percentage points, but the scientific basis for these is obscure, and other evidence exists to suggest that MCS in its clinically apparent form is rare (Cullen, Pace and Redlich 1992). Most available data derive from case series by practitioners who treat MCS patients. These shortcomings notwithstanding, some general observations can be made. Although patients of virtually all ages have been described, MCS occurs most commonly among mid-life subjects. Workers in jobs of higher socio-economic status seem disproportionately affected, while the economically disadvantaged and non-White population seems underrepresented; this may be an artefact of differential access or of clinician bias. Women are more frequently affected than men. Epidemiological evidence strongly implicates some host idiosyncrasy as a risk factor, since mass outbreaks have been uncommon and only a small fraction of victims of chemical accidents or overexposures appear to develop MCS as a sequela (Welch and Sokas 1992; Simon 1992). Perhaps surprising in this regard is the fact that common atopic allergic disorders do not appear to be a strong risk factor for MCS among most groups.
Several groups of chemicals have been implicated in the majority of initiating episodes, specifically organic solvents, pesticides and respiratory irritants. This may be a function of the widespread usage of these materials in the workplace. The other commonplace setting in which many cases occur is in the sick building syndrome, some patients evolving from typical SBS-type complaints into MCS. Although the two illnesses have much in common, their epidemiological features should distinguish them. Sick building syndrome typically affects most individuals sharing a common environment, who improve in response to environmental remediation; MCS occurs sporadically and does not respond predictably to modifications of the office environment.
Finally, there is great interest in whether MCS is a new disorder or a new presentation or perception of an old one. Views are divided according to the proposed pathogenesis of MCS. Those favouring a biological role for environmental agents, including the clinical ecologists, postulate that MCS is a twentieth century disease with rising incidence related to increased chemical usage (Ashford and Miller 1991). Those who support the role of psychological mechanisms see MCS as an old somatoform illness with a new societal metaphor (Brodsky 1983; Shorter 1992). According to this view, the social perception of chemicals as agents of harm has resulted in the evolution of new symbolic content to the historic problem of psychosomatic disease.
Natural History
MCS has not yet been studied sufficiently to define its course or outcome. Reports of large numbers of patients have provided some clues. First, the general pattern of illness appears to be one of early progression as the process of generalization develops, followed by less predictable periods of incremental improvements and exacerbations. While these cycles may be perceived by the patient to be due to environmental factors or treatment, no scientific evidence for such relationships has been established.
Two important inferences follow. First, there is little evidence to suggest that MCS is progressive. Patients do not deteriorate from year to year in any measurable physical way, nor have complications such as infections or organ system failure resulted in the absence of intercurrent illness. There is no evidence that MCS is potentially lethal, despite the perceptions of the patients. While this may be the basis of a hopeful prognosis and reassurance, it has been equally clear from clinical descriptions that complete remissions are rare. While significant improvement occurs, this is generally based on enhanced patient function and sense of well-being. The underlying tendency to react to chemical exposures tends to persist, although symptoms may become sufficiently bearable to allow the victim to return to a normal lifestyle.
Clinical Management
Very little is known about the treatment of MCS. Many traditional and non-traditional methods have been tried, though none has been subjected to the usual scientific standards to confirm their efficacy. As with other conditions, approaches to treatment have paralleled theories of pathogenesis. Clinical ecologists and others, who believe that MCS is caused by immune dysfunction due to high burdens of exogenous chemicals, have focused attention on avoidance of artificial chemicals. This view has been accompanied by use of diagnostic strategies to determine “specific” sensitivities by various invalidated tests to “desensitize” patients. Coupled with this have been strategies to enhance underlying immunity with dietary supplements, such as vitamins and antioxidants, and efforts to eradicate yeasts or other commensal organisms. A most radical approach involves efforts to eliminate toxins from the body by chelation or accelerated turnover of fat where lipid-soluble pesticides, solvents and other organic chemicals are stored.
Those inclined to a psychological view of MCS have tried appropriately alternative approaches. Supportive individual or group therapies and more classic behavioural modification techniques have been described, though the efficacy of these approaches remains conjectural. Most observers have been struck by the intolerance of the patients to pharmacological agents typically employed for affective and anxiety disorders, an impression supported by a small placebo-controlled double-blind trial with fluvoxamine that was conducted by the author and aborted due to side effects in five of the first eight enrolees.
The limitations of present knowledge notwithstanding, certain treatment principles can be enunciated.
First, to the extent possible, the search for a specific “cause” of MCS in the individual case should be minimized—it is fruitless and counterproductive. Many patients have had considerable medical evaluation by the time MCS is considered and equate testing with evidence of pathology and the potential for a specific cure. Whatever the theoretical beliefs of the clinician, it is vital that the existing knowledge and uncertainty about MCS be explained to the patient, including specifically that its cause is unknown. The patient should be reassured that consideration of psychological issues does not make the illness less real, less serious or less worthy of treatment. Patients can also be reassured that MCS is not likely to be progressive or fatal, and they should be made to understand that total cures are not likely with present modalities.
Uncertainty about pathogenesis aside, it is most often necessary to remove the patient from components of their work environment which trigger symptoms. Although radical avoidance is of course counterproductive to the goal of enhancing the worker’s functioning, regular and severe symptomatic reactions should be controlled as far as possible as the basis for a strong therapeutic relationship with the patient. Often this requires a job change. Workers’ compensation may be available; even in the absence of detailed understanding of disease pathogenesis, MCS may correctly be characterized as a complication of a work exposure which is more readily identified (Cullen 1994).
The goal of all subsequent therapy is improvement of function. Psychological problems, such as adjustment difficulties, anxiety and depression should be treated, as should coexistent problems like typical atopic allergies. Since MCS patients do not tolerate chemicals in general, non-pharmacological approaches may be necessary. Most patients need direction, counselling and reassurance to adjust to an illness without an established treatment (Lewis 1987). To the extent possible, patients should be encouraged to expand their activities and should be discouraged from passivity and dependence, which are common responses to the disorder.
Prevention and Control
Obviously, primary prevention strategies cannot be developed given present knowledge of the pathogenesis of the disorder or of its predisposing host risk factors. On the other hand, reduction of opportunities in the workplace for the uncontrolled acute exposures which precipitate MCS in some hosts, such as those involving respiratory irritants, solvents and pesticides, will likely reduce the occurrence of MCS. Proactive measures to improve the air quality of poorly ventilated offices would also probably help.
Secondary prevention would appear to offer a greater opportunity for control, although no specific interventions have been studied. Since psychological factors may play a role in victims of occupational overexposures, careful and early management of exposed persons is advisable even when the prognosis from the point of view of the exposure itself is good. Patients seen in clinics or emergency rooms immediately after acute exposures should be assessed for their reactions to the events and should probably receive very close follow-up where undue concerns of long-term effects or persistent symptoms are noted. Obviously, efforts should be made for such patients to ensure that preventable reoccurrences do not come about, since this kind of exposure may be an important risk factor for MCS regardless of the causal mechanism.
Sick Building Syndrome
Sick building syndrome (SBS) is a term used to describe office worker discomfort and medical symptoms that are related to building characteristics, to pollutant exposures and to work organization, and that are mediated through personal risk factors. A wide range of definitions exists, but disagreement remains (a) as to whether a single individual in a building can develop this syndrome or whether a set numeric criterion (the proportion affected) should be used; and (b) as to the necessary symptom components. Figure 1 lists symptoms commonly included in SBS; in recent years, with increased understanding, complaints related to odours have generally been dropped from the list and chest symptoms included under mucous membrane irritation. A critical distinction needs to be made between SBS and building-related illness (BRI), where verifiable irritation, allergy or illness such as hypersensitivity pneumonitis, asthma or carbon monoxide-induced headaches may be present as an outbreak associated with a building. SBS should also be distinguished from multiple chemical sensitivities (MCS; see below) which is more sporadic in occurrence, often occurs within an SBS population, and is much less responsive to modifications of the office environment.
Figure 1. Sick building syndrome.
SBS should be simultaneously viewed from and informed by three disparate perspectives. For health professionals, the view is from the perspective of medicine and the health sciences as they define symptoms related to indoor work and their associated pathophysiological mechanisms. The second perspective is that of engineering, including design, commissioning, operations, maintenance and exposure assessment for specific pollutants. The third perspective includes the organizational, social and psychological aspects of work.
Epidemiology
Since the mid-1970s, increasingly voiced office worker discomfort has been studied in formal ways. These have included field epidemiological studies using a building or a workstation as the sampling unit to identify risk factors and causes, population-based surveys to define prevalence, chamber studies of humans to define effects and mechanisms, and field intervention studies.
Cross-sectional and case-control studies
Approximately 30 cross-sectional surveys have been published (Mendell 1993; Sundell et al. 1994). Many of these have included primarily “non-problem” buildings, selected at random. These studies consistently demonstrate an association between mechanical ventilation and increased symptom reporting. Additional risk factors have been defined in several case-control studies. Figure 2 presents a grouping of widely recognized risk factors associated with increased rates of complaints.
Many of these factors overlap; they are not mutually exclusive. For example, the presence of inadequate housekeeping and maintenance, the presence of strong indoor pollution sources and increased individual susceptibility may lead to much greater problems than the presence of any one factor alone.
Figure 2. Risk factors for and causes of the sick building syndrome.
Factor and principal components analyses of questionnaire responses in cross-sectional surveys have explored the interrelationship of various symptoms. Consistently, symptoms related to single organ systems have clustered together more strongly than symptoms relating to different organ systems. That is, eye irritation, eye tearing, eye dryness, and eye itching all appear to correlate very strongly, and little benefit is obtained from looking at multiple symptoms within an organ system.
Controlled exposure studies
Animal testing to determine irritant properties and thresholds has become standard. A consensus method of the American Society for Testing and Materials (1984) is widely regarded as the basic instrument. This method has been used to develop structure-activity relationships, to demonstrate that more than one irritant receptor may exist in the trigeminal nerve and to explore interactions between multiple exposures. Most recently, it has been used to demonstrate the irritating properties of office equipment offgassing.
Analogous to this method, several approaches have been defined to document methods and dose-response relationships for irritation in humans. This work meanwhile suggests that, at least for “non-reactive” compounds such as saturated aliphatic hydrocarbons, the percentage of vapour pressure saturation of a compound is a reasonable predictor of its irritant potency. Some evidence also supports the view that increasing the number of compounds in complex mixtures decreases the irritant thresholds. That is, the more agents that are present, even at a constant mass, the greater the irritation.
Controlled exposure studies have been performed of volunteers in stainless steel chambers. Most have been performed with one constant mixture of volatile organic compounds (VOC) (Mølhave and Nielsen 1992). These consistently document relationships between symptoms and increasing exposure levels. Office workers who perceived themselves as “susceptible” to the effects of usual levels of VOCs indoors demonstrated some impairment on standard tests of neuropsychological performance (Mølhave, Bach and Pederson 1986). Healthy volunteers, on the other hand, demonstrated mucous membrane irritation and headaches at exposures in the range of 10 to 25 mg/m3, but no changes on neuropsychological performance. More recently, office workers demonstrated similar symptoms after simulated work in environments where pollutants from commonly used office equipment were generated. Animals reacted similarly when a standardized test of irritant potency was used.
Population-based studies
To date, three population-based studies have been published in Sweden, Germany and the United States. The questionnaires differed considerably, and thus prevalence estimates cannot be directly compared. Nevertheless, between 20 and 35% of respondents from various buildings not known to be sick were found to have complaints.
Mechanisms
A number of potential mechanisms and objective measures to explain and examine symptoms within specific organ systems have been identified. None of these has a high predictive value for the presence of disease, and they are therefore not suitable for clinical diagnostic use. They are useful in field research and epidemiological investigations. For many of these it is unclear whether they should be regarded as mechanisms, as markers of effect, or as measures of susceptibility.
Eyes
Both allergic and irritant mechanisms have been proposed as explanations for eye symptoms. Shorter tear-film break-up time, a measure of tear film instability, is associated with increased levels of symptoms. “Fat-foam thickness” measurement and photography for documentation of ocular erythema have also been used. Some authors attribute eye symptoms at least in part to increased individual susceptibility as measured by those factors. In addition, office workers with ocular symptoms have been demonstrated to blink less frequently when working at video display terminals.
Nose
Both allergic and irritant mechanisms have been proposed as explanations for nasal symptoms. Measures that have successfully been used include nasal swabs (eosinophils), nasal lavage or biopsy, acoustic rhinometry (nasal volume), anterior and posterior rhinomanometry (plethysmography) and measures of nasal hyperreactivity.
Central nervous system
Neuropsychological tests have been used to document decreased performance on standardized tests, both as a function of controlled exposure (Mølhave, Bach and Pederson 1986) and as a function of the presence of symptoms (Middaugh, Pinney and Linz 1982).
Individual risk factors
Two sets of individual risk factors have been discussed. First, two commonly recognized diatheses, atopy and seborrhea, are considered predisposing factors for medically defined symptoms. Second, psychological variables may be important. For example, personal traits such as anxiety, depression or hostility are associated with sick-role susceptibility. Similarly, work stress is so consistently associated with building-related symptoms that some causal association is likely to be present. Which of the three components of work stress—individual traits, coping skills, and organization function such as poor management styles—is the dominant cause remains undetermined. It is recognized that failing to intervene in a well-defined problem leads workers to experience their discomfort with increasing distress.
Engineering and Sources
Beginning in the late 1970s, the US National Institute for Occupational Safety and Health (NIOSH) responded to requests for help in identifying causes of occupant discomfort in buildings, attributing problems to ventilation systems (50%), microbiological contamination (3 to 5%), strong indoor pollution sources (tobacco 3%, others 14%), pollutants entrained from the outside (15%) and others. On the other hand, Woods (1989) and Robertson (et al. 1988) published two well-known series of engineering analyses of problem buildings, documenting on average the presence of three potential causal factors in each building.
One current professional ventilation standard (American Society of Heating, Refrigerating, and Airconditioning Engineers (1989) suggests two approaches to ventilation: a ventilation rate procedure and an air quality procedure. The former provides a tabular approach to ventilation requirements: office buildings require 20 cubic feet of outside air per occupant per minute to maintain occupant complaint rates of environmental discomfort at below 20%. This assumes relatively weak pollution sources. When stronger sources are present, that same rate will provide less satisfaction. For example, when smoking is permitted at usual rates (according to data from the early 1980s), approximately 30% of occupants will complain of environmental discomfort. The second approach requires the selection of a target concentration in air (particulates, VOCs, formaldehyde, etc.), information on emission rates (pollutant per time per mass or surface), and derives the ventilation requirements. Although this is an intellectually much more satisfying procedure, it remains elusive because of inadequate emissions data and disagreement on target concentrations.
Pollutants
Environmental scientists have generally defined exposure and health effects on a pollutant-by-pollutant basis. The American Thoracic Society (1988) defined six important categories, listed in figure 3.
Figure 3. Principal pollutant categories.
Environmental criteria have been established for many of the individual substances in these six groups. The utility and applicability of such criteria for indoor environments is controversial for many reasons. For example, the goals of threshold limit values often do not include prevention of eye irritation, a common complaint in indoor environments with requirements for close eye work at video display units. For most of the pollutant categories, the problem of interactions, commonly termed the “multiple contaminants problem,” remains inadequately defined. Even for agents that are thought to affect the same receptor, such as aldehydes, alcohols and ketones, no prediction models are well established. Finally, the definition of “representative compounds” for measurement is unclear. That is, pollutants must be measurable, but complex mixtures vary in their composition. It is unclear, for instance, whether the chronic residual odor annoyance due to environmental tobacco smoke correlates better with nicotine, particulates, carbon monoxide or other pollutants. The measure “total volatile organic compounds” is meanwhile considered an interesting concept, but is not useful for practical purposes as the various components have such radically different effects (Mølhave and Nielsen 1992; Brown et al. 1994). Particulates indoors may differ in composition from their outdoor counterparts, as filter sizes affect entrained concentrations, and indoor sources may differ from outdoor sources. There are measurement problems as well, since the sizes of filters used will affect which particles are collected. Different filters may be needed for indoor measurements.
Finally, emerging data suggest that reactive indoor pollutants may interact with other pollutants and lead to new compounds. For example, the presence of ozone, either from office machines or entrained from outdoors, may interact with 4-phenylcyclohexene and generate aldehydes (Wechsler 1992).
Primary Aetiological Theories
Organic solvents
Buildings have always relied on general dilution strategies for pollutant removal, but designers have assumed that humans were the primary source of pollutants. More recently, emissions from “solid materials” (such as particle board desks, carpeting and other furniture), from wet products (such as glues, wall paints, office machine toners) and personal products (perfumes) have been recognized as contributors to a complex mixture of very low levels of individual pollutants (summarized in Hodgson, Levin and Wolkoff 1994).
Several studies suggest that the presence of reactive volatile organic compounds, such as aldehydes and halogenated hydrocarbons, are associated with increasing levels of symptoms. Offices with higher complaint rates have had greater “loss” of VOCs between incoming and outgoing air than did offices with lower complaints. In a prospective study of schools, short chain VOCs were associated with symptom development. In another survey, higher personal samples for VOCs using a screening sampler that “over-reacts” to reactive VOCs, such as aldehydes and halogenated hydrocarbons, were associated with higher symptom levels. In that study, women had higher levels of VOCs in their breathing zone, suggesting another potential explanation for the increased rate of complaints among women. VOCs might adsorb onto sinks, such as fleecy surfaces, and be re-emitted from such secondary sources. The interaction of ozone and relatively non-irritant VOCs to form aldehydes is also consistent with this hypothesis.
The presence of multiple potential sources, the consistency of VOC health effects and SBS symptoms, and the widely recognized problems associated with ventilation systems make VOCs an attractive aetiological agent. Solutions other than better design and operation of ventilation systems include the selection of low-emitting pollutants, better housekeeping and prevention of “indoor chemistry.”
Bioaerosols
Several studies have suggested that bioaerosols have the potential to contribute to occupant discomfort. They may do this through several different mechanisms: irritant emissions; release of fragments, spores or viable organisms leading to allergy; and secretion of complex toxins. Fewer data exist to support this theory than the others. Nevertheless, it is clear that heating, ventilating and air-conditioning systems may be sources of micro-organisms.
They have also been described in building construction materials (as a result of improper curing), as a result of unwanted water incursion and in office dust. The presence of sensitizers in the office environment, such as dust mites or cat dander brought in from home on clothing, presents another possibility of exposure. To the extent that biological agents contribute to the problem, dirt and water management become primary control strategies.
In addition, toxigenic fungi may be found on other porous products in buildings, including ceiling tile, spray-on insulation and wooden joists. Especially in residential environments, fungal proliferation associated with inadequate moisture control has been associated with symptoms.
Psychosocial aspects of work
In all studies where it has been examined, “work stress” was clearly associated with SBS symptoms. Workers’ perceptions of job pressures, task conflicts, and non-work stressors such as spousal or parental demands may clearly lead to the subjective experience of “stronger” irritation as a function of illness behaviour. At times, such perceptions may in fact result from poor supervisory practices. In addition, the presence of irritants leading to subjective irritation is thought to lead to “work stress”.
Evaluation of the Patient
The examination should be directed at identification or exclusion of a significant component of building related illness (BRI). Allergic disease should be identified and optimally managed. However, this must be done with awareness that non-allergic mechanisms may contribute to a substantial residual symptom burden. Sometimes individuals can be reassured of the absence of clear disease by studies such as portable peak flow monitoring or pre- and post-work pulmonary function tests. Once such observable or pathologically verifiable disease has been ruled out, evaluation of the building itself becomes paramount and should be done with industrial hygiene or engineering input. Documentation, management and remediation of identified problems is discussed in Controlling the Indoor Environment.
Conclusion
SBS is a phenomenon that can be experienced by an individual, but is usually seen in groups; it is associated with engineering deficiencies and is likely caused by a series of pollutants and pollutant categories. As with all “dis-ease,” a component of personal psychology serves as an effect modifier that can lead to varying degrees of symptom intensity at any given level of distress.
Systemic Conditions: An Introduction
The last edition of this Encyclopaedia did not contain articles on either sick building syndrome (SBS) or multiple chemical sensitivities (MCS) (the latter term was coined by Cullen, 1987). Most practitioners of occupational medicine are not comfortable with such symptomatically driven and frequently psychologically related phenomena, at least partly for the reason that patients with these syndromes do not respond reliably to the standard means of occupational health intervention, namely, exposure reduction. Non-occupational physicians in general medical practice also react similarly: patients with little verifiable pathology, such as those complaining of chronic fatigue syndrome or fibromyalgia, are regarded as more difficult to treat (and generally regard themselves as more disabled) than patients with deforming conditions such as rheumatoid arthritis. There is clearly less regulatory imperative for sick building syndrome and multiple chemical sensitivities than for the classic occupational syndromes such as lead intoxication or silicosis. This discomfort on the part of treating physicians and the lack of appropriate regulatory guidance is unfortunate, however understandable it may be, because it leads to minimization of the importance of these increasingly common, albeit largely subjective and non-lethal complaints. Since many workers with these conditions claim total disability, and few examples of cures can be found, multiple chemical sensitivities and sick building syndrome present important challenges to compensation systems.
In the developed world, since many classic occupational toxins are better controlled, symptomatic syndromes, such as those under present scrutiny that are associated with lower-level exposures, are assuming increasing recognition as significant economic and health concerns. Managers are frustrated by these conditions for a number of reasons. As there are no clear-cut regulatory requirements in most jurisdictions which cover indoor air or hypersusceptible individuals (with the important exception being persons with recognized allergic disorders), it is impossible for management to be certain whether or not they are in compliance. Agent-specific contaminant levels developed for industrial settings, such as the US Occupational Safety and Health Administration’s (OSHA’s) permissible exposure levels (PELs) or the American Conference of Governmental Industrial Hygienists’ (ACGIH’s) threshold limit values (TLVs), are clearly not able to prevent or predict symptomatic complaints in office and school workers. Finally, because of the apparent importance of individual susceptibility and psychological factors as determinants of response to low levels of contaminants, the impact of environmental interventions is not as predictable as many would like before a decision is taken to commit scarce building or maintenance resources. Often after complaints arise, a potential culprit such as elevated volatile organic compound levels with respect to outdoor air is found, and yet following remediation, complaints persist or reoccur.
Employees who suffer from symptoms of either sick building syndrome or multiple chemical sensitivities are often less productive and frequently accusatory when management or government is reluctant to commit themselves to interventions which cannot be reliably predicted to ameliorate symptoms. Clearly, occupational health providers are among the few key individuals who may be able to facilitate reasonable middle ground outcomes to the advantage of all concerned. This is true whether or not an underlying cause is low levels of contaminants, or even in the rare case of true mass hysteria, which may often have low-level environmental triggers. Using skill and sensitivity to address, evaluate and incorporate a combination of factors into solutions is an important approach to management.
Sick building syndrome is the more contained and definable of the two conditions, and has even had definitions established by the World Health Organization (1987). Although there is debate, both in general and in specific instances, about whether a given lesion is more attributable to individual workers or to the building, it is widely acknowledged, based on controlled exposure studies with volatile organic compounds, as well as survey epidemiology, that modifiable environmental factors do drive the kinds of symptom which are subsumed under the following article entitled Sick Building Syndrome. In that article, Michael Hodgson (1992) details the triad of personal, work activity and building factors which may contribute in various proportions to symptoms among a population of workers. A major problem is in maintaining good employee-employer communication while investigation and attempts at remediation take place. Health professionals will usually require expert environmental consultation to assist in the evaluation and remediation of identified outbreaks.
Multiple chemical sensitivities is a more problematic condition to define than sick building syndrome. Some organized medical entities, including the American Medical Association, have published position papers which question the scientific basis of the diagnosis of this condition. Many physicians who practise without a rigorous scientific basis have nevertheless championed the validity of this diagnosis. They rely on unproven or over-interpreted diagnostic tests such as lymphocyte activation or brain imaging and may recommend treatments such as sauna therapies and megadoses of vitamins, practices which have in large part engendered the animosity of groups such as the American Medical Association. However, no one denies that there is a group of patients who present with complaints of becoming symptomatic in response to low levels of ambient chemicals. Their constitutional symptoms overlap those of other subjective syndromes such as chronic fatigue syndrome and fibromyalgia. These symptoms include pain, fatigue and confusion, they worsen with low-level chemical exposure and they are reported to be present in a substantial percentage of patients who have been diagnosed with these other syndromes. Of great import, but still unresolved, is the question whether chemical sensitivity symptoms are acquired (and to what extent) because of a preceding chemical overexposure, or whether—as in the commonly reported situation—they arise without a major identified precipitating event.
Multiple chemical sensitivities is sometimes invoked as an outcome in certain sick building syndrome outbreaks which are not resolved or ameliorated after routine investigation and remediation. Here it is clear that MCS afflicts an individual or small number of people, rarely a population; it is the effect on a population that may even be a criterion for the sick building syndrome by some definitions. MCS seems to be endemic in populations, whereas sick building syndrome is often epidemic; however, preliminary investigations suggest that some degree of chemical sensitivity (and chronic fatigue) may occur in outbreaks, as was found among American veterans of the Persian Gulf conflict. The controlled exposure studies which have done much to clarify the role of volatile organic compounds and irritants in sick building syndrome have yet to be performed in a controlled manner for multiple chemical sensitivities.
Many practitioners claim to recognize MCS when they see it, but there is no agreed-upon definition. It may well be included as a condition which “overlaps” other non-occupational syndromes such as chronic fatigue syndrome, fibromyalgia, somatization disorder and others. Sorting out its relationship to both psychiatric diagnoses and to early reports suggests that when the onset of the syndrome is fairly definable, there is a much lower rate of diagnosable psychiatric co-morbidity (Fiedler et al. 1996). The phenomenon of odor-triggered symptoms is distinctive, but clearly not unique, and the extent to which this is an occupational condition at all is debated. This is important because Dr. Cullen’s (1987) definition, like many others, describes multiple chemical sensitivities as a sequel to a better-characterized occupational or environmental disorder. However, as stated above, symptoms following exposure to ambient levels of odorants are common among individuals both with and without clinical diagnoses, and it may be just as important to explore the similarities between MCS and other conditions as to define the differences (Kipen et al. 1995; Buchwald and Garrity 1994).
Fatigue and Recovery
Fatigue and recovery are periodic processes in every living organism. Fatigue can be described as a state which is characterized by a feeling of tiredness combined with a reduction or undesired variation in the performance of the activity (Rohmert 1973).
Not all the functions of the human organism become tired as a result of use. Even when asleep, for example, we breathe and our heart is pumping without pause. Obviously, the basic functions of breathing and heart activity are possible throughout life without fatigue and without pauses for recovery.
On the other hand, we find after fairly prolonged heavy work that there is a reduction in capacity—which we call fatigue. This does not apply to muscular activity alone. The sensory organs or the nerve centres also become tired. It is, however, the aim of every cell to balance out the capacity lost by its activity, a process which we call recovery.
Stress, Strain, Fatigue and Recovery
The concepts of fatigue and recovery at human work is closely related to the ergonomic concepts of stress and strain (Rohmert 1984) (figure 1).
Figure 1. Stress, strain and fatigue
Stress means the sum of all parameters of work in the working system influencing people at work, which are perceived or sensed mainly over the receptor system or which put demands on the effector system. The parameters of stress result from the work task (muscular work, non-muscular work—task-oriented dimensions and factors) and from the physical, chemical and social conditions under which the work has to be done (noise, climate, illumination, vibration, shift work, etc.—situation-oriented dimensions and factors).
The intensity/difficulty, the duration and the composition (i.e., the simultaneous and successive distribution of these specific demands) of the stress factors results in combined stress, which all the exogenous effects of a working system exert on the working person. This combined stress can be actively coped with or passively put up with, specifically depending on the behaviour of the working person. The active case will involve activities directed towards the efficiency of the working system, while the passive case will induce reactions (voluntary or involuntary), which are mainly concerned with minimizing stress. The relation between the stress and activity is decisively influenced by the individual characteristics and needs of the working person. The main factors of influence are those that determine performance and are related to motivation and concentration and those related to disposition, which can be referred to as abilities and skills.
The stresses relevant to behaviour, which are manifest in certain activities, cause individually different strains. The strains can be indicated by the reaction of physiological or biochemical indicators (e.g., raising the heart rate) or it can be perceived. Thus, the strains are susceptible to “psycho-physical scaling”, which estimates the strain as experienced by the working person. In a behavioural approach, the existence of strain can also be derived from an activity analysis. The intensity with which indicators of strain (physiological-biochemical, behaviouristic or psycho-physical) react depends on the intensity, duration, and combination of stress factors as well as on the individual characteristics, abilities, skills, and needs of the working person.
Despite constant stresses the indicators derived from the fields of activity, performance and strain may vary over time (temporal effect). Such temporal variations are to be interpreted as processes of adaptation by the organic systems. The positive effects cause a reduction of strain/improvement of activity or performance (e.g., through training). In the negative case, however, they will result in increased strain/reduced activity or performance (e.g., fatigue, monotony).
The positive effects may come into action if the available abilities and skills are improved in the working process itself, e.g., when the threshold of training stimulation is slightly exceeded. The negative effects are likely to appear if so-called endurance limits (Rohmert 1984) are exceeded in the course of the working process. This fatigue leads to a reduction of physiological and psychological functions, which can be compensated by recovery.
To restore the original performance rest allowances or at least periods with less stress are necessary (Luczak 1993).
When the process of adaptation is carried beyond defined thresholds, the employed organic system may be damaged so as to cause a partial or total deficiency of its functions. An irreversible reduction of functions may appear when stress is far too high (acute damage) or when recovery is impossible for a longer time (chronic damage). A typical example of such damage is noise-induced hearing loss.
Models of Fatigue
Fatigue can be many-sided, depending on the form and combi-nation of strain, and a general definition of it is yet not possible. The biological proceedings of fatigue are in general not measurable in a direct way, so that the definitions are mainly oriented towards the fatigue symptoms. These fatigue symptoms can be divided, for example, into the following three categories.
- Physiological symptoms: fatigue is interpreted as a decrease of functions of organs or of the whole organism. It results in physiological reactions, e.g., in an increase of heart rate frequency or electrical muscle activity (Laurig 1970).
- Behavioural symptoms: fatigue is interpreted mainly as a decrease of performance parameters. Examples are increasing errors when solving certain tasks, or an increasing variability of performance.
- Psycho-physical symptoms: fatigue is interpreted as an increase of the feeling of exertion and deterioration of sensation, depending on the intensity, duration and composition of stress factors.
In the process of fatigue all three of these symptoms may play a role, but they may appear at different points in time.
Physiological reactions in organic systems, particularly those involved in the work, may appear first. Later on, the feelings of exertion may be affected. Changes in performance are manifested generally in a decreasing regularity of work or in an increasing quantity of errors, although the mean of the performance may not yet be affected. On the contrary, with appropriate motivation, the working person may even try to maintain performance through will-power. The next step may be a clear reduction of performance ending with a breakdown of performance. The physiological symptoms may lead to a breakdown of the organism including changes of the structure of personality and in exhaustion. The process of fatigue is explained in the theory of successive destabilization (Luczak 1983).
The principal trend of fatigue and recovery is shown in figure 2.
Figure 2. Principal trend of fatigue and recovery
Prognosis of Fatigue and Recovery
In the field of ergonomics there is a special interest in predicting fatigue dependent on the intensity, duration and composition of stress factors and to determine the necessary recovery time. Table 1 shows those different activity levels and consideration periods and possible reasons of fatigue and different possibilities of recovery.
Table 1. Fatigue and recovery dependent on activity levels
|
Level of activity |
Period |
Fatigue from |
Recovery by |
|
Work life |
Decades |
Overexertion for |
Retirement |
|
Phases of work life |
Years |
Overexertion for |
Holidays |
|
Sequences of |
Months/weeks |
Unfavourable shift |
Weekend, free |
|
One work shift |
One day |
Stress above |
Free time, rest |
|
Tasks |
Hours |
Stress above |
Rest period |
|
Part of a task |
Minutes |
Stress above |
Change of stress |
In ergonomic analysis of stress and fatigue for determining the necessary recovery time, considering the period of one working day is the most important. The methods of such analyses start with the determination of the different stress factors as a function of time (Laurig 1992) (figure 3).
Figure 3. Stress as a function of time
The stress factors are determined from the specific work content and from the conditions of work. Work content could be the production of force (e.g., when handling loads), the coordination of motor and sensory functions (e.g., when assembling or crane operating), the conversion of information into reaction (e.g., when controlling), the transformations from input to output information (e.g., when programming, translating) and the production of information (e.g., when designing, problem solving). The conditions of work include physical (e.g., noise, vibration, heat), chemical (chemical agents) and social (e.g., colleagues, shift work) aspects.
In the easiest case there will be a single important stress factor while the others can be neglected. In those cases, especially when the stress factors results from muscular work, it is often possible to calculate the necessary rest allowances, because the basic concepts are known.
For example, the sufficient rest allowance in static muscle work depends on the force and duration of muscular contraction as in an exponential function linked by multiplication according to the formula:
![]()
with
R.A. = Rest allowance in percentage of t
t = duration of contraction (working period) in minutes
T = maximal possible duration of contraction in minutes
f = the force needed for the static force and
F = maximal force.
The connection between force, holding time and rest allowances is shown in figure 4.
Figure 4. Percentage rest allowances for various combinations of holding forces and time
Similar laws exist for heavy dynamic muscular work (Rohmert 1962), active light muscular work (Laurig 1974) or different industrial muscular work (Schmidtke 1971). More rarely you find comparable laws for non-physical work, e.g., for computing (Schmidtke 1965). An overview of existing methods for determining rest allowances for mainly isolated muscle and non-muscle work is given by Laurig (1981) and Luczak (1982).
More difficult is the situation where a combination of different stress factors exists, as shown in figure 5, which affect the working person simultaneously (Laurig 1992).
Figure 5. The combination of two stress factors
The combination of two stress factors, for example, can lead to different strain reactions depending on the laws of combination. The combined effect of different stress factors can be indifferent, compensatory or cumulative.
In the case of indifferent combination laws, the different stress factors have an effect on different subsystems of the organism. Each of these subsystems can compensate for the strain without the strain being fed into a common subsystem. The overall strain depends on the highest stress factor, and thus laws of superposition are not needed.
A compensatory effect is given when the combination of different stress factors leads to a lower strain than does each stress factor alone. The combination of muscular work and low temperatures can reduce the overall strain, because low temperatures allow the body to lose heat which is produced by the muscular work.
A cumulative effect arises if several stress factors are superimposed, that is, they must pass through one physiological “bottleneck”. An example is the combination of muscular work and heat stress. Both stress factors affect the circulatory system as a common bottleneck with resultant cumulative strain.
Possible combination effects between muscle work and physical conditions are described in Bruder (1993) (see table 2).
Table 2. Rules of combination effects of two stress factors on strain
|
Cold |
Vibration |
Illumination |
Noise |
|
|
Heavy dynamic work |
– |
+ |
0 |
0 |
|
Active light muscle work |
+ |
+ |
0 |
0 |
|
Static muscle work |
+ |
+ |
0 |
0 |
0 indifferent effect; + cumulative effect; – compensatory effect.
Source: Adapted from Bruder 1993.
For the case of the combination of more than two stress factors, which is the normal situation in practice, only limited scientific knowledge is available. The same applies for the successive combination of stress factors, (i.e., the strain effect of different stress factors which affect the worker successively). For such cases, in practice, the necessary recovery time is determined by measuring physiological or psychological parameters and using them as integrating values.
General Fatigue
This article is adapted from the 3rd edition of the Encyclopaedia of Occupational Health and Safety.
The two concepts of fatigue and rest are familiar to all from personal experience. The word “fatigue” is used to denote very different conditions, all of which cause a reduction in work capacity and resistance. The very varied use of the concept of fatigue has resulted in an almost chaotic confusion and some clarification of current ideas is necessary. For a long time, physiology has distinguished between muscle fatigue and general fatigue. The former is an acute painful phenomenon localized in the muscles: general fatigue is characterized by a sense of diminishing willingness to work. This article is concerned only with general fatigue, which may also be called “psychic fatigue” or “nervous fatigue” and the rest that it necessitates.
General fatigue may be due to quite different causes, the most important of which are shown in figure 1. The effect is as if, during the course of the day, all the various stresses experienced accumulate within the organism, gradually producing a feeling of increasing fatigue. This feeling prompts the decision to stop work; its effect is that of a physiological prelude to sleep.
Figure 1. Diagrammatic presentation of the cumulative effect of the everyday causes of fatigue
Fatigue is a salutary sensation if one can lie down and rest. However, if one disregards this feeling and forces oneself to continue working, the feeling of fatigue increases until it becomes distressing and finally overwhelming. This daily experience demonstrates clearly the biological significance of fatigue which plays a part in sustaining life, similar to that played by other sensations such as, for example, thirst, hunger, fear, etc.
Rest is represented in figure 1 as the emptying of a barrel. The phenomenon of rest can take place normally if the organism remains undisturbed or if at least one essential part of the body is not subjected to stress. This explains the decisive part played on working days by all work breaks, from the short pause during work to the nightly sleep. The simile of the barrel illustrates how necessary it is for normal living to reach a certain equilibrium between the total load borne by the organism and the sum of the possibilities for rest.
Neurophysiological interpretation of fatigue
The progress of neurophysiology during the last few decades has greatly contributed to a better understanding of the phenomena triggered off by fatigue in the central nervous system.
The physiologist Hess was the first to observe that electrical stimulation of certain of the diencephalic structures, and more especially of certain of the structures of the medial nucleus of the thalamus, gradually produced an inhibiting effect which showed itself in a deterioration in the capacity for reaction and in a tendency to sleep. If the stimulation was continued for a certain time, general relaxation was followed by sleepiness and finally by sleep. It was later proved that starting from these structures, an active inhibition may extend to the cerebral cortex where all conscious phenomena are centered. This is reflected not only in behaviour, but also in the electrical activity of the cerebral cortex. Other experiments have also succeeded in initiating inhibitions from other subcortical regions.
The conclusion which can be drawn from all these studies is that there are structures located in the diencephalon and mesencephalon which represent an effective inhibiting system and which trigger off fatigue with all its accompanying phenomena.
Inhibition and activation
Numerous experiments performed on animals and humans have shown that the general disposition of them both to reaction depends not only on this system of inhibition but essentially also on a system functioning in an antagonistic manner, known as the reticular ascending system of activation. We know from experiments that the reticular formation contains structures that control the degree of wakefulness, and consequently the general dispositions to a reaction. Nervous links exist between these structures and the cerebral cortex where the activating influences are exerted on the consciousness. Moreover, the activating system receives stimulation from the sensory organs. Other nervous connections transmit impulses from the cerebral cortex—the area of perception and thought—to the activation system. On the basis of these neurophysiological concepts, it can be established that external stimuli, as well as influences originating in the areas of consciousness, may, in passing through the activating system, stimulate a disposition to a reaction.
In addition, many other investigations make it possible to conclude that stimulation of the activating system frequently spreads also from the vegetative centers, and cause the organism to orient towards the expenditure of energy, towards work, struggle, flight, etc. (ergotropic conversion of the internal organs). Conversely, it appears that stimulation of the inhibiting system within the sphere of the vegetative nervous system causes the organism to tend towards rest, reconstitution of its reserves of energy, phenomena of assimilation (trophotropic conversion).
By synthesis of all these neurophysiological findings, the following conception of fatigue can be established: the state and feeling of fatigue are conditioned by the functional reaction of the consciousness in the cerebral cortex, which is, in turn, governed by two mutually antagonistic systems—the inhibiting system and the activating system. Thus, the disposition of humans to work depends at each moment on the degree of activation of the two systems: if the inhibiting system is dominant, the organism will be in a state of fatigue; when the activating system is dominant, it will exhibit an increased disposition to work.
This psychophysiological conception of fatigue makes it possible to understand certain of its symptoms which are sometimes difficult to explain. Thus, for example, a feeling of fatigue may disappear suddenly when some unexpected outside event occurs or when emotional tension develops. It is clear in both these cases that the activating system has been stimulated. Conversely, if the surroundings are monotonous or work seems boring, the functioning of the activating system is diminished and the inhibiting system becomes dominant. This explains why fatigue appears in a monotonous situation without the organism being subjected to any workload.
Figure 2 depicts diagrammatically the notion of the mutually antagonistic systems of inhibition and activation.
Figure 2. Diagrammatic presentation of the control of disposition to work by means of inhibiting and activating systems
Clinical fatigue
It is a matter of common experience that pronounced fatigue occurring day after day will gradually produce a state of chronic fatigue. The feeling of fatigue is then intensified and comes on not only in the evening after work but already during the day, sometimes even before the start of work. A feeling of malaise, frequently of an emotive nature, accompanies this state. The following symptoms are often observed in persons suffering from fatigue: heightened psychic emotivity (antisocial behaviour, incompatibility), tendency to depression (unmotivated anxiety), and lack of energy with loss of initiative. These psychic effects are often accompanied by an unspecific malaise and manifest themselves by psychosomatic symptoms: headaches, vertigo, cardiac and respiratory functional disturbances, loss of appetite, digestive disorders, insomnia, etc.
In view of the tendency towards morbid symptoms that accompany chronic fatigue, it may justly be called clinical fatigue. There is a tendency towards increased absenteeism, and particularly to more absences for short periods. This would appear to be caused both by the need for rest and by increased morbidity. The state of chronic fatigue occurs particularly among persons exposed to psychic conflicts or difficulties. It is sometimes very difficult to distinguish the external and internal causes. In fact, it is almost impossible to distinguish cause and effect in clinical fatigue: a negative attitude towards work, superiors or workplace may just as well be the cause of clinical fatigue as the result.
Research has shown that the switchboard operators and supervisory personnel employed in telecommunications services exhibited a significant increase in physiological symptoms of fatigue after their work (visual reaction time, flicker fusion frequency, dexterity tests). Medical investigations revealed that in these two groups of workers there was a significant increase in neurotic conditions, irritability, difficulty in sleeping and in the chronic feeling of lassitude, by comparison with a similar group of women employed in the technical branches of the postal, telephone and telegraphic services. The accumulation of symptoms was not always due to a negative attitude on the part of the women affected their job or their working conditions.
Preventive Measures
There is no panacea for fatigue but much can be done to alleviate the problem by attention to general working conditions and the physical environment at the workplace. For example much can be achieved by the correct arrangement of hours of work, provision of adequate rest periods and suitable canteens and restrooms; adequate paid holidays should also be given to workers. The ergonomic study of the workplace can also help in the reduction of fatigue by ensuring that seats, tables, and workbenches are of suitable dimensions and that the workflow is correctly organized. In addition, noise control, air-conditioning, heating, ventilation, and lighting may all have a beneficial effect on delaying the onset of fatigue in workers.
Monotony and tension may also be alleviated by controlled use of colour and decoration in the surroundings, intervals of music and sometimes breaks for physical exercises for sedentary workers. Training of workers and in particular of supervisory and management staff also play an important part.
More...
Biomechanics
Aims and Principles
Biomechanics is a discipline that approaches the study of the body as though it were solely a mechanical system: all parts of the body are likened to mechanical structures and are studied as such. The following analogies may, for example, be drawn:
- bones: levers, structural members
- flesh: volumes and masses
- joints: bearing surfaces and articulations
- joint linings: lubricants
- muscles: motors, springs
- nerves: feedback control mechanisms
- organs: power supplies
- tendons: ropes
- tissue: springs
- body cavities: balloons.
The main aim of biomechanics is to study the way the body produces force and generates movement. The discipline relies primarily on anatomy, mathematics and physics; related disciplines are anthropometry (the study of human body measurements), work physiology and kinesiology (the study of the principles of mechanics and anatomy in relation to human movement).
In considering the occupational health of the worker, biomechanics helps to understand why some tasks cause injury and ill health. Some relevant types of adverse health effect are muscle strain, joint problems, back problems and fatigue.
Back strains and sprains and more serious problems involving the intervertebral discs are common examples of workplace injuries that can be avoided. These often occur because of a sudden particular overload, but may also reflect the exertion of excessive forces by the body over many years: problems may occur suddenly or may take time to develop. An example of a problem that develops over time is “seamstress’s finger”. A recent description describes the hands of a woman who, after 28 years of work in a clothing factory, as well as sewing in her spare time, developed hardened thickened skin and an inability to flex her fingers (Poole 1993). (Specifically, she suffered from a flexion deformity of the right index finger, prominent Heberden’s nodes on the index finger and thumb of the right hand, and a prominent callosity on the right middle finger due to constant friction from the scissors.) X-ray films of her hands showed severe degenerative changes in the outermost joints of her right index and middle fingers, with loss of joint space, articular sclerosis (hardening of tissue), osteophytes (bony growths at the joint) and bone cysts.
Inspection at the workplace showed that these problems were due to repeated hyperextension (bending up) of the outermost finger joint. Mechanical overload and restriction in blood flow (visible as a whitening of the finger) would be maximal across these joints. These problems developed in response to repeated muscle exertion in a site other than the muscle.
Biomechanics helps to suggest ways of designing tasks to avoid these types of injuries or of improving poorly designed tasks. Remedies for these particular problems are to redesign the scissors and to alter the sewing tasks to remove the need for the actions performed.
Two important principles of biomechanics are:
- Muscles come in pairs. Muscles can only contract, so for any joint there must be one muscle (or muscle group) to move it one way and a corresponding muscle (or muscle group) to move it in the opposite direction. Figure 1 illustrates the point for the elbow joint.
- Muscles contract most efficiently when the muscle pair is in relaxed balance. The muscle acts most efficiently when it is in the midrange of the joint it flexes. This is so for two reasons: first, if the muscle tries to contract when it is shortened, it will pull against the elongated opposing muscle. Because the latter is stretched, it will apply an elastic counterforce that the contracting muscle must overcome. Figure 2 shows the way in which muscle force varies with muscle length.
Figure 1. Skeletal muscles occur in pairs in order to initiate or reverse a movement
Figure 2. Muscle tension varies with muscle length
Second, if the muscle tries to contract at other than the midrange of the movement of the joint, it will operate at a mechanical disadvantage. Figure 3 illustrates the change in mechanical advantage for the elbow in three different positions.
Figure 3. Optimal positions for joint movement
An important criterion for work design follows from these principles: Work should be arranged so that it occurs with the opposing muscles of each joint in relaxed balance. For most joints, this means that the joint should be at about its midrange of movement.
This rule also means that muscle tension will be at a minimum while a task is performed. One example of the infringement of the rule is the overuse syndrome (RSI, or repetitive strain injury) which affects the muscles of the top of the forearm in keyboard operators who habitually operate with the wrist flexed up. Often this habit is forced on the operator by the design of the keyboard and workstation.
Applications
The following are some examples illustrating the application of biomechanics.
The optimum diameter of tool handles
The diameter of a handle affects the force that the muscles of the hand can apply to a tool. Research has shown that the optimum handle diameter depends on the use to which the tool is put. For exerting thrust along the line of the handle, the best diameter is one that allows the fingers and thumb to assume a slightly overlapping grip. This is about 40 mm. To exert torque, a diameter of about 50-65 mm is optimal. (Unfortunately, for both purposes most handles are smaller than these values.)
The use of pliers
As a special case of a handle, the ability to exert force with pliers depends on the handle separation, as shown in figure 4.
Figure 4. Grip strength of pliers jaws exerted by male and female users as a function of handle separation
Seated posture
Electromyography is a technique that can be used to measure muscle tension. In a study of the tension in the erector spinae muscles (of the back) of seated subjects, it was found that leaning back (with the backrest inclined) reduced the tension in these muscles. The effect can be explained because the backrest takes more of the weight of the upper body.
X-ray studies of subjects in a variety of postures showed that the position of relaxed balance of the muscles that open and close the hip joint corresponds to a hip angle of about 135º. This is close to the position (128º) naturally adopted by this joint in weightless conditions (in space). In the seated posture, with an angle of 90º at the hip, the hamstring muscles that run over both the knee and hip joints tend to pull the sacrum (the part of the vertebral column that connects with the pelvis) into a vertical position. The effect is to remove the natural lordosis (curvature) of the lumbar spine; chairs should have appropriate backrests to correct for this effort.
Screwdriving
Why are screws inserted clockwise? The practice probably arose in unconscious recognition that the muscles that rotate the right arm clockwise (most people are right-handed) are larger (and therefore more powerful) that the muscles that rotate it anticlockwise.
Note that left-handed people will be at a disadvantage when inserting screws by hand. About 9% of the population are left-handed and will therefore require special tools in some situations: scissors and can openers are two such examples.
A study of people using screwdrivers in an assembly task revealed a more subtle relation between a particular movement and a particular health problem. It was found that the greater the elbow angle (the straighter the arm), the more people had inflammation at the elbow. The reason for this effect is that the muscle that rotates the forearm (the biceps) also pulls the head of the radius (lower arm bone) onto the capitulum (rounded head) of the humerus (upper arm bone). The increased force at the higher elbow angle caused greater frictional force at the elbow, with consequent heating of the joint, leading to the inflammation. At the higher angle, the muscle also had to pull with greater force to effect the screwing action, so a greater force was applied than would have been required with the elbow at about 90º. The solution was to move the task closer to the operators to reduce the elbow angle to about 90º.
The cases above demonstrate that a proper understanding of anatomy is required for the application of biomechanics in the workplace. Designers of tasks may need to consult experts in functional anatomy to anticipate the types of problems discussed. (The Pocket Ergonomist (Brown and Mitchell 1986) based on electromyographical research, suggests many ways of reducing physical discomfort at work.)
Manual Material Handling
The term manual handling includes lifting, lowering, pushing, pulling, carrying, moving, holding and restraining, and encompasses a large part of the activities of working life.
Biomechanics has obvious direct relevance to manual handling work, since muscles must move to carry out tasks. The question is: how much physical work can people be reasonably expected to do? The answer depends on the circumstances; there are really three questions that need to be asked. Each one has an answer that is based on scientifically researched criteria:
- How much can be handled without damage to the body (in the form, for example, of muscle strain, disc injury or joint problems)? This is called the biomechanical criterion.
- How much can be handled without overexerting the lungs (breathing hard to the point of panting)? This is called the physiological criterion.
- How much do people feel able to handle comfortably? This is called the psychophysical criterion.
There is a need for these three different criteria because there are three broadly different reactions that can occur to lifting tasks: if the work goes on all day, the concern will be how the person feels about the task—the psychophysical criterion; if the force to be applied is large, the concern would be that muscles and joints are not overloaded to the point of damage—the biomechanical criterion; and if the rate of work is too great, then it may well exceed the physiological criterion, or the aerobic capacity of the person.
Many factors determine the extent of the load placed on the body by a manual handling task. All of them suggest opportunities for control.
Posture and Movements
If the task requires a person to twist or reach forward with a load, the risk of injury is greater. The workstation can often be redesigned to prevent these actions. More back injuries occur when the lift begins at ground level compared to mid-thigh level, and this suggests simple control measures. (This applies to high lifting as well.)
The load.
The load itself may influence handling because of its weight and its location. Other factors, such as its shape, its stability, its size and its slipperiness may all affect the ease of a handling task.
Organization and environment.
The way work is organized, both physically and over time (temporally), also influences handling. It is better to spread the burden of unloading a truck in a delivery bay over several people for an hour rather than to ask one worker to spend all day on the task. The environment influences handling—poor light, cluttered or uneven floors and poor housekeeping may all cause a person to stumble.
Personal factors.
Personal handling skills, the age of the person and the clothing worn also can influence handling requirements. Education for training and lifting are required both to provide necessary information and to allow time for the development of the physical skills of handling. Younger people are more at risk; on the other hand, older people have less strength and less physiological capacity. Tight clothing can increase the muscle force required in a task as people strain against the tight cloth; classic examples are the nurse’s smock uniform and tight overalls when people do work above their heads.
Recommended Weight Limits
The points mentioned above indicate that it is impossible to state a weight that will be “safe” in all circumstances. (Weight limits have tended to vary from country to country in an arbitrary manner. Indian dockers, for example, were once “allowed” to lift 110 kg, while their counterparts in the former People’s Democratic Republic of Germany were “limited” to 32 kg.) Weight limits have also tended to be too great. The 55 kg suggested in many countries is now thought to be far too great on the basis of recent scientific evidence. The National Institute for Occupational Safety and Health (NIOSH) in the United States has adopted 23 kg as a load limit in 1991 (Waters et al. 1993).
Each lifting task needs to be assessed on its own merits. A useful approach to determining a weight limit for a lifting task is the equation developed by NIOSH:
RWL = LC x HM x VM x DM x AM x CM x FM
Where
RWL = recommended weight limit for the task in question
HM = the horizontal distance from the centre of gravity of the load to the midpoint between the ankles (minimum 15 cm, maximum 80 cm)
VM = the vertical distance between the centre of gravity of the load and the floor at the start of the lift (maximum 175 cm)
DM = the vertical travel of the lift (minimum 25 cm, maximum 200 cm)
AM = asymmetry factor–the angle the task deviates from straight out in front of the body
CM = coupling multiplier–the ability to get a good grip on the item to be lifted, which is found in a reference table
FM = frequency multipliers–the frequency of the lifting.
All variables of length in the equation are expressed in units of centimetres. It should be noted that 23 kg is the maximum weight that NIOSH recommends for lifting. This has been reduced from 40 kg after observation of many people doing many lifting tasks has revealed that the average distance from the body of the start of the lift is 25 cm, not the 15 cm assumed in an earlier version of the equation (NIOSH 1981).
Lifting index.
By comparing the weight to be lifted in the task and the RWL, a lifting index (LI) can be obtained according to the relationship:
LI=(weight to be handled)/RWL.
Therefore, particularly valuable use of the NIOSH equation is the placing of lifting tasks in order of severity, using the lifting index to set priorities for action. (The equation has a number of limitations, however, that need to be understood for its most effective application. See Waters et al. 1993).
Estimating Spinal Compression Imposed by the Task
Computer software is available to estimate the spinal compression produced by a manual handling task. The 2D and 3D Static Strength Prediction Programs from the University of Michigan (“Backsoft”) estimate spinal compression. The inputs required to the program are:
- the posture in which the handling activity is performed
- the force exerted
- the direction of the force exertion
- the number of hands exerting the force
- the percentile of the population under study.
The 2D and 3D programs differ in that the 3D software allows computations applying to postures in three dimensions. The program output gives spinal compression data and lists the percentage of the population selected that would be able to do the particular task without exceeding suggested limits for six joints: ankle, knee, hip, first lumbar disc-sacrum, shoulder, and elbow. This method also has a number of limitations that need to be fully understood in order to derive maximum value out of the program.
Postures at Work
A person’s posture at work—the mutual organization of the trunk, head and extremities—can be analysed and understood from several points of view. Postures aim at advancing the work; thus, they have a finality which influences their nature, their time relation and their cost (physiological or otherwise) to the person in question. There is a close interaction between the body’s physiological capacities and characteristics and the requirement of the work.
Musculoskeletal load is a necessary element in body functions and indispensable in well-being. From the standpoint of the design of the work, the question is to find the optimal balance between the necessary and the excessive.
Postures have interested researchers and practitioners for at least the following reasons:
- A posture is the source of musculoskeletal load. Except for relaxed standing, sitting and lying horizontally, muscles have to create forces to balance the posture and/or control movements. In classical heavy tasks, for example in the construction industry or in the manual handling of heavy materials, external forces, both dynamic and static, add to the internal forces in the body, sometimes creating high loads which may exceed the capacity of the tissues. (See figure 1) Even in relaxed postures, when muscle work approaches zero, tendons and joints may be loaded and show signs of fatigue. A job with low apparent loading—an example being that of a microscopist—may become tedious and strenuous when it is carried out over a long period of time.
- Posture is closely related to balance and stability. In fact, posture is controlled by several neural reflexes where input from tactile sensations and visual cues from the surroundings play an important role. Some postures, like reaching objects from a distance, are inherently unstable. Loss of balance is a common immediate cause of work accidents. Some work tasks are performed in an environment where stability cannot always be guaranteed, for example, in the construction industry.
- Posture is the basis of skilled movements and visual observation. Many tasks require fine, skilled hand movements and close observation of the object of the work. In such cases, posture becomes the platform of these actions. Attention is directed to the task, and the postural elements are enlisted to support the tasks: the posture becomes motionless, the mus-cular load increases and becomes more static. A French research group showed in their classical study that immobility and musculoskeletal load increased when the rate of work increased (Teiger, Laville and Duraffourg 1974).
- Posture is a source of information on the events taking place at work. Observing posture may be intentional or unconscious. Skilful supervisors and workers are known to use postural observations as indicators of the work process. Often, observing postural information is not conscious. For example, on an oil drilling derrick, postural cues have been used to communicate messages between team members during different phases of a task. This takes place under conditions where other means of communication are not possible.
Figure 1. Too high hand positions or forward bending are amont the most commom ways of creating “static” load
Safety, Health and Working Postures
From a safety and health point of view, all the aspects of posture described above may be important. However, postures as a source of musculoskeletal illnesses such as low back diseases have attracted the most attention. Musculoskeletal problems related to repetitive work are also connected to postures.
Low back pain (LBP) is a generic term for various low back diseases. It has many causes and posture is one possible causal element. Epidemiological studies have shown that physically heavy work is conducive to LBP and that postures are one element in this process. There are several possible mechanisms which explain why certain postures may cause LBP. Forward bending postures increase the load on the spine and ligaments, which are especially vulnerable to loads in a twisted posture. External loads, especially dynamic ones, such as those imposed by jerks and slipping, may increase the loads on the back by a large factor.
From a safety and health standpoint, it is important to identify bad postures and other postural elements as part of the safety and health analysis of work in general.
Recording and Measuring Working Postures
Postures can be recorded and measured objectively by the use of visual observation or more or less sophisticated measuring techniques. They can also be recorded by using self-rating schemes. Most methods consider posture as one of the elements in a larger context, for example, as part of the job content—as do the AET and Renault’s Les profils des postes (Landau and Rohmert 1981; RNUR 1976)—or as a starting point for biomechanical calculations that also take into account other components.
In spite of the advancements in measuring technology, visual observation remains, under field conditions, the only practicable means of systematically recording postures. However, the precision of such measurements remains low. In spite of this, postural observations can be a rich source of information on work in general.
The following short list of measuring methods and techniques presents selected examples:
- Self-reporting questionnaires and diaries. Self-reporting questionnaires and diaries are an economical means of collecting postural information. Self-reporting is based on the perception of the subject and usually deviates greatly from “objectively” observed postures, but may still convey important information about the tediousness of the work.
- Observation of postures. The observation of postures includes the purely visual recording of the postures and their components as well as methods in which an interview completes the information. Computer support is usually available for these methods. Many methods are available for visual observations. The method may simply contain a catalogue of actions, including postures of the trunk and limbs (e.g., Keyserling 1986; Van der Beek, Van Gaalen and Frings-Dresen 1992) .The OWAS method proposes a structured scheme for the analysis, rating and evaluation of trunk and limb postures designed for field conditions (Karhu, Kansi and Kuorinka 1977). The recording and analysis method may contain notation schemes, some of them quite detailed (as with the posture targeting method, by Corlett and Bishop 1976), and they may provide a notation for the position of many anatomical elements for each element of the task (Drury 1987).
- Computer-aided postural analyses. Computers have aided postural analyses in many ways. Portable computers and special programs allow easy recording and fast analysis of postures. Persson and Kilbom (1983) have developed the program VIRA for upper-limb study; Kerguelen (1986) has produced a complete recording and analysis package for work tasks; Kivi and Mattila (1991) have designed a computerized OWAS version for recording and analysis.
Video is usually an integral part of the recording and analysis process. The US National Institute for Occupational Safety and Health (NIOSH) has presented guidelines for using video methods in hazard analysis (NIOSH 1990).
Biomechanical and anthropometrical computer programs offer specialized tools for analysing some postural elements in the work activity and in the laboratory (e.g., Chaffin 1969).
Factors Affecting Working Postures
Working postures serve a goal, a finality outside themselves. That is why they are related to external working conditions. Postural analysis that does not take into account the work environment and the task itself is of limited interest to ergonomists.
The dimensional characteristics of the workplace largely define the postures (as in the case of a sitting task), even for dynamic tasks (for example, the handling of material in a confined space). The loads to be handled force the body into a certain posture, as does the weight and nature of the working tool. Some tasks require that body weight be used to support a tool or to apply force on the object of the work, as shown, for example in figure 2.
Figure 2. Ergonomic aspects of standing
Individual differences, age and sex influence postures. In fact, it has been found that a “typical” or “best” posture, for example in manual handling, is largely fiction. For each individual and each working situation, there are a number of alternative “best” postures from the standpoint of different criteria.
Job Aids and Supports for Working Postures
Belts, lumbar supports and orthotics have been recommended for tasks with a risk of low back pain or upper-limb musculoskeletal injuries. It has been assumed that these devices give support to muscles, for example, by controlling intra-abdominal pressure or hand movements. They are also expected to limit the range of movement of the elbow, wrist or fingers. There is no evidence that modifying postural elements with these devices would help to avoid musculoskeletal problems.
Postural supports in the workplace and on machinery, such as handles, supporting pads for kneeling, and seating aids, may be useful in alleviating postural loads and pain.
Safety and Health Regulations concerning Postural Elements
Postures or postural elements have not been subject to regulatory activities per se. However, several documents either contain statements which have a bearing on postures or include the issue of postures as an integral element of a regulation. A complete picture of the existing regulatory material is not available. The following references are presented as examples.
- The International Labour Organization published a Recommendation in 1967 on maximum loads to be handled. Although the Recommendation does not regulate postural elements as such, it has a significant bearing on postural strain. The Recommendation is now outdated but has served an important purpose in focusing attention on problems in manual material handling.
- The NIOSH lifting guidelines (NIOSH 1981), as such, are not regulations either, but they have attained that status. The guidelines derive weight limits for loads using the location of the load—a postural element—as a basis.
- In the International Organization for Standardization as well as in the European Community, ergonomics standards and directives exist which contain matter relating to postural elements (CEN 1990 and 1991).
Muscular Work
Muscular Work in Occupational Activities
In industrialized countries around 20% of workers are still employed in jobs requiring muscular effort (Rutenfranz et al. 1990). The number of conventional heavy physical jobs has decreased, but, on the other hand, many jobs have become more static, asymmetrical and stationary. In developing countries, muscular work of all forms is still very common.
Muscular work in occupational activities can be roughly divided into four groups: heavy dynamic muscle work, manual materials handling, static work and repetitive work. Heavy dynamic work tasks are found in forestry, agriculture and the construction industry, for example. Materials handling is common, for example, in nursing, transportation and warehousing, while static loads exist in office work, the electronics industry and in repair and maintenance tasks. Repetitive work tasks can be found in the food and wood-processing industries, for example.
It is important to note that manual materials handling and repetitive work are basically either dynamic or static muscular work, or a combination of these two.
Physiology of Muscular Work
Dynamic muscular work
In dynamic work, active skeletal muscles contract and relax rhythmically. The blood flow to the muscles is increased to match metabolic needs. The increased blood flow is achieved through increased pumping of the heart (cardiac output), decreased blood flow to inactive areas, such as kidneys and liver, and increased number of open blood vessels in the working musculature. Heart rate, blood pressure, and oxygen extraction in the muscles increase linearly in relation to working intensity. Also, pulmonary ventilation is heightened owing to deeper breathing and increased breathing frequency. The purpose of activating the whole cardio-respiratory system is to enhance oxygen delivery to the active muscles. The level of oxygen consumption measured during heavy dynamic muscle work indicates the intensity of the work. The maximum oxygen consumption (VO2max) indicates the person’s maximum capacity for aerobic work. Oxygen consumption values can be translated to energy expenditure (1 litre of oxygen consumption per minute corresponds to approximately 5 kcal/min or 21 kJ/min).
In the case of dynamic work, when the active muscle mass is smaller (as in the arms), maximum working capacity and peak oxygen consumption are smaller than in dynamic work with large muscles. At the same external work output, dynamic work with small muscles elicits higher cardio-respiratory responses (e.g., heart rate, blood pressure) than work with large muscles (figure 1).
Figure 1. Static versus dynamic work
Static muscle work
In static work, muscle contraction does not produce visible movement, as, for example, in a limb. Static work increases the pressure inside the muscle, which together with the mechanical compression occludes blood circulation partially or totally. The delivery of nutrients and oxygen to the muscle and the removal of metabolic end-products from the muscle are hampered. Thus, in static work, muscles become fatigued more easily than in dynamic work.
The most prominent circulatory feature of static work is a rise in blood pressure. Heart rate and cardiac output do not change much. Above a certain intensity of effort, blood pressure increases in direct relation to the intensity and the duration of the effort. Furthermore, at the same relative intensity of effort, static work with large muscle groups produces a greater blood pressure response than does work with smaller muscles. (See figure 2)
Figure 2. The expanded stress-strain model modified from Rohmert (1984)
In principle, the regulation of ventilation and circulation in static work is similar to that in dynamic work, but the metabolic signals from the muscles are stronger, and induce a different response pattern.
Consequences of Muscular Overload in Occupational Activities
The degree of physical strain a worker experiences in muscular work depends on the size of the working muscle mass, the type of muscular contractions (static, dynamic), the intensity of contractions, and individual characteristics.
When muscular workload does not exceed the worker’s physical capacities, the body will adapt to the load and recovery is quick when the work is stopped. If the muscular load is too high, fatigue will ensue, working capacity is reduced, and recovery slows down. Peak loads or prolonged overload may result in organ damage (in the form of occupational or work-related diseases). On the other hand, muscular work of certain intensity, frequency, and duration may also result in training effects, as, on the other hand, excessively low muscular demands may cause detraining effects. These relationships are represented by the so-called expanded stress-strain concept developed by Rohmert (1984) (figure 3).
Figure 3. Analysis of acceptable workloads
In general, there is little epidemiological evidence that muscular overload is a risk factor for diseases. However, poor health, disability and subjective overload at work converge in physically demanding jobs, especially with older workers. Furthermore, many risk factors for work-related musculoskeletal diseases are connected to different aspects of muscular workload, such as the exertion of strength, poor working postures, lifting and sudden peak loads.
One of the aims of ergonomics has been to determine acceptable limits for muscular workloads which could be applied for the prevention of fatigue and disorders. Whereas the prevention of chronic effects is the focus of epidemiology, work physiology deals mostly with short-term effects, that is, fatigue in work tasks or during a work day.
Acceptable Workload in Heavy Dynamic Muscular Work
The assessment of acceptable workload in dynamic work tasks has traditionally been based on measurements of oxygen consumption (or, correspondingly, energy expenditure). Oxygen consumption can be measured with relative ease in the field with portable devices (e.g., Douglas bag, Max Planck respirometer, Oxylog, Cosmed), or it can be estimated from heart rate recordings, which can be made reliably at the workplace, for example, with the SportTester device. The use of heart rate in the estimation of oxygen consumption requires that it be individually calibrated against measured oxygen consumption in a standard work mode in the laboratory, i.e., the investigator must know the oxygen consumption of the individual subject at a given heart rate. Heart rate recordings should be treated with caution because they are also affected by such factors as physical fitness, environmental temperature, psychological factors and size of active muscle mass. Thus, heart rate measurements can lead to overestimates of oxygen consumption in the same way that oxygen consumption values can give rise to underestimates of global physiological strain by reflecting only energy requirements.
Relative aerobic strain (RAS) is defined as the fraction (expressed as a percentage) of a worker’s oxygen consumption measured on the job relative to his or her VO2max measured in the laboratory. If only heart rate measurements are available, a close approximation to RAS can be made by calculating a value for percentage heart rate range (% HR range) with the so-called Karvonen formula as in figure 3.
VO2max is usually measured on a bicycle ergometer or treadmill, for which the mechanical efficiency is high (20-25%). When the active muscle mass is smaller or the static component is higher, VO2max and mechanical efficiency will be smaller than in the case of exercise with large muscle groups. For example, it has been found that in the sorting of postal parcels the VO2max of workers was only 65% of the maximum measured on a bicycle ergometer, and the mechanical efficiency of the task was less than 1%. When guidelines are based on oxygen consumption, the test mode in the maximal test should be as close as possible to the real task. This goal, however, is difficult to achieve.
According to Åstrand’s (1960) classical study, RAS should not exceed 50% during an eight-hour working day. In her experiments, at a 50% workload, body weight decreased, heart rate did not reach steady state and subjective discomfort increased during the day. She recommended a 50% RAS limit for both men and women. Later on she found that construction workers spontaneously chose an average RAS level of 40% (range 25-55%) during a working day. Several more recent studies have indicated that the acceptable RAS is lower than 50%. Most authors recommend 30-35% as an acceptable RAS level for the entire working day.
Originally, the acceptable RAS levels were developed for pure dynamic muscle work, which rarely occurs in real working life. It may happen that acceptable RAS levels are not exceeded, for example, in a lifting task, but the local load on the back may greatly exceed acceptable levels. Despite its limitations, RAS determination has been widely used in the assessment of physical strain in different jobs.
In addition to the measurement or estimation of oxygen consumption, other useful physiological field methods are also available for the quantification of physical stress or strain in heavy dynamic work. Observational techniques can be used in the estimation of energy expenditure (e.g., with the aid of the Edholm scale) (Edholm 1966). Rating of perceived exertion (RPE) indicates the subjective accumulation of fatigue. New ambulatory blood pressure monitoring systems allow more detailed analyses of circulatory responses.
Acceptable Workload in Manual Materials Handling
Manual materials handling includes such work tasks as lifting, carrying, pushing and pulling of various external loads. Most of the research in this area has focused on low back problems in lifting tasks, especially from the biomechanical point of view.
A RAS level of 20-35% has been recommended for lifting tasks, when the task is compared to an individual maximum oxygen consumption obtained from a bicycle ergometer test.
Recommendations for a maximum permissible heart rate are either absolute or related to the resting heart rate. The absolute values for men and women are 90-112 beats per minute in continuous manual materials handling. These values are about the same as the recommended values for the increase in heart rate above resting levels, that is, 30 to 35 beats per minute. These recommendations are also valid for heavy dynamic muscle work for young and healthy men and women. However, as mentioned previously, heart rate data should be treated with caution, because it is also affected by other factors than muscle work.
The guidelines for acceptable workload for manual materials handling based on biomechanical analyses comprise several factors, such as weight of the load, handling frequency, lifting height, distance of the load from the body and physical characteristics of the person.
In one large-scale field study (Louhevaara, Hakola and Ollila 1990) it was found that healthy male workers could handle postal parcels weighing 4 to 5 kilograms during a shift without any signs of objective or subjective fatigue. Most of the handling occurred below shoulder level, the average handling frequency was less than 8 parcels per minute and the total number of parcels was less than 1,500 per shift. The mean heart rate of the workers was 101 beats per minute and their mean oxygen consumption 1.0 l/min, which corresponded to 31% RAS as related to bicycle maximum.
Observations of working postures and use of force carried out for example according to OWAS method (Karhu, Kansi and Kuorinka 1977), ratings of perceived exertion and ambulatory blood pressure recordings are also suitable methods for stress and strain assessments in manual materials handling. Electromyography can be used to assess local strain responses, for example in arm and back muscles.
Acceptable Workload for Static Muscular Work
Static muscular work is required chiefly in maintaining working postures. The endurance time of static contraction is exponentially dependent on the relative force of contraction. This means, for example, that when the static contraction requires 20% of the maximum force, the endurance time is 5 to 7 minutes, and when the relative force is 50%, the endurance time is about 1 minute.
Older studies indicated that no fatigue will be developed when the relative force is below 15% of the maximum force. However, more recent studies have indicated that the acceptable relative force is specific to the muscle or muscle group, and is 2 to 5% of the maximum static strength. These force limits are, however, difficult to use in practical work situations because they require electromyographic recordings.
For the practitioner, fewer field methods are available for the quantification of strain in static work. Some observational methods (e.g., the OWAS method) exist to analyse the proportion of poor working postures, that is, postures deviating from normal middle positions of the main joints. Blood pressure measurements and ratings of perceived exertion may be useful, whereas heart rate is not so applicable.
Acceptable Workload in Repetitive Work
Repetitive work with small muscle groups resembles static muscle work from the point of view of circulatory and metabolic responses. Typically, in repetitive work muscles contract over 30 times per minute. When the relative force of contraction exceeds 10% of the maximum force, endurance time and muscle force start to decrease. However, there is wide individual variation in endurance times. For example, the endurance time varies between two to fifty minutes when the muscle contracts 90 to 110 times per minute at a relative force level of 10 to 20% (Laurig 1974).
It is very difficult to set any definitive criteria for repetitive work, because even very light levels of work (as with the use of a microcomputer mouse) may cause increases in intramuscular pressure, which may sometimes lead to swelling of muscle fibres, pain and reduction in muscle strength.
Repetitive and static muscle work will cause fatigue and reduced work capacity at very low relative force levels. Therefore, ergonomic interventions should aim to minimize the number of repetitive movements and static contractions as far as possible. Very few field methods are available for strain assessment in repetitive work.
Prevention of Muscular Overload
Relatively little epidemiological evidence exists to show that muscular load is harmful to health. However, work physiological and ergonomic studies indicate that muscular overload results in fatigue (i.e., decrease in work capacity) and may reduce productivity and quality of work.
The prevention of muscular overload may be directed to the work content, the work environment and the worker. The load can be adjusted by technical means, which focus on the work environment, tools, and/or the working methods. The fastest way to regulate muscular workload is to increase the flexibility of working time on an individual basis. This means designing work-rest regimens which take into account the workload and the needs and capacities of the individual worker.
Static and repetitive muscular work should be kept at a minimum. Occasional heavy dynamic work phases may be useful for the maintenance of endurance type physical fitness. Probably, the most useful form of physical activity that can be incorporated into a working day is brisk walking or stair climbing.
Prevention of muscular overload, however, is very difficult if a worker’s physical fitness or working skills are poor. Appropriate training will improve working skills and may reduce muscular loads at work. Also, regular physical exercise during work or leisure time will increase the muscular and cardio-respiratory capacities of the worker.
Anthropometry
This article is adapted from the 3rd edition of the Encyclopaedia of Occupational Health and Safety.
Anthropometry is a fundamental branch of physical anthropology. It represents the quantitative aspect. A wide system of theories and practice is devoted to defining methods and variables to relate the aims in the different fields of application. In the fields of occupational health, safety and ergonomics anthropometric systems are mainly concerned with body build, composition and constitution, and with the dimensions of the human body’s interrelation to workplace dimensions, machines, the industrial environment, and clothing.
Anthropometric variables
An anthropometric variable is a measurable characteristic of the body that can be defined, standardized and referred to a unit of measurement. Linear variables are generally defined by landmarks that can be precisely traced to the body. Landmarks are generally of two types: skeletal-anatomical, which may be found and traced by feeling bony prominences through the skin, and virtual landmarks that are simply found as maximum or minimum distances using the branches of a caliper.
Anthropometric variables have both genetic and environmental components and may be used to define individual and population variability. The choice of variables must be related to the specific research purpose and standardized with other research in the same field, as the number of variables described in the literature is extremely large, up to 2,200 having been described for the human body.
Anthropometric variables are mainly linear measures, such as heights, distances from landmarks with subject standing or seated in standardized posture; diameters, such as distances between bilateral landmarks; lengths, such as distances between two different landmarks; curved measures, namely arcs, such as distances on the body surface between two landmarks; and girths, such as closed all-around measures on body surfaces, generally positioned at at least one landmark or at a defined height.
Other variables may require special methods and instruments. For instance skinfold thickness is measured by means of special constant pressure calipers. Volumes are measured by calculation or by immersion in water. To obtain full information on body surface characteristics, a computer matrix of surface points may be plotted using biostereometric techniques.
Instruments
Although sophisticated anthropometric instruments have been described and used with a view to automated data collection, basic anthropometric instruments are quite simple and easy to use. Much care must be taken to avoid common errors resulting from misinterpretation of landmarks and incorrect postures of subjects.
The standard anthropometric instrument is the anthropometer—a rigid rod 2 metres long, with two counter-reading scales, with which vertical body dimensions, such as heights of landmarks from floor or seat, and transverse dimensions, such as diameters, can be taken.
Commonly the rod can be split into 3 or 4 sections which fit into one another. A sliding branch with a straight or curved claw makes it possible to measure distances from the floor for heights, or from a fixed branch for diameters. More elaborate anthropometers have a single scale for heights and diameters to avoid scale errors, or are fitted with digital mechanical or electronic reading devices (figure 1).
A stadiometer is a fixed anthropometer, generally used only for stature and frequently associated with a weight beam scale.
For transverse diameters a series of calipers may be used: the pelvimeter for measures up to 600 mm and the cephalometer up to 300 mm. The latter is particularly suitable for head measurements when used together with a sliding compass (figure 2).
Figure 2. A cephalometer together with a sliding compass
The foot-board is used for measuring the feet and the head-board provides cartesian co-ordinates of the head when oriented in the “Frankfort plane” (a horizontal plane passing through porion and orbitale landmarks of the head).The hand may be measured with a caliper, or with a special device composed of five sliding rulers.
Skinfold thickness is measured with a constant-pressure skinfold caliper generally with a pressure of 9.81 x 104 Pa (the pressure imposed by a weight of 10 g on an area of 1 mm2).
For arcs and girths a narrow, flexible steel tape with flat section is used. Self-straightening steel tapes must be avoided.
Systems of variables
A system of anthropometric variables is a coherent set of body measurements to solve some specific problems.
In the field of ergonomics and safety, the main problem is fitting equipment and workspace to humans and tailoring clothes to the right size.
Equipment and workspace require mainly linear measures of limbs and body segments that can easily be calculated from landmark heights and diameters, whereas tailoring sizes are based mainly on arcs, girths and flexible tape lengths. Both systems may be combined according to need.
In any case, it is absolutely necessary to have a precise space reference for each measurement. The landmarks must, therefore, be linked by heights and diameters and every arc or girth must have a defined landmark reference. Heights and slopes must be indicated.
In a particular survey, the number of variables has to be limited to the minimum so as to avoid undue stress on the subject and operator.
A basic set of variables for workspace has been reduced to 33 measured variables (figure 3) plus 20 derived by a simple calculation. For a general-purpose military survey, Hertzberg and co-workers use 146 variables. For clothes and general biological purposes the Italian Fashion Board (Ente Italiano della Moda) uses a set of 32 general purpose variables and 28 technical ones. The German norm (DIN 61 516) of control body dimensions for clothes includes 12 variables. The recommendation of the International Organization for Standardization (ISO) for anthropometry includes a core list of 36 variables (see table 1). The International Data on Anthropometry tables published by the ILO list 19 body dimensions for the populations of 20 different regions of the world (Jürgens, Aune and Pieper 1990).
Figure 3. Basic set of anthropometric variables
Table 1. Basic anthropometric core list
1.1 Forward reach (to hand grip with subject standing upright against a wall)
1.2 Stature (vertical distance from floor to head vertex)
1.3 Eye height (from floor to inner eye corner)
1.4 Shoulder height (from floor to acromion)
1.5 Elbow height (from floor to radial depression of elbow)
1.6 Crotch height (from floor to pubic bone)
1.7 Finger tip height (from floor to grip axis of fist)
1.8 Shoulder breadth (biacromial diameter)
1.9 Hip breadth, standing (the maximum distance across hips)
2.1 Sitting height (from seat to head vertex)
2.2 Eye height, sitting (from seat to inner corner of the eye)
2.3 Shoulder height, sitting (from seat to acromion)
2.4 Elbow height, sitting (from seat to lowest point of bent elbow)
2.5 Knee height (from foot-rest to the upper surface of thigh)
2.6 Lower leg length (height of sitting surface)
2.7 Forearm-hand length (from back of bent elbow to grip axis)
2.8 Body depth, sitting (seat depth)
2.9 Buttock-knee length (from knee-cap to rearmost point of buttock)
2.10 Elbow to elbow breadth (distance between lateral surface of the elbows)
2.11 Hip breadth, sitting (seat breadth)
3.1 Index finger breadth, proximal (at the joint between medial and proximal phalanges)
3.2 Index finger breadth, distal (at the joint between distal and medial phalanges)
3.3 Index finger length
3.4 Hand length (from tip of middle finger to styloid)
3.5 Handbreadth (at metacarpals)
3.6 Wrist circumference
4.1 Foot breadth
4.2 Foot length
5.1 Heat circumference (at glabella)
5.2 Sagittal arc (from glabella to inion)
5.3 Head length (from glabella to opisthocranion)
5.4 Head breadth (maximum above the ear)
5.5 Bitragion arc (over the head between the ears)
6.1 Waist circumference (at the umbilicus)
6.2 Tibial height (from the floor to the highest point on the antero-medial margin of the glenoid of the tibia)
6.3 Cervical height sitting (to the tip of the spinous process of the 7th cervical vertebra).
Source: Adapted from ISO/DP 7250 1980).
Precision and errors
The precision of living body dimensions must be considered in a stochastic manner because the human body is highly unpredictable, both as a static and as a dynamic structure.
A single individual may grow or change in muscularity and fatness; undergo skeletal changes as a consequence of aging, disease or accidents; or modify behavior or posture. Different subjects differ by proportions, not only by general dimensions. Tall stature subjects are not mere enlargements of short ones; constitutional types and somatotypes probably vary more than general dimensions.
The use of mannequins, particularly those representing the standard 5th, 50th and 95th percentiles for fitting trials may be highly misleading, if body variations in body proportions are not taken into consideration.
Errors result from misinterpretation of landmarks and incorrect use of instruments (personal error), imprecise or inexact instruments (instrumental error), or changes in subject posture (subject error—this latter may be due to difficulties of communication if the cultural or linguistic background of the subject differs from that of the operator).
Statistical treatment
Anthropometric data must be treated by statistical procedures, mainly in the field of inference methods applying univariate (mean, mode, percentiles, histograms, variance analysis, etc.), bivariate (correlation, regression) and multivariate (multiple correlation and regression, factor analysis, etc.) methods. Various graphical methods based on statistical applications have been devised to classify human types (anthropometrograms, morphosomatograms).
Sampling and survey
As anthropometric data cannot be collected for the whole population (except in the rare case of a particularly small population), sampling is generally necessary. A basically random sample should be the starting point of any anthropometric survey. To keep the number of measured subjects to a reasonable level it is generally necessary to have recourse to multiple-stage stratified sampling. This allows the most homogeneous subdivision of the population into a number of classes or strata.
The population may be subdivided by sex, age group, geographical area, social variables, physical activity and so on.
Survey forms have to be designed keeping in mind both measuring procedure and data treatment. An accurate ergonomic study of the measuring procedure should be made in order to reduce the operator’s fatigue and possible errors. For this reason, variables must be grouped according to the instrument used and ordered in sequence so as to reduce the number of body flexions the operator has to make.
To reduce the effect of personal error, the survey should be carried out by one operator. If more than one operator has to be used, training is necessary to assure the replicability of measurements.
Population anthropometrics
Disregarding the highly criticized concept of “race”, human populations are nevertheless highly variable in size of individuals and in size distribution. Generally human populations are not strictly Mendelian; they are commonly the result of admixture. Sometimes two or more populations, with different origins and adaptation, live together in the same area without interbreeding. This complicates the theoretical distribution of traits. From the anthropometric viewpoint, sexes are different populations. Populations of employees may not correspond exactly to the biological population of the same area as a consequence of possible aptitudinal selection or auto-selection due to job choice.
Populations from different areas may differ as a consequence of different adaptation conditions or biological and genetic structures.
When close fitting is important a survey on a random sample is necessary.
Fitting trials and regulation
The adaptation of workspace or equipment to the user may depend not only on the bodily dimensions, but also on such variables as tolerance of discomfort and nature of activities, clothing, tools and environmental conditions. A combination of a checklist of relevant factors, a simulator and a series of fitting trials using a sample of subjects chosen to represent the range of body sizes of the expected user population can be used.
The aim is to find tolerance ranges for all subjects. If the ranges overlap it is possible to select a narrower final range that is not outside the tolerance limits of any subject. If there is no overlap it will be necessary to make the structure adjustable or to provide it in different sizes. If more than two dimensions are adjustable a subject may not be able to decide which of the possible adjustments will fit him best.
Adjustability can be a complicated matter, especially when uncomfortable postures result in fatigue. Precise indications must, therefore, be given to the user who frequently knows little or nothing about his own anthropometric characteristics. In general, an accurate design should reduce the need for adjustment to the minimum. In any case, it should constantly be kept in mind what is involved is anthropometrics, not merely engineering.
Dynamic anthropometrics
Static anthropometrics may give wide information about movement if an adequate set of variables has been chosen. Nevertheless, when movements are complicated and a close fit with the industrial environment is desirable, as in most user-machine and human-vehicle interfaces, an exact survey of postures and movements is necessary. This may be done with suitable mock-ups that allow tracing of reach lines or by photography. In this case, a camera fitted with a telephoto lens and an anthropometric rod, placed in the sagittal plane of the subject, allows standardized photographs with little distortion of the image. Small labels on subjects’ articulations make the exact tracing of movements possible.
Another way of studying movements is to formalize postural changes according to a series of horizontal and vertical planes passing through the articulations. Again, using computerized human models with computer-aided design (CAD) systems is a feasible way to include dynamic anthropometrics in ergonomic workplace design.
" DISCLAIMER: The ILO does not take responsibility for content presented on this web portal that is presented in any language other than English, which is the language used for the initial production and peer-review of original content. Certain statistics have not been updated since the production of the 4th edition of the Encyclopaedia (1998)."