Children categories

53. Environmental Health Hazards (11)

53. Environmental Health Hazards
Chapter Editors: Annalee Yassi and Tord Kjellström
Table of Contents
Tables and Figures
Linkages between Environmental and Occupational Health
Annalee Yassi and Tord Kjellström
Food and Agriculture
Friedrich K. Käferstein
Industrial Pollution in Developing Countries
Niu Shiru
Developing Countries and Pollution
Tee L. Guidotti
Air Pollution
Isabelle Romieu
Land Pollution
Tee L. Guidotti and Chen Weiping
Water Pollution
Ivanildo Hespanhol and Richard Helmer
Energy and Health
L.D. Hamilton
Urbanization
Edmundo Werna
Global Climate Change and Ozone Depletion
Jonathan A. Patz
Species Extinction, Biodiversity Loss and Human Health
Eric Chivian
Tables
Click a link below to view table in article context.
1. Selected major "environmental disease" outbreaks
2. Foodborne-disease agents: epidemiology features
3. Major sources of outdoor air pollutants
4. Exposure-response relationship of PM10
5. Changes in ozone concentration: health outcomes
6. Morbidity & mortality: water-related diseases
7. Generating fuel electricity: health effects
8. Generating renewable electricity: health effects
9. Generating nuclear electricity: health effects
10. Housing & health
11. Urban infrastructure & health
12. Global status of major vector-borne diseases
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

54. Environmental Policy (10)

54. Environmental Policy
Chapter Editor: Larry R. Kohler
Table of Contents
Tables and Figures
Overview Occupational Safety and Health and the Environment - Two Sides of the Same Coin
Larry R. Kohler
Environment and the World of Work: An Integrated Approach to Sustainable Development, Environment and the Working Environment
Larry R. Kohler
Law and Regulations
Françoise Burhenne-Guilmin
International Environmental Conventions
David Freestone
Environmental Impact Assessments
Ron Bisset
Life-Cycle Assessment (Cradle-To-Grave)
Sven-Olof Ryding
Risk Assessment and Communication
Adrian V. Gheorghe and Hansjörg Seiler
Environmental Auditing - Definition and Methodology
Robert Coyle
Environmental Management Strategies and Workers’ Protection
Cecilia Brighi
Environmental Pollution Control: Making Pollution Prevention a Corporate Priority
Robert P. Bringer and Tom Zosel
Tables
Click a link below to view table in article context.
1. Scope of an environmental audit
2. Basic steps in environmental auditing
3. Voluntary agreements relevant to the environment
4. Environment-protection measures & collective agreements
5. Collective agreements on environment-protection
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.

55. Environmental Pollution Control (11)

55. Environmental Pollution Control
Chapter Editors: Jerry Spiegel and Lucien Y. Maystre
Table of Contents
Tables and Figures
Environmental Pollution Control and Prevention
Jerry Spiegel and Lucien Y. Maystre
Air Pollution Management
Dietrich Schwela and Berenice Goelzer
Air Pollution: Modelling of Air Pollutant Dispersion
Marion Wichmann-Fiebig
Air Quality Monitoring
Hans-Ulrich Pfeffer and Peter Bruckmann
Air Pollution Control
John Elias
Water Pollution Control
Herbert C. Preul
Dan Region Sewage Reclamation Project: A Case Study
Alexander Donagi
Principles of Waste Management
Lucien Y. Maystre
Solid Waste Management and Recycling
Niels Jorn Hahn and Poul S. Lauridsen
Case Study: Canadian Multimedia Pollution Control and Prevention on the Great Lakes
Thomas Tseng, Victor Shantora and Ian R. Smith
Cleaner Production Technologies
David Bennett
Tables
Click a link below to view table in article context.
1. Common atmospheric pollutants & their sources
2. Measurement planning parameters
3. Manual measurement procedures for inorganic gases
4. Automated measurement procedures for inorganic gases
5. Measurement procedures for suspended particulate
6. Long-distance measurement procedures
7. Chromatographic air quality measurement procedures
8. Systematic air quality monitoring in Germany
9. Steps in selecting pollution controls
10. Air quality standards for sulphur dioxide
11. Air quality standards for benzene
12. Examples of best available control technology
13. Industrial gas: cleaning methods
14. Sample emission rates for industrial processes
15. Wastewater treatment operations & processes
16. List of investigated parameters
17. Parameters investigated at the recovery wells
18. Sources of waste
19. Criteria for selection of substances
20. Reductions in releases of dioxin & furan in Canada
Figures
Point to a thumbnail to see figure caption, click to see figure in article context.
Linkages Between Environmental and Occupational Health
Development, and industrialization in particular, have made immense positive contributions to health, including greater personal and social wealth, as well as vastly improved health and education services, transportation and communication. Unquestionably, on the global scale, people are living longer and are healthier than they were centuries and even decades ago. However, industrialization has also had adverse health consequences not only for workforces, but for the general population as well. These effects have been caused either directly by exposure to safety hazards and harmful agents, or indirectly through environmental degradation locally and globally (see “Industrial pollution in developing countries” in this chapter).
This article outlines the nature of environmental health hazards and the reasons for linking environmental health with occupational health.
Environmental health hazards, like occupational health hazards, may be biological, chemical, physical, biomechanical or psychosocial in nature. Environmental health hazards include traditional hazards of poor sanitation and shelter, as well as agricultural and industrial contamination of air, water, food and land. These hazards have resulted in a host of health impacts, ranging from catastrophic direct effects (e.g., the recent cholera epidemic in Latin America and the chemical poisoning outbreak in Bhopal, India), to chronic effects (e.g., in Minamata, Japan), to subtle, indirect, and even disputed effects (e.g., in Love Canal, USA). Table 1 summarizes some of the major notorious disasters in the last half century that have caused “environmental disease” outbreaks. There are undeniably countless other examples of environmental disease outbreaks, some of which are not easily detectable on the macrostatistical level. Meanwhile, over a billion people in the world lack access to safe drinking water (WHO 1992b) and over 600 million are exposed to ambient levels of sulphur dioxide that well exceed recommended levels. Moreover the pressure on agriculture and food production as both population and per capita demand increase, will likely lead to a greater burden on the environment (see “Food and agriculture” in this chapter). Environmental health impacts thus include the indirect effects of industrial disruption of adequate food and housing, as well as the degradation of the global systems on which the health of the planet depends.
Table 1. Selected major "environmental disease" outbreaks
|
Location and year |
Environmental hazard |
Type of disease |
Number affected |
|
London, UK 1952 |
Severe air-pollution with sulphur dioxide and suspended particulate matter (SPM) |
Increase in heart and lung disease manifestations |
3,000 deaths, many others ill |
|
Toyama, Japan 1950s |
Cadmium in rice |
Kidney and bone disease (“Itai-itai disease”) |
200 with severe disease, many more with slight effects |
|
South-east Turkey 1955-61 |
Hexachlorobenzene in seed grains |
Porphyria; neurological disease |
3,000 |
|
Minamata, Japan 1956 |
Methylmercury in fish |
Neurological disease (“Minimata disease”) |
200 with severe disease, 2,000 suspected |
|
USA cities 1960s-70s |
Lead in paint |
Anaemia, behavioural and mental effects |
Many thousands |
|
Fukuoka, Japan 1968 |
Polychlorinated biphenyls (PCBs) in food oil |
Skin disease, general weakness |
Several thousands |
|
Iraq 1972 |
Methylmercury in seed grains |
Neurological disease |
500 deaths, 6,500 hospitalized |
|
Madrid, Spain 1981 |
Aniline or other toxin in food oil |
Various symptoms |
340 deaths, 20,000 cases |
|
Bhopal, India 1985 |
Methylisocyanate |
Acute lung disease |
2,000 deaths, 200,000 poisoned |
|
California, USA 1985 |
Carbamate pesticide in watermelons |
Gastrointestinal, skeletal, muscle, autonomic and central nervous system effects (Carbamate illness) |
1,376 reported cases of illness resulting from consumption, 17 severely ill |
|
Chernobyl, USSR 1986 |
Iodine-134, Caesium-134 and -137 from a reactor explosion |
Radiation illness (including increases in cancer and thyroid diseases in children) |
300 injured, 28 died within 3 months, more than 600 cases of thyroid cancer |
|
Goiánia, Brazil 1987 |
Caesium-137 from an abandoned cancer therapy machine |
Radiation illness (follow-up of in utero exposures continuing) |
Some 240 people were contaminated and 2 died |
|
Peru 1991 |
Cholera epidemic |
Cholera |
139 deaths, many thousand ill |
In many countries large-scale agriculture and the concomitant active use of toxic pesticides is a major health hazard both for workers and for their households. Pollution by fertilizers or biological waste from the food industry, paper industry and so on can also have harmful effects on waterways, reducing fishing and food supplies. The fishermen and gatherers of other seafood may have to travel much further to get their daily catch, with increased risks of drowning accidents and other mishaps. The spread of tropical disease by the environmental changes associated with developments such as the building of dams, roads and so on constitutes another type of environmental health risk. The new dam may create breeding grounds for schistosomiasis, a debilitating disease affecting rice farmers who have to walk in water. The new road may create fast communication between an area with endemic malaria and another area hitherto spared from this disease.
It should be pointed out that the major basis for a harmful environment in the workplace or in the general environment is poverty. The traditional health threats in developing countries or in poor sections of any country include poor sanitation, water and food which spreads communicable diseases, poor housing with high exposures to cooking smoke and high fire risks, as well as high injury risks in small-scale agriculture or cottage industries. Reduction of poverty and improved living and working conditions is a fundamental priority for improved occupational and environmental health for billions of people. Despite efforts for energy conservation and sustainable development, failure to address the underlying inequities in wealth distribution threatens the global ecosystem.
Forests, for example, which represent the culmination of ecological successional processes, are being destroyed at an alarming rate, due to commercial logging and clearance by impoverished peoples for agriculture and firewood. The effects of forest depletion include soil erosion, which, if extreme, can lead to desertification. Loss of biodiversity is an important consequence (see “Species extinction, biodiversity loss and human health” in this chapter). It is estimated that one-third of all carbon dioxide emissions are from the burning of tropical forests (the importance of carbon dioxide in creating global warming is discussed in “Global climate change and ozone depletion” in this chapter). Thus, addressing poverty is imperative with respect to global environmental health as well as individual, community and regional well-being.
Reasons for Linking Environmental and Occupational Health
The main link between the workplace and the general environment is that the source of the hazard is usually the same, whether it is an agricultural activity or an industrial activity. In order to control the health hazard, a common approach may work effectively in both settings. This is particularly so when it comes to the choice of chemical technologies for production. If an acceptable result or product can be produced with a less toxic chemical, the choice of such a chemical can reduce or even eliminate the health risk. One example is the use of safer water-based paints instead of paints made with toxic organic solvents. Another example is the choice of non-chemical pest-control methods whenever this is possible. In fact, in many cases, particularly in the developing world, there is no separation between the home and the workplace; thus the setting is truly the same.
It is now well recognized that the scientific knowledge and training required to assess and control environmental health hazards are, for the most part, the same skills and knowledge required to address health hazards within the workplace. Toxicology, epidemiology, occupational hygiene, ergonomics, safety engineering - in fact, the very disciplines included in this Encyclopaedia - are the basic tools of environmental science. The process of risk assessment and risk management is also the same: identify the hazards, categorize the risks, assess the exposure and estimate risk. This is followed by evaluating control options, controlling the exposure, communicating the risk to the public and establishing an on-going exposure- and risk-monitoring programme. Thus occupational and environmental health are strongly linked by common methodologies, particularly in health assessment and exposure control.
The identification of environmental health hazards has often come from observations of adverse health outcomes among workers; and unquestionably it is in the workplace that the impact of industrial exposures is best understood. Documentation of health effects generally comes from one of three sources: animal or other laboratory experiments (both non-human and controlled human), accidental high-level exposures or the epidemiological studies that usually follow such exposures. To conduct an epidemiological study it is necessary to be able to define both the exposed population and the nature and level of the exposure, as well as to ascertain the negative health effect. It is generally easier to define the members of a workforce than to determine the membership of a community, particularly in a community that is transient; the nature and level of exposure to various members of the cohort are generally more clear-cut in a workplace population than in a community; and the outcomes of high levels of exposure are almost always easier to delineate than more subtle changes attributable to low-level exposure. While there are some examples of exposure outside factory gates approaching the worst occupational exposures (e.g., cadmium exposure from mining in China and Japan; lead and cadmium emissions from smelters in Upper Silesia, Poland), the levels of exposure are generally much higher to a workforce than to the surrounding community (WHO 1992b).
Since adverse health outcomes are more apparent in workers, information on occupational health effects of many toxic exposures (including heavy metals such as lead, mercury, arsenic and nickel, as well as such well-known carcinogens as asbestos) has been used to calculate the health risk to the wider community. With respect to cadmium, for example, as early as 1942 reports began to appear of cases of osteomalacia with multiple fractures among workers in a French factory producing alkaline batteries. During the 1950s and 1960s cadmium intoxication was considered to be strictly an occupational disease. However, the knowledge gained from the workplace helped achieve the recognition that osteomalacia and kidney disease that was occurring in Japan at this time, “Itai-itai” disease, was indeed due to contamination of rice from irrigation of soil with water contaminated with cadmium from industrial sources (Kjellström 1986). Thus occupational epidemiology has been able to make a substantive contribution to knowledge of the effects of environmental exposure, constituting another reason for linking the two fields.
On an individual level, occupational disease affects well-being in the home and the community; and, universally, an individual who is ill from inadequacies in the home and the community cannot be productive in the workplace.
Strictly from a scientific viewpoint, there is a need to consider total (environmental plus occupational) exposures in order to truly assess health impact and establish dose-response relationships. Pesticide exposure is a classic example wherein occupational exposure may be supplemented by considerable environmental exposure, through food and water-source contamination, and through non-occupational airborne exposure. From outbreaks in which over 100 poisonings occurred from contaminated food alone, over 15,000 cases and 1,500 deaths due to pesticide poisoning have been documented by the WHO (1990e). In one study of Central American cotton growers using pesticides, not only did very few of the workers have access to protective clothing, but virtually all of the workers lived within 100 metres of the cotton fields, many in temporary housing with no walls for protection from aerial pesticide spraying. The workers also often washed in irrigation channels containing pesticide residues, resulting in increased exposures (Michaels, Barrera and Gacharna 1985). To understand the relationship between pesticide exposure and any health effects reported, all sources of exposure should be taken into consideration. Thus ensuring that occupational and environmental exposures are evaluated together improves the accuracy of exposure assessment in both areas.
The health problems caused by occupational and environmental hazards are particularly acute in developing countries, where well established methods of hazard control are less likely to be applied because of limited awareness of the hazards, low political priority of health and environment matters, limited resources or lack of appropriate occupational and environmental health management systems. A major impediment to environmental health hazard control in many parts of the world is the lack of people with appropriate training. It has been documented that developing countries suffer from a severe shortage of expert staff in occupational health (Noweir 1986). In 1985 a WHO expert committee also concluded that there is an urgent need for staff trained in environmental health matters; indeed Agenda 21, the internationally agreed upon strategy taken by the United Nations Conference on Environment and Development (UN 1993), identifies training (national “capacity building”) as a key element of promoting human health through sustainable development. Where resources are limited, it is not feasible to train one group of people to look after health concerns within the workplace, and another group to attend to hazards outside the factory gate.
Even in developed countries, there is a strong trend to make most efficient use of resources by training and employing “occupational and environmental health” professionals. Today, businesses must find ways to manage their affairs logically and efficiently within the societal framework of duty, law and financial policy. Combining occupational and environment health under one roof is one way of achieving this goal.
Broad environmental concerns must be taken into consideration in designing workplaces and deciding on industrial hygiene control strategies. Substituting for one substance another one that is less acutely toxic may make good occupational health sense; however, if the new substance is not biodegradable, or damages the ozone layer, it would not be an appropriate exposure control solution—it would only move the problem elsewhere. The use of chlorofluorocarbons, now widely used as a refrigerant instead of the more acutely dangerous substance ammonia, is the classic example of what is now known to have been an environmentally inappropriate substitution. Thus linking occupational and environmental health minimizes unwise exposure control decisions.
While understanding of the health effects of various deleterious exposures has usually come from the workplace, the public health impact of environmental exposures to these same agents has often been a major force in stimulating clean-up efforts both inside the workplace and in the surrounding community. For example, discovery of high lead levels in workers’ blood by an industrial hygienist in a lead foundry in Bahia, Brazil, led to investigations of lead in the blood of children in nearby residential areas. The finding that the children had high lead levels was a major impetus in the company taking action to reduce occupational exposures as well as lead emissions from the factory (Nogueira 1987), although occupational exposures still remain substantially higher than would be tolerated by the general community.
In fact, environmental health standards are usually much stricter than occupational health standards. The WHO’s recommended guideline values for selected chemicals provide an example. The rationale for the difference is generally that the community consists of sensitive populations including the very old, the ill, young children and pregnant women, whereas the workforce is at least healthy enough to work. Also, it is often argued that risk is more “acceptable” to a workforce, as these people are benefiting by having a job, and are therefore more willing to accept the risk. Many political, ethical, as well as scientific, debates rage around the question of standards. Linking occupational and environmental health can be a positive contribution to sorting out these controversies. In this regard, tightening the connection between occupational and environmental health may facilitate greater consistency in approaches to standard setting.
Likely inspired at least in part by the active debate about the environment and sustainable development brought to the forefront by Agenda 21, many occupational health professional organizations have changed their names to “occupational and environmental” organizations in acknowledgement that their members are increasingly devoting their attention to environmental health hazards both inside and outside the workplace. Further, as noted in the chapter on ethics , the International Code of Ethics for Occupational Health Professionals states that the duty to protect the environment is part and parcel of the ethical obligations of occupational health professionals.
In summary, occupational and environmental health are strongly linked by:
- the very fact that the source of the health threat is usually the same
- common methodologies, particularly in health assessment and exposure control
- the contribution that occupational epidemiology makes to knowledge of the effects of environmental exposure
- the effects that occupational disease has on well-being in the home and the community, and conversely the effect of environmental pathology on worker productivity
- the scientific need to consider total exposures in order to determine dose-response relationships
- the efficiency in human resource development and utilization gained by such a linkage
- improvements in exposure control decisions stemming from the broader view
- greater consistency in standard setting facilitated by the link
- the fact that linking environmental and occupational health enhances the incentive for rectification of hazards to both the workforce and the community.
The desirability of bringing together occupational and environmental health notwithstanding, each has a unique and specific orientation that should not be lost. Occupational health must continue to focus on workers’ health, and environmental health must continue to concern itself with the health of the general public. None the less, even where it is desirable for professionals to operate strictly in only one of these fields, having a good appreciation of the other enhances the credibility, knowledge base and effectiveness of the overall endeavour. It is in this spirit that this chapter is presented.
Food and Agriculture
This article has been prepared by Dr F. Käferstein, Chief, Food Safety, World Health Organization. It is entirely based on the report of a WHO Panel on Food and Agriculture which had supported the WHO Commission on Health and Environment to prepare a report for the United Nations Conference on Environment and Development (UNCED), Rio de Janeiro, 1992. Both reports are available from the WHO.
Production Needs in the Face of Population Pressure and Other Forces
Rapid population growth continues in some regions of the world. As compared with the situation in 1990, by the year 2010 there will be an extra 1,900 million people to be fed, a rise of 36% from 5,300 to 7,200 million people.
Ninety per cent of the entire projected growth over the next 20 years is expected to take place in the countries which are currently classified as developing nations. Progressive urbanization of society is taking place. The urban population of the world will reach 3,600 million, a rise of 62% from the 2,200 million city dwellers in 1990. Moreover the urban population of developing countries will increase by 92% (from 1,400 million to 2,600 million) in the twenty years from 1990, a fourfold increase since 1970. Even if family planning receives the urgent attention that it desperately requires from all rapidly growing populations, population growth and urbanization will continue to dominate the scene for the next two decades.
A 36% increase in food, other agricultural products and potable water will be required over the next twenty years simply to match the rise in population; the need for half a billion people to be properly fed instead of remaining undernourished, and the greater demand from populations with a rising income, will all lead to a vast increase in total food production. An excessive demand for food of animal origin will continue to characterize people in the higher income groups, leading to increases in animal feed production.
The pressure on agriculture and food production, as both population and per capita demand increase, will lead to a greater burden on the environment. This burden will be unevenly generated and have uneven environmental effects. Globally, these will be adverse and will require concerted action.
This increased demand will fall on resources of land and water which are finite, where the most productive areas have already been used, and where the cost of bringing marginal land into production, and of using less readily available water, will be high. Much of this marginal land may have only temporary fertility unless specific measures are taken to maintain it, while the productivity of natural fisheries is also sharply limited. The area of arable land will decrease due to soil erosion from over-grazing; laterization of clearfelled areas; soil salinization and other types of land degradation; and the expansion of urban, industrial and other developments.
Water availability and quality, already totally inadequate in much of the world, will remain major problems for rural areas of developing countries and also for many urban populations, who may face the additional problem of high utilization charges. Needs for water will increase greatly, and for several large cities the meeting of water demands will become increasingly costly as supplies will have to be brought from far away. Re-use of water implies more stringent standards for treatment. The increasing production of wastewater and sewage will require more extensive treatment facilities, as well as large outlays of capital.
The continuing long-term need for industrial development to produce goods, services and employment will lead to more intensive food production, which will itself become more industrialized. Consequently, and especially because of urbanization, the demand for, and the resources employed in, packaging, processing, storage and distribution of food will increase in volume and importance.
The public is becoming much more aware of the need to produce, protect and market food in ways which minimize adverse change in our environment, and is more demanding in this respect. The emergence of revolutionary scientific tools (e.g., biotechnological advances) offers the possibility of significantly increasing food production, reducing waste and enhancing safety.
The principal challenge is to meet the increasing demands for food, other agricultural products and water in ways that foster long-term improvements in health, and which are also sustainable, economical and competitive.
Despite the fact that globally there is at present sufficient food for all, great difficulties have to be overcome to ensure the availability and equitable distribution of safe, nutritious and affordable food supplies to meet health needs in many parts of the world, and notably in areas of rapid population growth.
There is often a failure to take the possible health consequences fully into account in the design and implementation of agricultural and fisheries policies and programmes. An example is the production of tobacco, which has very serious and negative impacts on human health and on scarce land and fuelwood resources. Moreover, the lack of an integrated approach to development of the agriculture and forestry sectors results in failure to recognize the important relationship of both sectors to the protection of wildlife habitats, biological diversity and genetic resources.
If timely and appropriate action is not taken to mitigate the environmental impacts of agriculture, fisheries, food production and water use, then the following situations will prevail:
- As the urban population increases, the difficulty of maintaining and extending an efficient food distribution system will become greater. This may increase the prevalence of household food insecurity, associated malnutrition and health risks among the growing masses of urban poor.
- Microbial, viral and parasitic diseases from contaminated food and water will continue to be serious health problems. New agents of public health importance will continue to emerge. The diarrhoeal diseases related to food and water, causing high infant mortality and universal morbidity, will increase.
- Vector-borne diseases from irrigation, other water resource developments, and uncontrolled wastewater will increase substantially. Malaria, schistosomiasis, filariasis and arbovirus fevers will continue to be major problems.
- The problems outlined above will be reflected in static or rising levels of infant and young child malnutrition and mortality, as well as morbidity at all ages, but predominantly among the poor, the very young, the aged and the sick.
- diseases linked to inappropriate life-styles, smoking and diet (for example, obesity, diabetes or coronary heart disease), which are characteristic of the more affluent countries, are now emerging and becoming significant problems also in developing countries. The increasing urbanization will accelerate this trend.
- As the intensity of food production increases, the risk of occupational diseases and accidents among those working in this and related sectors will increase substantially unless sufficient efforts for safety and prevention are made.
Health Consequences of Biological Contamination and Chemicals in Food
Despite progress in science and technology, contaminated food and water remain to this day major public health problems. Foodborne diseases are perhaps the most widespread health problems in the contemporary world and important causes of reduced economic productivity (WHO/FAO 1984). They are caused by a wide range of agents, and cover all degrees of severity, from mild indispositions to life-threatening illnesses. However, only a small proportion of cases comes to the notice of health services and even fewer are investigated. As a result, it is believed that in industrialized countries only approximately 10% of the cases are reported, whilst in developing countries reported cases probably account for not more than 1% of the total.
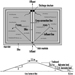
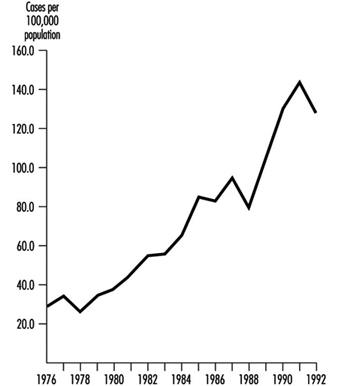
Despite these limitations, the data that are available indicate that foodborne diseases are increasing all over the world, both in developing and industrialized countries. Experience in Venezuela illustrates this trend (PAHO/WHO 1989) (figure 1).
Figure 1. Foodborne diseases in Venezuela
Developing countries
Available information clearly indicates that biological contaminants (bacteria, viruses and parasites) are the major causes of foodborne diseases (table 1).
Table 1. Some agents of important foodborne diseases and salient epidemiological features
|
Agents |
Important reservoir/carrier |
Transmissiona by |
Multiplication |
Examples of some incriminated foods |
||
|
Water |
Food |
Person to person |
||||
|
Bacteria |
||||||
|
Baccillus cereus |
Soil |
- |
+ |
- |
+ |
Cooked rice, cooked meats, vegetables, |
|
Brucella species |
Cattle, goats, sheep |
- |
+ |
- |
+ |
Raw milk, dairy products |
|
Campylobacter jejuni |
Chickens, dogs, cats, cattle, |
+ |
+ |
+ |
-b |
Raw milk, poultry |
|
Clostridium botulinum |
Soil, mammals, birds, fish |
- |
+ |
- |
+ |
Fish, meat, vegetables (home preserved), |
|
Clostridium perfringens |
Soil, animals, humans |
- |
+ |
- |
+ |
Cooked meat and poultry, gravy, beans |
|
Escherichia coli |
||||||
|
Enterotoxigenic |
Humans |
+ |
+ |
+ |
+ |
Salad, raw vegetables |
|
Enteropathogenic |
Humans |
+ |
+ |
+ |
+ |
Milk |
|
Enteroinvasive |
Humans |
+ |
+ |
0 |
+ |
Cheese |
|
Enterohaemorrhagic |
Cattle, poultry, sheep |
+ |
+ |
+ |
+ |
Undercooked meat, raw milk, cheese |
|
Listeria monocytogenes |
Environment |
+ |
+ |
-c |
+ |
Cheese, raw milk, coleslaw |
|
Mycobacterium bovis |
Cattle |
- |
+ |
- |
- |
Raw milk |
|
Salmonella typhi and |
Humans |
+ |
+ |
± |
+ |
Dairy products, meat products, shellfish, |
|
Salmonella (non-typhi) |
Humans and animals |
± |
+ |
± |
+ |
Meat, poultry, eggs, dairy products, |
|
Shigella spp. |
Humans |
+ |
+ |
+ |
+ |
Potato/egg salads |
|
Staphylococcus aureus |
- |
+ |
- |
+ |
Ham, poultry and egg salads, cream-filled |
|
|
Vibrio cholerae, 01 |
Humans, marine life |
+ |
+ |
± |
+ |
Salad, shellfish |
|
Vibrio cholerae, non-01 |
Humans, marine life |
+ |
+ |
± |
+ |
Shellfish |
|
Vibrio parahaemolyticus |
Sea water, marine life |
- |
+ |
- |
+ |
Raw fish, crabs, and other shellfish |
|
Vibrio vulnificus |
Sea water, marine life |
+ |
+ |
- |
+ |
Shellfish |
|
Yersinia enterocolitica |
Water, wild animals, pigs, |
+ |
+ |
- |
+ |
Milk, pork, and poultry |
|
Viruses |
||||||
|
Hepatitis A virus |
Humans |
+ |
+ |
+ |
- |
Shellfish, raw fruit and vegetables |
|
Norwalk agents |
Humans |
+ |
+ |
- |
- |
Shellfish, salad |
|
Rotavirus |
Humans |
+ |
+ |
+ |
- |
0 |
|
Protozoa |
+ |
+ |
+ |
+ |
||
|
Cryptosporidium parvum |
Humans, animals |
+ |
+ |
+ |
- |
Raw milk, raw sausage (non-fermented) |
|
Entamoeba histolytica |
Humans |
+ |
+ |
+ |
- |
Vegetables and fruits |
|
Giardia lamblia |
Humans, animals |
+ |
± |
+ |
- |
Vegetables and fruits |
|
Toxoplasma gondii |
Cats, pigs |
0 |
+ |
- |
- |
Undercooked meat, raw vegetables |
|
Helminths |
||||||
|
Ascaris lumbricoides |
Humans |
+ |
+ |
- |
- |
Soil-contaminated food |
|
Clonorchis sinensis |
Freshwater fish |
- |
+ |
- |
- |
Undercooked/raw fish |
|
Fasciola hepatica |
Cattle, goats |
+ |
+ |
- |
- |
Watercress |
|
Opisthorclis viverrini/felinus |
Freshwater fish |
- |
+ |
- |
- |
Undercooked/raw fish |
|
Paragonimus sp. |
Freshwater crabs |
- |
+ |
- |
- |
Undercooked/raw crabs |
|
Taenia saginata and T. solium |
Cattle, swine |
- |
+ |
- |
- |
Undercooked meat |
|
Trichinella spiralis |
Swine, carnivora |
- |
+ |
- |
- |
Undercooked meat |
|
Trichuris trichiura |
Humans |
0 |
+ |
- |
- |
Soil-contaminated food |
a Almost all acute enteric infections show increased transmission during the summer and/or wet months, except infections due to Rotavirus and Yersinia enterocolitica, which show increased transmission in cooler months.
b Under certain circumstances, some multiplication has been observed. The epidemiological significance of this observation is not clear.
c Vertical transmission from pregnant woman to foetus occurs frequently.
+ = Yes; ± = Rare; - = No; 0 = No information.
Adapted from WHO/FAO 1984.
In the developing countries, they are responsible for a wide range of foodborne diseases (e.g., cholera, salmonellosis, shigellosis, typhoid and paratyphoid fevers, brucellosis, poliomyelitis and amoebiasis). Diarrhoeal diseases, especially infant diarrhoea, are the dominant problem and indeed one of massive proportions. Annually, some 1,500 million children under the age of five suffer from diarrhoea and of these over three million die as a result. Formerly it was thought that contaminated water supplies were the main direct source of pathogens causing diarrhoea, but now it has been shown that up to 70% of diarrhoeal episodes may be due to foodborne pathogens (WHO 1990c). However, the contamination of the food may in many cases originate from contaminated water that is used for irrigation and similar purposes.
Industrialized countries
Although the situation regarding foodborne diseases is very serious in developing countries, the problem is not limited to these countries, and in recent years, industrialized countries have experienced a succession of major epidemics. In the United States it is estimated there are 6.5 million cases per year, with 9,000 fatalities, but according to the US Food and Drug Administration this figure is an underestimate and may be as high as 80 million cases (Cohen 1987; Archer and Kvenberg 1985; Young 1987). The estimate for former West Germany was one million cases in 1989 (Grossklaus 1990). A study in the Netherlands found that as many as 10% of the population may be affected by foodborne or waterborne diseases (Hoogenboom-Vergedaal et al. 1990).
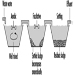
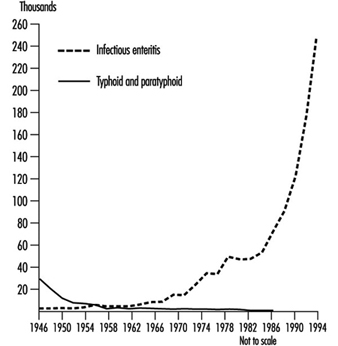
With today’s improvements in standards of personal hygiene, development of basic sanitation, safe water supplies, effective infrastructure and the increasing application of technologies such as pasteurization, many foodborne diseases have been either eliminated or considerably reduced in certain industrialized countries (e.g., milkborne salmonellosis). Nevertheless, most countries are now experiencing an important increase in several other foodborne diseases. The situation in former West Germany (1946-1991) illustrates this phenomenon (figure 2) (Statistisches Bundesamt 1994).
Figure 2. Infectious enteritis, typhoid fever and para-typhoid fever (A, B and C), Germany
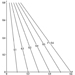
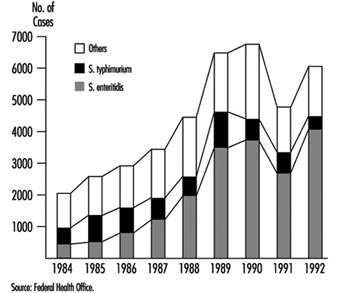
Salmonellosis, specifically, has increased tremendously on both sides of the Atlantic over the past few years (Rodrigue 1990). In many cases it is due to Salmonella enteritidis. Figure 3 shows the increase of this micro-organism in relation to other Salmonella strains in Switzerland. In many countries, poultry meat, eggs and foods containing eggs have been identified as the predominant sources of this pathogen. In certain countries, 60 to 100% of poultry meat is contaminated with Salmonella spp., and meat, frogs’ legs, chocolate and milk have also been implicated (Notermans 1984; Roberts 1990). In 1985, some 170,000 to 200,000 persons were involved in an outbreak of salmonellosis in Chicago which was caused by contaminated pasteurized milk (Ryzan 1987).
Figure 3. Serotypes of Salmonella in Switzerland
Chemicals and toxicants in food
Considerable efforts have been undertaken at the national and international levels to ensure the chemical safety of food supplies. Two joint FAO/WHO committees have, over a period of three decades, evaluated a large number of food chemicals. The Joint FAO/WHO Expert Committee on Food Additives (JECFA) evaluates food additives, contaminants and veterinary drug residues, and the Joint FAO/WHO Meeting on Pesticide Residues (JMPR) evaluates pesticide residues. Recommendations are made on the acceptable daily intake (ADI), on maximum residue levels (MRLs) and maximum levels (MLs). Based on these recommendations, the Codex Alimentarius Commission and governments establish food standards and safe levels for these substances in foodstuffs. Moreover, the Joint UNEP/FAO/WHO Food Contamination Monitoring Programme (GEMS/Food) provides information on the levels of contaminants in food and on time trends of contamination, enabling preventive and control measures.
While information from most of the developing countries is scarce, surveys made in the industrialized countries suggest that the food supply is largely safe from the chemical viewpoint owing to the extensive food safety infrastructure (i.e., legislation, enforcement mechanisms, surveillance and monitoring systems) and the general level of responsibility of the food industry. However, accidental contamination or adulteration does occur, in which case the health consequences may be grave. For example, in Spain in 1981-82, adulterated cooking oil killed some 600 people and disabled—temporarily or permanently—another 20,000 (WHO 1984). The agent responsible for this mass poisoning has not yet been identified in spite of intensive investigations.
Environmental chemicals
A number of chemical substances may occur in the food supply as a result of environmental contamination. Their effects on health may be extremely serious and have caused great concern in recent years.
Serious consequences have been reported when foods contaminated with heavy metals such as lead, cadmium or mercury have been ingested over extended periods of time.
The Chernobyl accident provoked great concern over the health risks to people exposed to accidental radionuclide emissions. People living in the vicinity of the accident were exposed, and this exposure included radioactive contaminants in food and water. In other parts of Europe and elsewhere, at some distance from the accident, this concern focused on contaminated foods as a source of exposure. In most countries, the estimated average dose acquired from eating contaminated foods amounted to only a very small fraction of the dose normally received from background radiation (IAEA 1991).
Other environmental chemicals of interest are polychlorinated biphenyls (PCBs). PCBs are used in various industrial applications. Information on the effects of PCBs on human health were originally noted following from two large-scale incidents which occurred in Japan (1968) and in Taiwan, China (1979). Experience from these outbreaks showed that as well as their acute effects, PCBs may also have carcinogenic effects.
DDT was widely used between 1940 and 1960 as an insecticide for agricultural purposes and for the control of vector-borne diseases. It is now banned or restricted in many countries because of its potential risk to the environment. In many tropical countries, DDT is still an important chemical, used for the control of malaria. No confirmed ill effects have been reported due to residues of DDT in food (UNEP 1988).
Mycotoxins
Mycotoxins, the toxic metabolites of certain microscopic fungi (moulds), may cause serious adverse effects in humans, as well as in animals. Animal studies have shown that besides acute intoxication, mycotoxins are capable of causing carcinogenic, mutagenic and teratogenic effects.
Biotoxins
Intoxication by marine biotoxin (also known as “fish poisoning”) is another problem of concern. Examples of such intoxications are ciguatera and various kinds of shellfish poisoning.
Plant toxicants
Toxicants in edible plants and poisonous plants which resemble them (mushrooms, certain wild green plants) are important causes of ill health in many areas of the world and present a troublesome problem for food safety (WHO 1990b).
Industrial Pollution in Developing Countries
While industrialization is an essential feature of economic growth in developing countries, industrial practices may also produce adverse environmental health consequences through the release of air and water pollutants and the disposal of hazardous wastes. This is often the case in developing countries, where less attention is paid to environmental protection, environmental standards are often inappropriate or not effectively implemented, and pollution control techniques are not yet fully developed. With rapid economic development, many developing countries, like China and other Asian countries, face some additional environmental problems. One is the environmental pollution from hazardous industries or technologies transferred from developed countries, which are no longer acceptable for occupational and environmental health reasons in developed countries, but still allowable in developing countries due to looser environmental legislation. Another problem is the rapid proliferation of informal small-scale enterprises in townships as well as in rural areas, which often create serious air and water pollution because of lack of sufficient knowledge and funds.
Air Pollution
Air pollution in developing countries is derived not only from stack emission of pollutants from relatively large industries, like iron and steel, non-ferrous metals and petroleum products industries, but also from fugitive emission of pollutants from small-scale factories, such as cement mills, lead refineries, chemical fertilizer and pesticide factories and so on, where inadequate pollution control measures exist and pollutants are allowed to escape to the atmosphere.
Since industrial activities always involve energy generation, the combustion of fossil fuels is a main source of air pollution in the developing countries, where coal is widely used not only for industrial, but also for domestic consumption. For instance, in China, more than 70% of total energy consumption relies on direct coal combustion, from which large amounts of pollutants (suspended particulates, sulphur dioxide, etc.) are emitted under incomplete combustion and inadequate emission controls.
The kinds of air pollutants emitted vary from industry to industry. The concentrations of different pollutants in the atmosphere also vary widely from process to process, and from place to place with different geographic and climatic conditions. It is difficult to estimate specific exposure levels of various pollutants from different industries to the general population in developing countries, as elsewhere. In general, the workplace exposure levels are much higher than that of the general population, because the emissions are rapidly diluted and dispersed by the wind. But the exposure duration of the general population is much longer than that of workers.
The exposure levels of the general population in developing countries are usually higher than that in developed countries, where air pollution is more strictly controlled and resident areas are usually far from industries. As discussed further on in this chapter, a large number of epidemiological studies have already showed the close association of reduction in pulmonary function and increased incidence of chronic respiratory diseases among residents with long-term exposure to the common air pollutants.
A case study of air pollution effects on the health of 480 primary school children in Cubatao, Brazil, where large quantities of mixed pollutants were emitted from 23 industries (steel mill, chemical industries, cement factory, fertilizer plants, etc.), showed that 55.3% of the children had decreases in pulmonary function. Another example of health effects of air pollution appeared in the Ulsan/Onsan special industrial zone, Republic of Korea, where many large-scale plants (mainly petrochemical plants and metal refineries) are concentrated. Local residents complained of a variety of health problems, particularly of the nervous system disorder called “Onsan Disease”.
Accidental releases of toxic substances into the atmosphere resulting in serious health risks are usually more common in developing countries. The reasons include inadequate safety planning, lack of skilled technical personnel to maintain proper facilities, and difficulties in obtaining spare parts and so on. One of the worst of such accidents occurred in Bhopal, India, in 1984, where leaking methyl isocyanide killed 2,000 people.
Water and Soil Pollution
Inappropriate and often careless disposal of industrial wastes—uncontrolled discharge into watercourses and uncontrolled disposal on the land, which often causes water and soil pollution—is another crucial environmental health problem, in addition to industrial air pollution, in developing countries, particularly with numerous small-scale township enterprises, like those in China. Some small-scale factories, such as textile dyeing, pulp and paper, leather tanning, electroplating, fluorescent lamp, lead battery and metal smelting, always produce a large amount of wastes, containing toxic or hazardous substances like chromium, mercury, lead, cyanide and so on, which may pollute the rivers, streams and lakes, and soil as well, when they are untreated. The soil pollution in turn may contaminate groundwater resources.
In Karachi, the Lyan river, which runs through the city, has become an open drain of sewage and untreated industrial effluent from some 300 large and small industries. There is a similar case in Shanghai. Some 3.4 million cubic metres of industrial and domestic waste pour into Suzhou creek and Huangpu river, which flow through the heart of the city. Because of serious pollution, the river and creek have essentially become devoid of life and often produce smells and sights that are unpleasant and offensive to the public living in the surrounding area.
A further problem of water and soil pollution in developing countries is the transfer of toxic or hazardous wastes from developed to developing countries. The cost of transporting these wastes to simple storage sites in developing countries is a mere fraction of the cost required for safely storing or incinerating them in their countries of origin in compliance with the applicable government regulations there. This has occurred in Thailand, Nigeria, Guinea-Bissau and so on. The toxic wastes inside the barrels can leak and pollute the air, water and soil, posing a potential health risk to the people living in the vicinity.
Thus the environmental health problems discussed in this chapter tend to apply to an even greater extent to developing countries.
Developing Countries and Pollution
Industrial pollution is a more complicated problem in developing countries than in developed economies. There are greater structural obstacles to preventing and cleaning up pollution. These obstacles are largely economic, because developing countries do not have the resources to control pollution to the extent that developed countries can. On the other hand, the effects of pollution may be very costly to a developing society, in terms of health, waste, environmental degradation, reduced quality of life and clean-up costs in the future. An extreme example is concern for the future of children exposed to lead in some megacities in countries where leaded gasoline is still used, or in the vicinity of smelters. Some of these children have been found to have blood lead levels high enough to impair intelligence and cognition.
Industry in developing countries usually operates short of capital compared to industry in developed countries, and those investment funds that are available are first put into the equipment and resources necessary for production. Capital that is applied toward control of pollution is considered “unproductive” by economists because such investment does not lead to increased production and financial return. However, the reality is more complicated. Investment in control of pollution may not bring an obvious direct return on investment to the company or industry, but that does not mean that there is no return on investment. In many cases, as in an oil refinery, control of pollution also reduces the amount of wastage and increases the efficiency of the operation so that the company does benefit directly. Where public opinion carries weight and it is to the advantage of a company to maintain good public relations, industry may make an effort to control pollution in its own interest. Unfortunately, the social structure in many developing countries does not favour this because the people most negatively affected by pollution tend to be those who are impoverished and marginalized in society.
Pollution may damage the environment and society as a whole, but these are “externalized dis-economies” that do not substantially hurt the company itself, at least not economically. Instead, the costs of pollution tend to be carried by society as a whole, and the company is spared the costs. This is particularly true in situations where the industry is critical to the local economy or national priorities, and there is a high tolerance for the damage it causes. One solution would be to “internalize” the external dis-economies by incorporating the costs of clean-up or the estimated costs of environmental damage into the operating costs of the company as a tax. This would give the company a financial incentive to control its costs by reducing its pollution. Virtually no government in any developing country is in a position to do this and to enforce the tax, however.
In practice, capital is rarely available to invest in equipment to control pollution unless there is pressure from government regulation. However, governments are rarely motivated to regulate industry unless there are compelling reasons to do so, and pressure from their citizens. In most developed countries, people are reasonably secure in their health and their lives, and expect a higher quality of life, which they associate with a cleaner environment. Because there is more economic security, these citizens are more willing to accept an apparent economic sacrifice in order to achieve a cleaner environment. However, in order to be competitive in world markets, many developing countries are very reluctant to impose regulation on their industries. Instead, they hope that industrial growth today will lead to a society rich enough tomorrow to clean up the pollution. Unfortunately, the cost of clean-up increases as fast as, or faster than, the costs associated with industrial development. At an early stage of industrial development, a developing country would in theory have very low costs associated with the prevention of pollution, but hardly ever do such countries have the capital resources they need to do so. Later, when such a country does have the resources, the costs are often staggeringly high and the damage has already been done.
Industry in developing countries tends to be less efficient than in developed countries. This lack of efficiency is a chronic problem in developing economies, reflecting untrained human resources, the cost of importing equipment and technology, and the inevitable wastage that occurs when some parts of the economy are more developed than others.
This inefficiency is also based in part on the need to rely on outdated technologies which are freely available, do not require an expensive licence or that do not cost as much to use. These technologies are often more polluting than the state-of-the-art technologies available to industry in developed countries. An example is the refrigeration industry, where the use of chlorofluorocarbons (CFCs) as refrigerant chemicals is much cheaper than the alternatives, despite the serious effects of these chemicals in depleting ozone from the upper atmosphere and thereby reducing the earth’s shield from ultraviolet radiation; some countries had been very reluctant to agree to prohibit the use of CFCs because it would then be economically impossible for them to manufacture and purchase refrigerators. Technology transfer is the obvious solution, but companies in developed countries who developed or hold the licence for such technologies are understandably reluctant to share them. They are reluctant because they spent their own resources developing the technology, wish to retain the advantage they have in their own markets by controlling such technology, and may make their money from using or selling the technology only during the limited term of the patent.
Another problem faced by developing countries is lack of expertise in and awareness of the effects of pollution, monitoring methods and the technology of pollution control. There are relatively few experts in the field in developing countries, in part because there are fewer jobs and a smaller market for their services even though the need may actually be greater. Because the market for pollution control equipment and services may be small, this expertise and technology may have to be imported, adding to the costs. General recognition of the problem by managers and supervisors in industry may be lacking or very low. Even when an engineer, manager or supervisor in industry realizes that an operation is polluting, it may be difficult to persuade others in the company, their bosses or the owners that there is a problem that must be solved.
Industry in most developing countries competes at the low end of international markets, meaning that it produces products that are competitive on the basis of price and not quality or special features. Few developing countries specialize in making very fine grades of steel for surgical instruments and sophisticated machinery, for example. They manufacture lesser grades of steel for construction and manufacturing because the market is much larger, the technical expertise required to produce it is less, and they can compete on the basis of price as long as the quality is good enough to be acceptable. Pollution control reduces the price advantage by increasing the apparent costs of production without increasing output or sales. The central problem in developing countries is how to balance this economic reality against the need to protect their citizens, the integrity of their environment, and their future, realizing that after development the costs will be even higher and the damage may be permanent.
Air Pollution
The problem of air pollution has grown steadily since the Industrial Revolution began 300 years ago. Four major factors have exacerbated air pollution: growing industrialization; increasing traffic; rapid economic development; and higher levels of energy consumption. The available information shows that the WHO guidelines for the major air pollutants are regularly exceeded in many major urban centres. Although progress has been made in controlling air pollution problems in many industrialized countries over the last two decades, air quality—particularly in the larger cities in the developing world—is worsening. Of major concern are the adverse health effects of ambient air pollutants in many urban areas, where levels are sufficiently high to contribute to increased mortality and morbidity, deficits in pulmonary function and cardiovascular and neurobehavioural effects (Romieu, Weizenfeld and Finkelman 1990; WHO/UNEP 1992). Indoor air pollution due to domestic combustion products is also a major issue in developing countries (WHO 1992b), but it is not part of this review, which considers only the sources, dispersion and health effects of outdoor air pollution, and includes a case study of the situation in Mexico.
Source of Air Pollutants
The most common air pollutants in urban environments include sulphur dioxide (SO2), suspended particulate matter (SPM), the nitrogen oxides (NO and NO2, collectively termed NOX), ozone (O3), carbon monoxide (CO) and lead (Pb). Combustion of fossil fuels in stationary sources leads to the production of SO2, NOX and particulates, including sulphate and nitrate aerosols formed in the atmosphere following gas to particle conversion. Petrol-fuelled motor vehicles are the principal sources of NOX, CO and Pb, whereas diesel-fuelled engines emit significant quantities of particulates, SO2 and NOX. Ozone, a photochemical oxidant and the main constituent of photochemical smog, is not emitted directly from combustion sources but is formed in the lower atmosphere from NOX and volatile organic compounds (VOCs) in the presence of sunlight (UNEP 1991b). Table 1 presents the major sources of outdoor air pollutants.
Table 1. Major sources of outdoor air pollutants
Pollutants Sources
Sulphur oxides Coal and oil combustion, smelters
Suspended particulate matter Combustion products (fuel, biomass), tobacco smoke
Nitrogen oxides Fuel and gas combustion
Carbon monoxide Incomplete petrol and gas combustion
Ozone Photochemical reaction
Lead Petrol combustion, coal combustion, producing batteries, cables, solder, paint
Organic substances Petrochemical solvents, vaporization of unburnt fuels
Source: Adapted from UNEP 1991b.
Dispersion and Transport of Air Pollutants
The two major influences on the dispersion and transport of air pollutant emissions are the meteorology (including microclimate effects such as “heat islands”) and the topography in relation to the population distribution. Many cities are surrounded by hills which may act as a downwind barrier, trapping pollution. Thermal inversions contribute to a particulate problem in temperate and cold climates. Under normal dispersion conditions, hot pollutant gases rise as they come into contact with colder air masses with increasing altitude. However, under certain circumstances the temperature may increase with altitude, and an inversion layer forms, trapping pollutants close to the emission source and delaying their diffusion. Long-range transport of air pollution from large urban areas may have national and regional impacts. Oxides of nitrogen and sulphur may contribute to acid deposition at great distances from the emission source. Ozone concentrations are often elevated downwind of urban areas due to the time lag involved in photochemical processes (UNEP 1991b).
Health Effects of Air Pollutants
Pollutants and their derivatives can cause adverse effects by interacting with and impairing molecules crucial to the biochemical or physiological processes of the human body. Three factors influence the risk of toxic injury related to these substances: their chemical and physical properties, the dose of the material that reaches the critical tissue sites and the responsiveness of these sites to the substance. The adverse health effects of air pollutants may also vary across population groups; in particular, the young and the elderly may be especially susceptible to deleterious effects. Persons with asthma or other pre-existing respiratory or cardiac diseases may experience aggravated symptoms upon exposure (WHO 1987).
Sulphur Dioxide and Particulate Matter
During the first half of the twentieth century, episodes of marked air stagnation resulted in excess mortality in areas where fossil-fuel combustion produced very high levels of SO2 and SMP. Studies of long-term health effects have also related the annual mean concentrations of SO2 and SMP to mortality and morbidity. Recent epidemiological studies have suggested an adverse effect of inhalable particulate levels (PM10) at relatively low concentrations (not exceeding the standard guidelines) and have shown a dose-response relationship between exposure to PM10 and respiratory mortality and morbidity (Dockery and Pope 1994; Pope, Bates and Razienne 1995; Bascom et al. 1996) as shown in table 2.
Table 2. Summary of short-term exposure-response relationship of PM10 with different health effects indicators
|
Health effect |
% changes for each 10 μg/m3 |
|
|
Mean |
Range |
|
|
Mortality |
||
|
Total |
1.0 |
0.5-1.5 |
|
Cardiovascular |
1.4 |
0.8-1.8 |
|
Respiratory |
3.4 |
1.5-3.7 |
|
Morbidity |
||
|
Hospital admission for respiratory condition |
1.1 |
0.8-3.4 |
|
Emergency visits for respiratory conditions |
1.0 |
0.5-4 |
|
Symptom exacerbations among asthmatics |
3.0 |
1.1-11.5 |
|
Changes in peak expiratory flow |
0.08 |
0.04-0.25 |
Nitrogen Oxides
Some epidemiological studies have reported adverse health effects of NO2 including increased incidence and severity of respiratory infections and increase in respiratory symptoms, especially with long-term exposure. Worsening of the clinical status of persons with asthma, chronic obstructive pulmonary disease and other chronic respiratory conditions has also been described. However, in other studies, investigators have not observed adverse effects of NO2 on respiratory functions (WHO/ECOTOX 1992; Bascom et al. 1996).
Photochemical Oxidants and Ozone
The health effects of photochemical oxidants exposure cannot be attributed only to oxidants, because photochemical smog typically consists of O3, NO2, acid and sulphate and other reactive agents. These pollutants may have additive or synergistic effects on human health, but O3 appears to be the most biologically active. Health effects of ozone exposure include decreased pulmonary function (including increased airway resistance, reduced air flow, decreased lung volume) due to airway constriction, respiratory symptoms (cough, wheezing, shortness of breath, chest pains), eye, nose and throat irritation, and disruption of activities (such as athletic performance) due to less oxygen availability (WHO/ECOTOX 1992). Table 3 summarizes the major acute health effects of ozone (WHO 1990a, 1995). Epidemiological studies have suggested a dose-response relationship between exposure to increasing ozone levels and the severity of respiratory symptoms and the decrement in respiratory functions (Bascom et al. 1996).
Table 3. Health outcomes associated with changes in peak daily ambient ozone concentration in epidemiological studies
|
Health outcome |
Changes in |
Changes in |
|
Symptom exacerbations among healthy children |
||
|
25% increase |
200 |
100 |
|
50% increase |
400 |
200 |
|
100% increase |
800 |
300 |
|
Hospital admissions for respiratory |
||
|
5% |
30 |
25 |
|
10% |
60 |
50 |
|
20% |
120 |
100 |
a Given the high degree of correlation between the 1-h and 8-h O3 concentrations in field studies, an improvement in health risk associated with decreasing 1- or 8-h O3 levels should be almost identical.
Source: WHO 1995.
Carbon Monoxide
The main effect of CO is to decrease oxygen transport to the tissues through the formation of carboxyhaemoglobin (COHb). With increasing levels of COHb in blood, the following health effects can be observed: cardiovascular effects in subjects with previous angina pectoris (3 to 5%); impairment of vigilance tasks (>5%); headache and dizziness (≥10%); fibrinolysis and death (WHO 1987).
Lead
Lead exposure principally affects haem biosynthesis, but also may act on the nervous system and other systems such as the cardiovascular system (blood pressure). Infants and young children less than five years old are particularly sensitive to lead exposure because of its effect on neurological development at blood lead levels close to 10 μg/dl (CDC 1991).
Several epidemiological studies have investigated the effect of air pollution, especially ozone exposure, on the health of the population of Mexico City. Ecological studies have shown an increase in mortality with respect to exposure to fine particulates (Borja-Arburto et al. 1995) and an increase in emergency visits for asthma among children (Romieu et al. 1994). Studies of the adverse effect of ozone exposure conducted among healthy children have shown an increase in school absenteeism due to respiratory illnesses (Romieu et al. 1992), and a decrease in lung function after both acute and subacute exposure (Castillejos et al. 1992, 1995). Studies conducted among asthmatic children have shown an increase in respiratory symptoms and a decrease in peak expiratory flow rate after exposure to ozone (Romieu et al. 1994) and to fine particulate levels (Romieu et al. in press). Although, it seems clear that acute exposure to ozone and particulates is associated with adverse health effects in the population of Mexico City, there is a need to evaluate the chronic effect of such exposure, in particular given the high levels of photo-oxidants observed in Mexico City and the ineffectiveness of control measures.
Case study: Air pollution in Mexico City
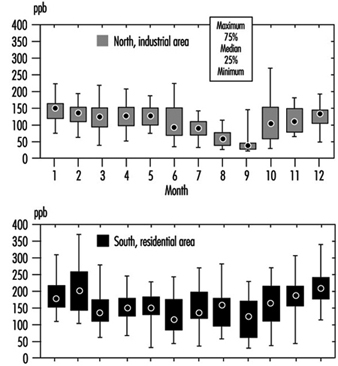
The metropolitan area of Mexico City (MAMC) is situated in the Mexican Basin at a mean altitude of 2,240 metres. The basin covers 2,500 square kilometres and is surrounded by mountains, two of which are over 5,000 metres high. The total population was estimated at 17 million in 1990. Due to the particular geographic characteristics and the light winds, ventilation is poor with a high frequency of thermic inversions, especially during the winter. More than 30,000 industries in the MAMC and the three million motor vehicles circulating daily are responsible for 44% of the total energy consumption. Since 1986, air pollution has been monitored, including SO2, NOx, CO, O3, particulate matter and non-methane hydrocarbon (HCNM). The main air pollutant problems are related to ozone, especially in the southwest part of the city (Romieu et al. 1991). In 1992 the Mexican norm for ozone (110 ppb one-hour maximum) was exceeded in the southwest part more than 1,000 hours and reached a maximum of 400 ppb. Particulate levels are high in the northeast section of the city, close to the industrial park. In 1992, the annual average of inhalable particulate (PM10) was 140 μg/m3. Since 1990, important control measures have been taken by the government to decrease air pollution, including a programme that prohibits use of cars one day a week depending on their terminating licence plate number, the closure of one of the most polluting refineries located in Mexico City, and the introduction of unleaded fuel. These measures have led to a decrease in various air pollutants, mainly SO2, particulate matter, NO2, CO and lead. However the ozone level remains a major problem (see figure 1, figure 2 and figure 3).
Figure 1. Ozone levels in two zones of Mexico City. One-hour daily maximum by month, 1994
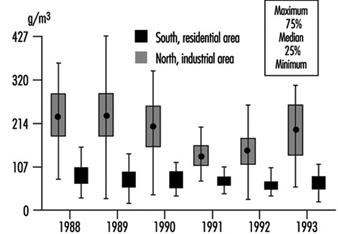
Figure 2. Particulates (PM10) in two zones of Mexico City, 1988-1993
Figure 3. Air lead levels in two zones of Mexico City, 1988-1994
Land Pollution
The amount of waste produced by human society is increasing. Commercial and domestic solid waste is a great practical problem for many local governments. Industrial wastes are usually much smaller in volume but are more likely to contain hazardous materials, such as toxic chemicals, flammable liquids and asbestos. Although the total amount is less, the disposal of hazardous industrial waste has been a greater concern than of domestic waste because of the perceived hazard to health and the risk of environmental contamination.
The generation of hazardous waste has become a major problem worldwide. The root cause of the problem is industrial production and distribution. Land pollution occurs when hazardous wastes contaminate soil and groundwater due to inadequate or irresponsible disposal measures. Abandoned or neglected waste disposal sites are a particularly difficult and expensive problem for society. Sometimes, hazardous waste is disposed of illegally and in an even more dangerous manner because the owner cannot find a cheap way to get rid of it. One of the major unresolved issues in managing hazardous waste is to find methods of disposal that are both safe and inexpensive. Public concern over hazardous waste focuses on the potential health effects of exposure to toxic chemicals, and particularly the risk of cancer.
The Basel Convention passed in 1989 is an international agreement to control the transboundary movement of hazardous waste and to prevent dangerous wastes from being shipped for disposal to countries that do not have the facilities to process them safely. The Basel Convention requires that the generation of hazardous wastes and transboundary movement of the wastes be kept to a minimum. Traffic in hazardous wastes is subject to the informed permission and laws of the receiving country. Transboundary movement of hazardous wastes is subject to good environmental practices and assurance that the receiving country is able to handle them safely. All other traffic in hazardous wastes is considered illegal and therefore criminal in intent, subject to national laws and penalties. This international convention provides an essential framework for controlling the problem at an international level.
Hazardous Properties of Chemicals
Hazardous substances are compounds and mixtures that pose a threat to health and property because of their toxicity, flammability, explosive potential, radiation or other dangerous properties. Public attention tends to focus on carcinogens, industrial wastes, pesticides and radiation hazards. However, innumerable compounds that do not fall into these categories can pose a threat to the public’s safety and health.
Hazardous chemicals may present physical hazards, although this is more common in transportation and industrial incidents. Hydrocarbons may catch fire and even explode. Fires and explosions may generate their own toxic hazards depending on the chemicals that were initially present. Fires involving pesticide storage areas are a particularly dangerous situation, as the pesticides may be converted into even more highly toxic combustion products (such as paraoxons in the case of organophosphates) and substantial amounts of environmentally damaging dioxins and furans may be generated from combustion in the presence of chlorine compounds.
Toxicity, however, is the principal concern of most people with respect to hazardous waste. Chemicals may be toxic to human beings and they may also be damaging to the environment through toxicity to animal and plant species. Those that do not readily degrade in the environment (a characteristic called biopersistence) or that accumulate in the environment (a characteristic called bioaccumulation) are of particular concern.
The number and hazardous nature of toxic substances in common use has changed dramatically. In the last generation, research and development in organic chemistry and chemical engineering have introduced thousands of new compounds into widespread commercial use, including persistent compounds such as the polychlorinated biphenyls (PCBs), more potent pesticides, accelerators and plasticizers with unusual and poorly understood effects. The production of chemicals has risen dramatically. In 1941 production of all synthetic organic compounds in the United States alone, for example, was less than one billion kilograms. Today it is much greater than 80 billion kilograms. Many compounds in common use today underwent little testing and are not well understood.
Toxic chemicals are also much more intrusive in daily life than in the past. Many chemical plants or disposal sites which were once isolated or on the edge of town have become incorporated into urban areas by suburban growth. Communities now lie in closer proximity to the problem than they have in the past. Some communities are built directly over old disposal sites. Although incidents involving hazardous substances take many forms and may be highly individual, the great majority seem to involve a relatively narrow range of hazardous substances, which include: solvents, paints and coatings, metal solutions, polychlorinated biphenyls (PCBs), pesticides, and acids and alkalis. In studies conducted in the United States, the ten most common hazardous substances found in disposal sites requiring government intervention were lead, arsenic, mercury, vinyl chloride, benzene, cadmium, PCBs, chloroform, benzo(a)pyrene and trichloroethylene. However, chromium, tetrachloroethylene, toluene and di-2-ethylhexylphthalate were also prominent among those substances that could be shown to migrate or for which there was an opportunity for human exposure. The origin of these chemical wastes varies greatly and depends on the local situation, but typically elecroplating solutions, discarded chemicals, manufacturing by-products and waste solvents contribute to the waste stream.
Groundwater Contamination
Figure 1 presents a cross-section of a hypothetical hazardous waste site to illustrate problems that may be encountered. (In practice, such a site should never be placed near a body of water or over a gravel bed.) In well-designed hazardous waste disposal (containment) facilities, there is an effectively impermeable seal to prevent hazardous chemicals from migrating out of the site and into the underlying soil. Such a site also has facilities to treat those chemicals that can be neutralized or transformed and to reduce the volume of waste that goes into the site; those chemicals that cannot be so treated are contained in impermeable containers. (Permeability, however, is relative, as described below.)
Figure 1. Cross-section of a hypothetical hazardous waste site
Chemicals may escape by leaking if the container is compromised, leaching if water gets in or spilling during handling or after the site is disturbed. Once they permeate the liner of a site, or if the liner is broken or if there is no liner, they enter the ground and migrate downward due to gravity. This migration is much more rapid through porous soil and is slow through clay and bedrock. Even underground, water flows downhill and will take the path of least resistance, and so the groundwater level will fall slightly in the direction of flow and the flow will be much faster through sand or gravel. If there is a water table under the ground, the chemicals will eventually reach it. Lighter chemicals tend to float on the groundwater and form an upper layer. Heavier chemicals and water-soluble compounds tend to dissolve or be carried along by the groundwater as it flows slowly underground through porous rock or gravel. The region of contamination, called the plume, can be mapped by drilling test wells, or bore holes. The plume slowly expands and moves in the direction of groundwater movement.
Surface water contamination may occur by runoff from the site, if the top layer of soil is contaminated, or by groundwater. When the groundwater feeds into a local body of water, such as a river or lake, the contamination is carried into this body of water. Some chemicals tend to deposit in the bottom sediment and others are carried along by the flow.
Groundwater contamination may take centuries to clear by itself. If shallow wells are used as a water source by local residents, there is a possibility of exposure by ingestion and by skin contact.
Human Health Concerns
People come into contact with toxic substances in many ways. Exposure to a toxic substance may occur at several points in the use cycle of the substance. People work in a plant where the substances arise as waste from an industrial process and do not change clothes or wash before coming home. They may reside near hazardous waste disposal sites which are illegal or poorly designed or managed, with opportunities for exposure as a result of accidents or careless handling or lack of containment of the substance, or lack of fencing to keep children off the site. Exposure may occur in the home as the result of consumer products that are mislabelled, poorly stored and not child-proof.
Three routes of exposure are by far the most important in considering the implications for toxicity of hazardous waste: inhalation, ingestion and absorption through the skin. Once absorbed, and depending on the route of exposure, there are many ways in which people can be affected by toxic chemicals. Obviously, the list of possible toxic effects associated with hazardous waste is very long. However, public concern and scientific studies have tended to concentrate on the risk of cancer and reproductive effects. In general, this has reflected the profile of chemical hazards at these sites.
There have been many studies of residents who live around or near such sites. With a few exceptions, these studies have shown remarkably little in the way of verifiable, clinically significant health problems. The exceptions have tended to be situations where the contamination is exceptionally severe and there has been a clear pathway of exposure of residents immediately adjacent to the site or who drink well water drawing on groundwater contaminated by the site. There are several likely reasons for this surprising absence of documentable health effects. One is that unlike air pollution and surface water pollution, the chemicals in land pollution are not easily available to people. People may live in areas highly contaminated by chemicals, but unless they actually come in contact with the chemicals by one of the routes of exposure mentioned above, no toxicity will result. Another reason may be that the chronic effects of exposure to these toxic chemicals take a long time to develop and are very difficult to study. Yet another reason may be that these chemicals are less potent in causing chronic health effects in humans than is usually supposed.
Notwithstanding the human health effects, the damage of land pollution to ecosystems may be very great. Plant and animal species, soil bacteria (which contribute to agricultural productivity) and other ecosystem constituents may be irreversibly damaged by degrees of pollution that are not associated with any visible human health effect.
Control of the Problem
Because of population distributions, land use restrictions, transportation costs and concern from society over environmental effects, there is intense pressure to find a solution to the problem of economical disposal of hazardous waste. This has led to increased interest in methods such as source reduction, recycling, chemical neutralization and secure hazardous waste disposal (containment) sites. The first two reduce the amount of waste that is produced. Chemical neutralization reduces the toxicity of the waste and may convert it into a more easily handled solid. Whenever possible, it is preferred that this be done at the site of production of the waste to reduce the amount of waste that must be moved. Well-designed hazardous waste disposal facilities, using the best available technologies of chemical processing and containment, are needed for the residual waste.
Secure hazardous waste containment sites are relatively expensive to build. The site needs to be selected carefully to ensure that pollution of surface water and major aquifers (groundwater) will not readily occur. The site must be designed and built with impermeable barriers to prevent contamination of soil and groundwater. These barriers are typically heavy plastic liners and layers of tamped clay fill under the holding areas. In reality, the barrier acts to delay breakthrough and to slow the permeation that eventually does occur to an acceptable rate, one that will not result in accumulation or significant pollution of groundwater. Permeability is a property of the material, described in terms of the resistance of the material to a liquid or gas penetrating it under given conditions of pressure and temperature. Even the least permeable barrier, such as plastic liners or packed clay, will eventually allow the passage of some liquid chemical through the barrier, although it may take years and even centuries, and once breakthrough occurs the flow becomes continuous, although it may occur at a very low rate. This means that groundwater immediately below a hazardous waste disposal site is always at some risk of contamination, even if it is very small. Once groundwater is contaminated, it is very difficult and often impossible to decontaminate.
Many hazardous waste disposal sites are regularly monitored with collection systems and by testing nearby wells to ensure that pollution is not spreading. The more advanced are built with recycling and processing facilities on-site or nearby to further reduce the waste that goes into the disposal site.
Hazardous waste containment sites are not a perfect solution to the problem of land pollution. They require expensive expertise to design, are expensive to build, and may require monitoring, which creates an ongoing cost. They do not guarantee that groundwater contamination will not occur in the future, although they are effective in minimizing this. A major disadvantage is that someone, inevitably, must live near one. Communities where hazardous waste sites are located or proposed to be located usually oppose them strongly and make it difficult for governments to grant approval. This is called the “not in my back yard” (NIMBY) syndrome and is a common response to the siting of facilities considered undesirable. In the case of hazardous waste sites, the NIMBY syndrome tends to be especially strong.
Unfortunately, without hazardous waste containment sites, society may lose control of the situation entirely. When no hazardous waste site is available, or when it is too expensive to use one, hazardous waste is often disposed of illegally. Such practices include pouring liquid waste on the ground in remote areas, dumping the waste into drains that go into local waterways and shipping the waste to jurisdictions that have more lax laws governing the handling of hazardous waste. This may create an even more dangerous situation than a poorly managed disposal site would create.
There are several technologies that can be used to dispose of the remaining waste. High-temperature incineration is one of the cleanest and most effective means of disposing of hazardous waste, but the cost of these facilities is very high. One of the more promising approaches has been to incinerate liquid toxic waste in cement kilns, which operate at the necessary high temperatures and are found throughout the developing as well as the developed world. Injection into deep wells, below the water table, is one option for chemicals that cannot be disposed of in any other way. However, groundwater migration can be tricky and sometimes unusual pressure situations underground or leaks in the well lead to groundwater contamination anyway. Dehalogenation is a chemical technology that strips the chlorine and bromine atoms from halogenated hydrocarbons, such as PCBs, so that they can be easily disposed of by incineration.
A major unresolved issue in municipal solid waste handling is contamination by hazardous waste discarded by accident or intent. This can be minimized by diverting disposal into a separate waste stream. Most municipal solid waste systems divert chemical and other hazardous wastes so that they do not contaminate the solid waste stream. The separate waste stream should, ideally, be diverted to a secure hazardous waste disposal site.
There is a pressing need for facilities to collect and properly dispose of small quantities of hazardous waste, at minimal cost. Individuals who find themselves in possession of a bottle or can of solvents, pesticides or some unknown powder or fluid usually cannot afford the high cost of proper disposal and do not understand the risk. Some system for collecting such hazardous waste from consumers is needed before it is poured on the ground, flushed down the toilet or burned and released into the air. A number of municipalities sponsor “toxic roundup” days, when residents bring small quantities of toxic materials to a central location for safe disposal. Decentralized systems have been introduced in some urban areas, involving home or local pick-up of small quantities of toxic substances to be discarded. In the United States, experience has shown that people are willing to drive up to five miles to dispose of household toxic wastes safely. Consumer education to promote awareness of the potential toxicity of common products is urgently needed. Pesticides in aerosol cans, bleaches, household cleaners and cleaning fluids are potentially dangerous, especially to children.
Abandoned Hazardous Waste Disposal Sites
Abandoned or insecure hazardous waste sites are a common problem worldwide. Hazardous waste sites that need to be cleaned up are great liabilities to society. The ability of countries and local jurisdictions to clean up major hazardous waste sites varies greatly. Ideally, the owner of the site or the person who created the site should pay for its clean-up. In practice, such sites have often changed hands and the past owners have often gone out of business, the current owners may not have the financial resources to clean up, and the clean-up effort tends to be delayed for very long periods by expensive technical studies followed by legal battles. Smaller and less affluent countries have little leverage in negotiating clean-ups with the current site owners or the responsible parties, and no substantial resources to clean up the site.
The traditional approaches to cleaning up hazardous waste sites are very slow and expensive. It requires highly specialized expertise that is often in short supply. A hazardous waste site is first evaluated to determine how serious the land pollution is and whether the groundwater is contaminated. The likelihood of residents coming into contact with hazardous substances is determined and, in some cases, an estimate of the risk to health that this poses is calculated. Acceptable clean-up levels must be decided upon, the extent to which exposure must ultimately be reduced to protect human health and the environment. Most governments make decisions about clean-up levels by applying various applicable environmental laws, air pollution standards, drinking water standards, and based on a hazards assessment of health risks posed by the particular site. Clean-up levels are therefore set to reflect both health and environmental concerns. A decision must be made on how the site is to be remediated, or how best to achieve this reduction in exposure. Remediation is a technical problem of achieving these clean-up levels by engineering and other methods. Some of the techniques that are used include incineration, solidification, chemical treatment, evaporation, repeated flushing of soil, biodegradation, containment, removal of soil off-site and pumping out groundwater. These engineering options are too complex and specific to the circumstances to describe in detail. Solutions must fit the particular situation and the funds available to achieve control. In some cases, remediation is not feasible. A decision then has to be made on what land use will be permitted on the site.
Water Pollution
For at least two millennia natural water quality has deteriorated progressively and reached contamination levels where water uses are severely limited or the water can be harmful to humans. This deterioration is related to the socio-economic development within a river basin, but long-range atmospheric transport of contaminants has now changed this picture: even remote areas can be indirectly polluted (Meybeck and Helmer 1989).
Medieval reports and complaints about inadequate excreta disposal, foul and stinking water courses within overcrowded cities and other similar problems were an early manifestation of urban water pollution. The first time that a clear causal linkage between bad water quality and human health effects was established was in 1854, when John Snow traced back the outbreak of cholera epidemics in London to a particular drinking water source.
Since the middle of the twentieth century, and concurrent with the onset of accelerated industrial growth, various types of water pollution problems have occurred in rapid succession. Figure 1 illustrates the types of problems as they became apparent in European freshwaters.
Figure 1. Types of water pollution problems
In summarizing the European situation it can be stated that: (1) the challenges of the past (pathogens, oxygen balance, eutrophication, heavy metals) have been recognized, researched and the necessary controls identified and more or less implemented and (2) the challenges of today are of a different nature—on the one hand, “traditional” point and non-point pollution sources (nitrates) and ubiquitous environmental contamination problems (synthetic organics), and, on the other hand, “third generation” problems interfering with global cycles (acidification, climate change).
In the past, water pollution in the developing countries resulted mainly from the discharge of untreated wastewater. Today it is more complex as a result of the production of hazardous wastes from industries and the rapidly increasing use of pesticides in agriculture. In fact, water pollution today in some developing countries, at least in the newly industrializing ones, is worse than in industrialized countries (Arceivala 1989). Unfortunately, developing countries, on the whole, are badly lagging behind in getting control over their major pollution sources. As a consequence, their environmental quality is gradually deteriorating (WHO/UNEP 1991).
Types and Sources of Pollution
There are a large number of microbial agents, elements and compounds which may cause water pollution. They can be classified as: microbiological organisms, biodegradable organic compounds, suspended matter, nitrates, salts, heavy metals, nutrients and organic micropollutants.
Microbiological organisms
Microbiological organisms are common in freshwater bodies polluted particularly by discharges of untreated domestic wastewater. These microbial agents include pathogenic bacteria, viruses, helminths, protozoa and several more complex multicellular organisms that can cause gastro-intestinal illness. Other organisms are more opportunistic in nature, infecting susceptible individuals through body contact with contaminated water or by inhalation of poor quality water droplets in aerosols of various origins.
Biodegradable organic compounds
Organic substances of either natural origin (allochthonous terrestrial detritus or autochthonous debris of aquatic plants) or from anthropogenic sources (domestic, agricultural and some industrial wastes) are decomposed by aerobic microbes as the river continues its course. The consequence is a lowering of the oxygen level downstream of the wastewater discharge, impairing the quality of the water and the survival of the aquatic biota, particularly of high-quality fish.
Particulate matter
Particulate matter is a major carrier of organic and inorganic pollutants. Most toxic heavy metals, organic pollutants, pathogens and nutrients, such as phosphorus, are found in suspended matter. An appreciable amount of the biodegradable organic material responsible for consumption of dissolved oxygen from rivers is also found in suspended particles. Particulate matter comes from urbanization and road construction, deforestation, mining operations, dredging operations in rivers, natural sources which are linked to continental erosion, or natural catastrophic events. Coarser particles are deposited on river beds, in reservoirs, in the flood plain and in wetlands and lakes.
Nitrates
The concentration of nitrates in unpolluted surface waters ranges from less than 0.1 to one milligrams per litre (expressed as nitrogen), so nitrate levels in excess of 1 mg/l indicate anthropogenic influences such as discharge of municipal wastes and urban and agricultural run-off. Atmospheric precipitation is also an important source of nitrate and ammonia to river basins, particularly in areas not affected by direct pollution sources—for example, some tropical regions. High concentrations of nitrate in drinking water may lead to acute toxicity in bottle-fed infants during their first months of life, or in the elderly, a phenomenon called methaemoglobinaemia.
Salts
Water salinization may be caused by natural conditions, such as geochemical interaction of waters with salty soils or by anthropogenic activities, including irrigated agriculture, sea water intrusion due to excessive pumping of groundwaters in islands and coastal areas, disposal of industrial wastes and of oilfield brines, highway de-icing, landfill leachates and leaking sewers.
While hampering beneficial uses, particularly for irrigation of sensitive crops or for drinking, salinity in itself may not, at even quite high levels, be directly harmful to health, but the indirect effects can be dramatic. The loss of fertile agricultural land and reduced crop yields caused by waterlogging and soil salinization of irrigated areas destroy the livelihood of whole communities and cause hardships in the form of food shortages.
Heavy metals
Heavy metals such as lead, cadmium and mercury are micro-pollutants and of special interest as they have health and environmental significance due to their persistence, high toxicity and bio-accumulation characteristics.
There are basically five sources of heavy metals contributing to water pollution: geological weathering, which provides the background level; industrial processing of ores and metals; the use of metal and metal compounds, such as chromium salts in tanneries, copper compounds in agriculture, and tetraethyl lead as an anti-knock agent in gasoline; leaching of heavy metals from domestic wastes and solid waste dumps; and heavy metals in human and animal excretions, particularly zinc. Metals released to the air from automobiles, fuel burning and industrial process emissions may settle on land and ultimately run off to surface waters.
Nutrients
Eutrophication is defined as the enrichment of waters with plant nutrients, primarily phosphorus and nitrogen, leading to enhanced plant growth (both algae and macrophytes) which results in visible algae blooms, floating algal or macrophyte mats, benthic algae and submerged macrophyte agglomerations. When decaying, this plant material leads to the depletion of the oxygen reserves of water bodies, which, in turn, causes an array of secondary problems such as fish mortality and liberation of corrosive gases and other undesirable substances, such as carbonic gas, methane, hydrogen sulphide, organoleptic substances (causing taste and odour), toxins and so on.
The source of phosphorus and nitrogen compounds is primarily untreated domestic wastewater, but other sources such as drainage of artificially fertilized agricultural land, surface run-off from intensive livestock farming and some industrial wastewaters can also substantially increase the trophic level of lakes and reservoirs, particularly in tropical developing countries.
The main problems associated with eutrophication of lakes, reservoirs and impoundments are: oxygen depletion of the bottom layer of lakes and reservoirs; water quality impairment, leading to treatment difficulties, particularly for the removal of taste- and odour-causing substances; recreational impairment, increased health hazards to bathers and unsightliness; fisheries impairment due to fish mortality and the development of undesirable and low-quality fish stocks; ageing and reducing the holding capacity of lakes and reservoirs by silting; and increase of corrosion problems in pipes and other structures.
Organic micropollutants
Organic micropollutants can be classified in groups of chemical products on the basis of how they are used and consequently how they are dispersed in the environment:
- Pesticides are substances, generally synthetic, that are deliberately introduced into the environment to protect crops or control disease vectors. They are found in various distinct families, such as organochloride insecticides, organophosphate insecticides, herbicides of the plant hormone type, triazines, substituted ureas and others.
- Materials for widespread household and industrial use comprise volatile organic substances used as extraction solvents, solvents for degreasing metals and dry-cleaning clothes, and propellants for use in aerosol containers. This group also includes halogenated derivatives of methane, ethane and ethylene. As they are widely used their rates of dispersion in the environment, compared with the amounts produced, are generally high. The group also contains the polycyclic aromatic hydrocarbons, whose presence in the environment results from the extraction, transport and refining of petroleum products and the dispersion of combustion products resulting from their use (petrol and heating oil).
- Materials used essentially in industry include substances which are direct or intermediate agents of chemical synthesis, such as carbon tetrachloride for synthesizing freons; vinyl chloride for polymerizing PVC; and chlorinated derivates of benzene, naphthalene, phenol and aniline for manufacturing dyestuffs. The group also contains finished products used in closed systems, such as heat-exchange fluids and dielectrics.
Organic micropollutants are generated from point and diffuse sources, either urban or rural. The largest part originates in major industrial activities such as petrol refining, coal mining, organic synthesis and the manufacture of synthetic products, the iron and steel industries, the textile industry and the wood and pulp industry. Effluents from pesticides factories may contain considerable quantities of these manufactured products. A significant proportion of organic pollutants are discharged into the aquatic environment as run-off from urban surfaces; and in agricultural areas, pesticides applied to crops may reach surface waters through rainwater run-off and artificial or natural drainage. Also, accidental discharges have led to severe ecological damage and temporary closure of water supplies.
Urban Pollution
Owing to this continuously expanding, aggressive and multi-faceted pollution scenario, the problem of maintaining the quality of water resources has become acute, particularly in the more urbanized areas of the developing world. Maintaining water quality is hampered by two factors: failure to enforce pollution control at the main sources, especially industries, and inadequacy of sanitation systems and of garbage collection and disposal (WHO 1992b). See some examples of water pollution in different cities in developing countries.
Examples of water pollution in selected cities
Karachi (Pakistan)
The Lyari river, which runs through Karachi, Pakistan’s largest industrial city, is an open drain from both the chemical and the microbiological point of view, a mixture of raw sewage and untreated industrial effluents. Most industrial effluents come from an industrial estate with some 300 major industries and almost three times as many small units. Three-fifths of the units are textile mills. Most other industries in Karachi also discharge untreated effluents into the nearest water body.
Alexandria (Egypt)
Industries in Alexandria account for around 40% of all Egypt’s industrial output, and most discharge untreated liquid wastes into the sea or into Lake Maryut. In the past decade, fish production in Lake Maryut declined by some 80% because of the direct discharge of industrial and domestic effluents. The lake has also ceased to be a prime recreational site because of its poor condition. Similar environmental degradation is taking place along the seafront as a result of the discharge of untreated wastewater from poorly located outfalls.
Shanghai (China)
Some 3.4 million cubic metres of industrial and domestic waste pour mostly into the Suzhou Creek and the Huangpu River, which flows through the heart of the city. These have become the main (open) sewers for the city. Most of the waste is industrial, since few houses possess flush toilets. The Huangpu has essentially been dead since 1980. In all, less than 5% of the city’s wastewater is treated. The normally high water table also means that a variety of toxins from industrial plants and local rivers find their way into groundwater and contaminate wells, which also contribute to the city water supply.
São Paulo (Brazil)
The Tiete River, as it passes through Greater São Paulo, one of the world’s largest urban agglomerations, receives 300 tonnes of effluents each day from 1,200 industries located in the region. Lead, cadmium and other heavy metals are among the main pollutants. It also receives 900 tonnes of sewage each day, of which only 12.5% is treated by the five sewage treatment stations located in the area.
Source: Based on Hardoy and Satterthwaite 1989.
Health Impacts of Microbial Pollution
Diseases arising from the ingestion of pathogens in contaminated water have the greatest impact worldwide. “An estimated 80% of all diseases, and over one-third of deaths in developing countries are caused by the consumption of contaminated water, and on average as much as one-tenth of each person’s productive time is sacrificed to water-related diseases” (UNCED 1992). Water-borne diseases are the largest single category of communicable diseases contributing to infant mortality in developing countries and second only to tuberculosis in contributing to adult mortality, with one million deaths per year.
The total annual number of cholera cases reported to the WHO by its member states has reached levels unprecedented during the seventh pandemic, with a peak of 595,000 cases in 1991 (WHO 1993). Table 1 shows the global morbidity and mortality rates of the major water-related diseases. These figures are, in many cases, grossly underestimated, since reporting of disease cases is done quite erratically by many countries.
Table 1. Global morbidity and mortality rates of main diseases related to water
|
Number/Year or Reporting Period |
||
|
Disease |
Cases |
Deaths |
|
Cholera - 1993 |
297,000 |
4,971 |
|
Typhoid |
500,000 |
25,000 |
|
Giardiasis |
500,000 |
Low |
|
Amoebiasis |
48,000,000 |
110,000 |
|
Diarrhoeal disease (under 5 years) |
1,600,000,000 |
3,200,000 |
|
Dracunculiasis (Guinea Worm) |
2,600,000 |
- |
|
Schistosomiasis |
200,000,000 |
200,000 |
Source: Galal-Gorchev 1994.
Health Impacts of Chemical Pollution
The health problems associated with chemical substances dissolved in water arise primarily from their ability to cause adverse effects after prolonged periods of exposure; of particular concern are contaminants that have cumulative toxic properties such as heavy metals and some organic micropollutants, substances that are carcinogenic and substances that may cause reproductive and developmental effects. Other dissolved substances in water are essential ingredients of dietary intake and yet others are neutral with regards to human needs. Chemicals in water, particularly in drinking water, may be classified into three typical categories for the purpose of health impact (Galal-Gorchev 1986):
- Substances exerting an acute or chronic toxicity upon consumption. The severity of the health impairment increases with the increase of their concentration in drinking water. On the other hand, below a certain threshold concentration no health effects can be observed—that is, the human metabolism can handle this exposure without measurable long-term effects. Various metals, nitrates, cyanides and so on fall within this category.
- Genotoxic substances, which cause health effects such as carcinogenicity, mutagenicity and birth-defects. According to present scientific thinking there is no threshold level which could be considered safe, since any amount of the substance ingested contributes to an increase in cancer and similar risks. Complex mathematical extrapolation models are used to determine such risks, since very little epidemiological evidence exists. Synthetic organics, many chlorinated organic micropollutants, some pesticides and arsenic fall within this category.
- For some elements, such as fluoride, iodine and selenium, the contribution made by drinking water is crucial and, if deficient, causes more or less severe health effects. At high concentrations, however, these same substances cause equally severe health effects, but of a different nature.
Environmental Impacts
The impacts of environmental pollution on freshwater quality are numerous and have existed for a long time. Industrial development, the advent of intensive agriculture, the exponential development of human populations and the production and use of tens of thousands of synthetic chemicals are among the main causes of water quality deterioration at local, national and global scales. The major issue of water pollution is the interference with actual or planned water uses.
One of the most severe and ubiquitous causes of environmental degradation is the discharge of organic wastes into watercourses (see “Biodegradable organic compounds” above). This pollution is mainly of concern in the aquatic environment where many organisms, for example fish, require high oxygen levels. A serious side effect of water anoxia is the release of toxic substances from particulates and bottom sediments in rivers and lakes. Other pollution effects from domestic sewage discharges into watercourses and aquifers include the build-up of nitrate levels in rivers and groundwaters, and the eutrophication of lakes and reservoirs (see above, “Nitrates” and “Salts”). In both cases, the pollution is a synergistic effect of sewage effluents and agricultural run-off or infiltration.
Economic Impacts
The economic consequences of water pollution can be rather severe due to detrimental effects on human health or on the environment. Impaired health often lowers human productivity, and environmental degradation reduces the productivity of water resources used directly by people.
The economic disease burden can be expressed not only in costs of treatment, but also in quantifying the loss of productivity. This is particularly true for primarily disabling diseases, such as diarrhoea or Guinea Worm. In India, for example, there are about 73 million workdays per year estimated to be lost due to water-related diseases (Arceivala 1989).
Deficiencies in sanitation and the resulting epidemics can also lead to severe economic penalties. This became most apparent during the recent cholera epidemic in Latin America. During the cholera epidemic in Peru, losses from reduced agricultural exports and tourism were estimated at one billion US dollars. This is more than three times the amount that the country had invested in water supply and sanitation services during the 1980s (World Bank 1992).
Water resources affected by pollution become less suitable as sources of water for municipal supply. As a consequence, expensive treatment has to be installed or clean water from far away has to be piped to the city at much higher costs.
In the developing countries of Asia and the Pacific, environmental damage was estimated by Economic and Social Commission for Asia and the Pacific (ESCAP) in 1985 to cost about 3% of the GNP, amounting to US$250 billion, while the cost of repairing such damage would range around 1%.
Energy and Health
The WHO Commission on Health and Environment (1992a) Panel on Energy considered four energy-related issues to be of the highest immediate and/or future concern for environmental health:
- exposure to noxious agents in the course of domestic utilization of biomass and coal
- exposure resulting from urban air pollution in numerous large cities of the world
- the possible health-related impacts of climate change
- serious accidents with environmental impacts on the health of the general public.
Quantitative assessment of the health risks from different energy systems requires system-wide evaluation of all steps in a fuel cycle, starting with extraction of raw resources, and concluding with the final consumption of energy. For valid intertechnology comparisons to be made, methods, data and end-use demands must be similar and specified. In quantifying the effects of end-use demands, differences in conversion efficiencies of energy- and fuel-specific devices to useful energy must be evaluated.
Comparative assessment is built around the idea of the Reference Energy System (RES), which depicts fuel cycles step-by-step, from extraction through processing to combustion and ultimate disposal of wastes. The RES provides a common, simple framework for defining flows of energy and related data used for risk assessment. An RES (figure 1) is a network representation of the main components of an energy system for a given year, specifying resource consumption, fuel transportation, conversion processes and end uses, thereby compactly incorporating the salient features of the energy system while providing a framework for assessment of major resource, environmental, health and economic effects that can result from new technologies or policies.
Figure 1. Reference energy system, year 1979
Based on their health risks, energy technologies can be classified into three groups:
- The fuels group is characterized by use of large amounts of fossil fuels or biomass—coal, oil, natural gas, wood and so on—the collection, processing and transport of which have high accident rates that dominate occupational risks and the burning of which produces large amounts of air pollution and solid waste that dominate public risks.
- The renewable group is characterized by use of diffuse renewable resources with low energy density—sun, wind, water—which are available in enormous quantities at no cost, but the capturing of which requires large areas and construction of expensive facilities capable of “concentrating” them into useful forms. Occupational risks are high and dominated by construction of the facilities. Public risks are low, mostly confined to low-probability accidents, such as dam failures, equipment failures and fires.
- The nuclear group includes nuclear fission technologies, distinguished by extremely high energy densities in the processed fuel, with corresponding low quantities of fuel and wastes to process, but with low concentrations in the earth’s crust, necessitating a large mining or collection effort. Occupational risks are, therefore, relatively high and dominated by mining and processing accidents. Public risks are small and dominated by routine operations of reactors. Special attention must be given to public fears of risks from exposure to radiation from nuclear technologies—fears which are relatively large per unit risk to health.
The significant health effects of technologies for generating electricity are shown in table 1, table 2 and table 3.
Table 1. Significant health effects of technologies for generating electricity - fuels group
|
Technology |
Occupational |
Public health effects |
|
Coal |
Black lung disease |
Air pollution health effects |
|
Oil |
Trauma from drilling accidents |
Air pollution health effects |
|
Oil shale |
Brown lung disease |
Cancer from exposure to |
|
Natural gas |
Trauma from drilling accidents |
Air pollution health effects |
|
Tar sands |
Trauma from mining accidents |
Air pollution health effects |
|
Biomass* |
Trauma from accidents during |
Air pollution health effects |
* As an energy source, usually considered as renewable.
Table 2. Significant health effects of technologies for generating electricity - renewable group
|
Technology |
Occupational |
Public health effects |
|
Geothermal |
Exposure to toxic gases - |
Disease from exposure to toxic |
|
Hydropower, |
Trauma from construction |
Trauma from dam failures |
|
Photovoltaics |
Exposure to toxic materials |
Exposure to toxic materials |
|
Wind |
Trauma from accidents during |
|
|
Solar thermal |
Trauma from accidents during |
Table 3. Significant health effects of technologies for generating electricity - nuclear group
|
Technology |
Occupational |
Public health effects |
|
Fission |
Cancer from exposure to radiation
|
Cancer from exposure to radiation
|
Studies of health effects of wood burning in the United States, like analyses of other energy sources, were based on the health effects of supplying a unit amount of energy, that is, that needed to heat one million dwelling years. This is 6 ×107 GJ heat, or 8.8 ×107 GJ wood input at 69% efficiency. Health effects were estimated in gathering, transport and combustion stages. Oil and coal alternatives were scaled from earlier work (see figure 2). The uncertainties in gathering are ± a factor of ~2, those in home fires ± a factor of ~3, and those in air pollution ± a factor greater than 10. If the hazards of nuclear electric were plotted on the same scale, the total risk would be approximately one-half that of mining for coal mining.
Figure 2. Health effects per unit amount of energy
A convenient way to help understand the risk is to scale it to a single person supplying one dwelling with wood over 40 years (figure 3). This results in a total risk of fatality of ~1.6 x 10–3 (i.e., ~0.2%). This can be compared with the risk of death in an automobile accident in the United States during the same time, ~9.3 x 10–3 (i.e., ~1%), which is five times greater. Wood burning presents risks which are of the same order as more conventional heating technologies. Both are well below the overall risk of other common activities, and many aspects of the risk are clearly amenable to preventive measures.
Figure 3. Risk, to a single person, of fatality due to supplying one dwelling with wood fuel for 40 years
The following comparisons for health risks can be made:
- Acute occupational risk. For the coal cycle, occupational risk is distinctly higher than that associated with oil and gas; it is about the same as that associated with renewable energy systems, when their construction is included in the assessment, and it is about 8-10 times higher than the corresponding risks for nuclear. Future technological advances in renewable solar and wind energy sources may result in a significant reduction in the acute occupational risk associated with these systems. Hydro-electricity generation entails comparatively high acute occupational risk.
- Late occupational risk. Late fatalities arise mainly in coal and uranium mining, and are roughly of the same size. Underground coal mining, however, appears to be more dangerous than underground uranium mining (calculation from the basis of a normalized unit of electricity generated). Use of surface-mined coal, on the other hand, leads in total to fewer late fatalities than does use of nuclear energy.
- Acute public risk. These risks, mostly due to transportation accidents, are highly dependent on distance travelled and mode of transport. The risk of nuclear is 10-100 times lower than those of all the other options, mainly because of the relatively low quantity of materials to be transported. The coal cycle has the highest acute public risk because of the large material transport using the same reasoning.
- Late public risk. There are great uncertainties associated with late public risks associated with all the energy sources. Late public risks for nuclear and natural gas are about equal and are, at least ten times lower than those associated with coal and oil. Future developments are expected to result in significant decreases in late public risks for renewables.
Clearly, health effects of different energy sources depend on the quantity and type of energy use. These vary greatly geographically. Fuelwood is the fourth largest contribution to world energy supply, after petroleum, coal and natural gas. Close to half the world population, especially those living in the rural and urban areas of developing countries, depend on it for cooking and heating (either wood or its derivative, charcoal, or, in the absence of either of these, on agricultural residues or dung). Fuelwood constitutes more than half the world’s consumption of wood, rising to 86% in developing countries and 91% in Africa.
In considering new and renewable sources of energy such as solar energy, wind power, and alcohol fuels, the idea of a “fuel cycle” must encompass industries such as solar photovoltaics, where virtually no risk attaches to the operation of the device but a substantial amount—often ignored—may be involved in its manufacture.
Attempts were made to deal with this difficulty by expanding the fuel cycle concept to include all stages in developing an energy system—including, for example, the concrete that goes into the plant that manufactures the glass for the solar collector. The issue of completeness has been addressed by noting that the backward analysis of manufacturing steps is equivalent to a set of simultaneous equations whose solution—if linear—is expressible as a matrix of values. Such an approach is familiar to economists as input-output analysis; and the appropriate numbers, showing how much each economic activity draws on the others, have already been derived—although for aggregate categories that may not exactly match the manufacturing steps one wishes to scrutinize for measuring health damage.
No single method of comparative risk analysis in the energy industry is fully satisfactory by itself. Each has advantages and limitations; each provides a different kind of information. Given the level of uncertainty of health risk analyses, results from all methods should be examined to provide as detailed a picture as possible, and fuller understanding of the magnitudes of associated uncertainties.
Urbanization
Urbanization is a major feature of the contemporary world. At the beginning of the nineteenth century there were some 50 million people living in urban areas. By 1975 there were 1.6 billion, and by the year 2000 there will be 3.1 billion (Harpham, Lusty and Vaugham 1988). Such figures outstrip by far the growth of rural population.
However, the process of urbanization has often had hazardous impacts on the health of those who work and live in cities and towns. To a greater or lesser extent, the production of adequate housing, the provision of urban infrastructure and the control of traffic has not kept pace with the growth of urban population. This has generated a myriad of health problems.
Housing
Housing conditions throughout the world are far from adequate. For example, by the mid-1980s, 40 to 50% of the population in many cities in developing countries were living in substandard accommodations (WHO Commission on Health and Environment 1992b). Such figures have increased ever since. Although the situation in industrialized countries is less critical, housing problems such as decay, overcrowding and even homelessness are frequent.
The major aspects of the residential environment which influence health, and their associated hazards, are presented in table 1. The health of a worker is likely to be affected if his or her residence is deficient in one or more of these aspects. In developing countries, for instance, some 600 million urban dwellers live in health- and life-threatening homes and neighbourhoods (Hardoy, Cairncross and Satterthwaite 1990; WHO 1992b).
Table 1. Housing and health
|
Housing problems |
Health hazards |
|
Poor control of temperature |
Heat stress, hypothermia |
|
Poor control of ventilation |
Acute and chronic respiratory diseases |
|
Poor control of dust |
Asthma |
|
Overcrowding |
Household accidents, easier spread of |
|
Poor control of open fires, poor protection |
Burns |
|
Poor finishing of walls, floors or roofs |
Chagas’ disease, plague, typhus, shigellosis, |
|
Siting of house |
Malaria, schistosomiasis, filariasis, |
|
Siting of house (in area prone to disasters such as landslides |
Accidents |
|
Construction defects |
Accidents |
Source: Hardoy et al. 1990; Harpham et al. 1988; WHO Commission on Health and Environment 1992b.
Housing problems may also have a direct effect on occupational health, in the case of those who work in residential environments. Those include domestic servants and also a growing number of small-scale producers in a variety of cottage industries. These producers may be further affected when their production processes generate some form of pollution. Selected studies in these types of industries have detected hazardous wastes with consequences such as cardiovascular diseases, skin cancer, neurological disorders, bronchial cancer, photophobia and infant methaemoglobinaemia (Hamza 1991).
Prevention of home-related problems includes action in different stages of housing provision:
- location (e.g., safe and vector-free sites)
- house design (e.g., spaces with adequate size and climatic protection, use of non-perishable building materials, adequate protection for equipment)
- construction (prevention of construction defects)
- maintenance (e.g., proper control of equipment, proper screening).
The insertion of industrial activities in the residential environment may require special measures of protection, according to the particular process of production.
The specific housing solutions may vary widely from place to place, depending on the social, economic, technical and cultural circumstances. A great number of cities and towns do have local planning and building legislation that includes measures to prevent health hazards. However, such legislation is often not enforced due to ignorance, lack of legal control or, in most cases, lack of financial resources to build proper housing. Therefore, it is important not only to design (and update) adequate codes, but also to create the conditions for their implementation.
Urban Infrastructure: The Provision of Environmental Health Services
Housing may also affect health when it is not properly supplied with environmental health services such as garbage collection, water, sanitation and drainage. The inadequate provision of these services, however, extend beyond the housing realm, and may cause hazards for the city or town as a whole. Standards of provision of these services are still critical in a large number of places. For example, 30 to 50% of solid waste generated within urban centres is left uncollected. In 1985 there were 100 million more people without water service than in 1975. More than two billion people still have no sanitary means to dispose of human waste (Hardoy, Cairncross and Satterthwaite 1990; WHO Commission on Health and Environment 1992b). And the media have frequently shown cases of floods and other accidents connected to inadequate urban drainage.
Hazards derived from deficient provision of environmental health services are presented in table 2. Cross-service hazards are also common—e.g., contamination of water supply due to lack of sanitation, dissemination of refuse through non-drained water. To give one illustration of the extent of infrastructural problems among many, a child is killed worldwide every 20 seconds due to diarrhoea—which is a major outcome of deficient environmental health services.
Table 2. Urban infrastructure and health
|
Problems in the provision of |
Health hazards |
|
Uncollected garbage |
Pathogens in the refuse, disease vectors (mainly flies and rats) which breed or feed in the refuse, fire hazards, pollution of water flows |
|
Deficiency in quantity and/or |
Diarrhoea, trachoma, infectious skin diseases, infections carried out by body lice, other diseases originated by consumption of non-washed food |
|
Lack of sanitation |
Faeco-oral infections (e.g., diarrhoea, cholera, typhoid fever), intestinal parasites, filariasis |
|
Lack of drainage |
Accidents (from floods, landslides, collapsing houses), faeco-oral infections, schistosomiasis, mosquito-borne diseases (e.g., malaria, dengue, yellow fever), Bancroftian filariasis |
Source: Hardoy et al. 1990; WHO Commission on Health and Environment 1992b.
Those labourers whose immediate or wider working environment is not adequately supplied with such services are exposed to a profusion of occupational health risks. Those who work in the provision or maintenance of services, such as garbage pickers, sweepers and scavengers, are further exposed.
There exist indeed technical solutions capable of ameliorating the provision of environmental health services. They encompass, among many others, garbage recycling schemes (including support to scavengers), use of different kinds of garbage collection vehicles to reach different types of roads (including those of informal settlements), water-saving fittings, tighter control of water leakages and low-cost sanitation schemes such as ventilated pit latrines, septic tanks or small-bore sewers.
However, the success of each solution will depend on its appropriateness to the local circumstances and on the local resources and capacity to implement it. Political willingness is fundamental, but not enough. Governments have frequently found it difficult to provide urban services adequately by themselves. Success stories of good supply have often included cooperation between the public, private and/or voluntary sectors. A thorough involvement and support of the local communities is important. This often requires official recognition of the large number of illegal and semi-legal settlements (especially but not only in developing countries), which bear a heavy part of the environmental health problems. Workers directly involved in services such as garbage collection or recycling and sewerage maintenance need special equipment for protection, such as gloves, overalls and masks.
Traffic
Cities and towns have depended heavily on ground transport for the movement of people and goods. Thus, the increase in urbanization throughout the world has been accompanied by a sharp growth in urban traffic. However, such a situation has generated a large number of accidents. Some 500,000 people are killed in traffic accidents each year, two-thirds of which occur in urban or peri-urban areas. In addition, according to many studies in different countries, for every death there are ten to twenty persons injured. Many cases suffer permanent or prolonged loss of productivity (Urban Edge 1990a; WHO Commission on Health and Environment 1992a). A large share of such data relates to people on their way to or from work—and such a type of traffic accident has lately been considered an occupational hazard.
According to World Bank studies, the main causes of urban traffic accidents include: poor condition of vehicles; deteriorated streets; different types of traffic—from pedestrians and animals to trucks—sharing the same streets or lanes; non-existent foot-paths; and reckless road behaviour (both from drivers and pedestrians) (Urban Edge 1990a, 1990b).
A further hazard generated by the expansion of urban traffic is air and noise pollution. Health problems include acute and chronic respiratory diseases, malignancies and hearing deficiencies (pollution is also dealt with in other articles in this Encyclopaedia).
Technical solutions to ameliorate road and car safety (as well as pollution) abound. The major challenge seems to be changing the attitudes of drivers, pedestrians and public officials. Road safety education—from elementary school teaching to campaigns throughout the media—has often been recommended as a policy to target drivers and/or pedestrians (and such programmes have often had some degree of success when implemented). Public officials have the responsibility to design and enforce traffic legislation, inspect vehicles and design and implement engineering safety measures. However, according to the aforementioned studies, these officials seldom perceive traffic accidents (or pollution) as a top priority, or have the means to act dutifully (Urban Edge 1990a, 1990b). Therefore, they have to be targeted by educational campaigns, and supported in their work.
The Urban Fabric
In addition to the specific issues already noted (housing, services, traffic), the overall growth of the urban fabric also has had an impact on health. Firstly, urban areas are usually dense, a fact which facilitates the spread of communicable diseases. Secondly, such areas concentrate a large number of industries, and their associated pollution. Thirdly, through the process of urban growth, natural foci of disease vectors may get entrapped within new urban areas, and new niches for disease vectors may be established. Vectors may adapt to new (urban) habitats—for example, those responsible for urban malaria, dengue and yellow fever. Fourthly, urbanization has often had psychosocial consequences such as stress, alienation, instability and insecurity; which, in their turn, have led to problems such as depression and alcohol and drug abuse (Harpham, Lusty and Vaugham 1988; WHO Commission on Health and Environment 1992a).
Past experiences have demonstrated the possibility (and the need) to tackle health problems via improvements in urbanization. For instance, “¼ the remarkable decline in mortality rates and improvements in health in Europe and North America at the turn of the last century owe more to improved nutrition and improvements in water supply, sanitation and other aspects of housing and living conditions than to medical establishments” (Hardoy, Cairncross and Satterthwaite 1990).
Solutions for the mounting problems of urbanization need sound integration between (often separated) urban planning and management, and the participation of the different public, private and voluntary actors which operate in the urban arena. Urbanization affects a wide range of workers. Contrary to other sources or types of health problems (which might affect specific categories of workers), occupational hazards derived from urbanization cannot be dealt with through single trade union action or pressure. They require inter-profession action, or, even more broadly, action from the urban community in general.
Global Climate Change and Ozone Depletion
Climate Change
The major greenhouse gases (GHGs) consist of carbon dioxide, methane, nitrous oxide, water vapour and chlorofluorocarbons (CFCs). These gases allow sunlight to penetrate to the earth’s surface, yet prevent infrared radiant heat from escaping. The Intergovernmental Panel on Climate Change (IPCC) of the United Nations has concluded that emissions, primarily from industry, and destruction of greenhouse gas sinks, via poor land use management, especially deforestation, have substantially increased the concentrations of GHGs beyond natural processes. Without major policy shifts, pre-industrial carbon dioxide levels are expected to increase, yielding a 1.0-3.5°C rise in average global temperature by the year 2100 (IPCC in press).
The two primary components of climate change include (1) temperature elevation with concomitant weather instability and extremes and (2) rising sea-level due to thermoexpansion. These changes may result in an increased frequency of heat waves and hazardous air pollution episodes, reduced soil moisture, higher incidence of disruptive weather events, and coastal inundation (IPCC 1992). Subsequent health effects may include an increase in (1) heat-related mortality and morbidity; (2) infectious diseases, particularly those that are insect borne; (3) malnutrition from food supply shortages; and (4) public health infrastructural crises from weather disasters and sea-level rise, coupled with climate-related human migration (see figure 1).
Figure 1. Public health effects from the major components of global climate change
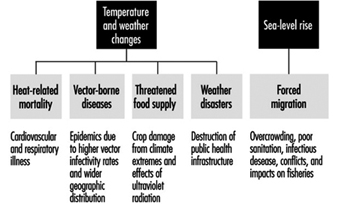 Humans have an enormous capacity to adapt to climatic and environmental conditions. However, the rate of predicted climatic and potential ecological change is of great concern to medical and earth scientists alike. Many of the health effects will be mediated through ecological responses to altered climate conditions. For example, spread of vector-borne diseases will depend on shifts in vegetation and availability of reservoir or intermediate hosts, in conjunction with the direct effects of temperature and humidity on parasites and their vectors (Patz et al. 1996). Understanding the hazards of climate change will, therefore, require an integrated ecological risk assessment which demands new and complex approaches compared to conventional single-agent cause-and-effect risk analysis from empirical data (McMichael 1993).
Humans have an enormous capacity to adapt to climatic and environmental conditions. However, the rate of predicted climatic and potential ecological change is of great concern to medical and earth scientists alike. Many of the health effects will be mediated through ecological responses to altered climate conditions. For example, spread of vector-borne diseases will depend on shifts in vegetation and availability of reservoir or intermediate hosts, in conjunction with the direct effects of temperature and humidity on parasites and their vectors (Patz et al. 1996). Understanding the hazards of climate change will, therefore, require an integrated ecological risk assessment which demands new and complex approaches compared to conventional single-agent cause-and-effect risk analysis from empirical data (McMichael 1993).
Stratospheric Ozone Depletion
Stratospheric ozone depletion is occurring primarily from reactions with halogen free radicals from chlorofluorocarbons (CFCs), along with other halocarbons and methyl bromide (Molina and Rowland 1974). Ozone specifically blocks the penetration of ultravioletB radiation (UVB), which contains the most biologically destructive wavelengths (290-320 nanometres). UVB levels are expected to rise disproportionately in temperate and arctic zones, since a clear relationship has been established between higher latitudes and the extent of ozone thinning (Stolarski et al. 1992).
For the period 1979-91, average ozone loss has been estimated at 2.7% per decade, correcting for solar cycle and other factors (Gleason et al. 1993). In 1993, researchers using a sensitive new spectroradiometer in Toronto, Canada, discovered that current ozone depletion has caused local increases in ambient UVB radiation of 35% in winter and 7% in summer, relative to 1989 levels (Kerr and McElroy 1993). Earlier estimates by the UN Environment Programme (UNEP) predicted a 1.4% rise in UVB per 1% drop in stratospheric ozone (UNEP 1991a).
The direct health impacts from stratospheric ozone depletion, which leads to increased ambient UVB radiation, include (1) skin cancer (2) ocular diseases and (3) immunosuppression. Indirect effects to health may occur from crop damage by ultraviolet radiation.
Health Effects of Temperature and Precipitation Change
Heat-related morbidity and mortality
Physiologically, humans have a great capacity for thermoregulation up to a threshold temperature. Weather conditions exceeding threshold temperatures and persisting for several consecutive days cause increased mortality in the population. In large cities, poor housing combined with the urban “heat island” effect further exacerbate conditions. In Shanghai, for instance, this effect can be as high as 6.5 °C on a windless evening during winter (IPCC 1990). Most heat-related fatalities occur in the elderly population and are attributed to cardiovascular and respiratory disorders (Kilbourne 1989). Key meteorological variables contribute to heat-related mortality, the most significant being high night-time readings; the greenhouse effect is predicted to especially elevate these minimum temperatures (Kalkstein and Smoyer 1993).
Temperate and polar regions are expected to warm disproportionately more than tropical and subtropical zones (IPCC 1990). Based on predictions by the US National Aeronautics and Space Administration (NASA), average summer temperatures in New York and St. Louis, for example, would rise by 3.1 and 3.9 °C, respectively, if ambient CO2 doubles. Even with adjustment for physiological acclimatization, annual summer mortality in temperate cities such as these could rise over fourfold (Kalkstein and Smoyer 1993).
Atmospheric chemistry is an important contributing factor in the formation of urban photochemical smog, whereby photodecomposition of NO2 in the presence of volatile organic compounds results in the production of tropospheric (ground-level) ozone. Both increased ambient UV radiation and warmer temperatures would further drive these reactions. Adverse health effects from air pollution are well known, and continued fossil fuel use will extend acute and chronic health impacts. (see “Air pollution” in this chapter).
Infectious diseases and climate/ecosystem change
Coupled atmosphere-ocean general circulation models predict that high latitudes in the northern hemisphere will experience the largest surface temperature elevation based on current IPCC scenarios (IPCC 1992). Minimum winter temperatures are expected to be disproportionately more affected, allowing for certain viruses and parasites to extend into regions where they previously could not live. In addition to direct climate effects on vectors, transformation of ecosystems could have marked implications for diseases whereby the geographic range of vector and/or reservoir host species is defined by these ecosystems.
Vector-borne diseases may spread to temperate regions in both hemispheres and intensify in endemic areas. Temperature determines vector infectivity by affecting pathogen replication, maturation and the period of infectivity (Longstreth and Wiseman 1989). Elevated temperature and humidity also intensify the biting behaviour of several mosquito species. Extreme heat, on the other hand, can shorten insect survival time.
Infectious diseases which incorporate a cold-blooded species (invertebrate) within their life cycles, are most susceptible to subtle climate variations (Sharp 1994). Diseases whose infectious agents, vectors or hosts are affected by climate change include malaria, schistosomiasis, filariasis, leishmaniasis, onchocerciasis (river blindness), trypanosomiasis (Chagas’ and African sleeping sickness), dengue, yellow fever and arboviral encephalitis. Current figures of the number of people at risk of these diseases are listed in table 1 (WHO 1990d).
Table 1. Global status of major vector-borne diseases
|
No.a |
Disease |
Population at risk |
Prevalence of infection |
Present distribution |
Possible change of distribution as a result of climatic change |
|
1. |
Malaria |
2,100 |
270 |
Tropics/subtropics |
++ |
|
2. |
Lymphatic filariases |
900 |
90.2 |
Tropics/subtropics |
+ |
|
3. |
Onchocerciasis |
90 |
17.8 |
Africa/L. America |
+ |
|
4. |
Schistosomiasis |
600 |
200 |
Tropics/subtropics |
++ |
|
5. |
African trypanosomiasis |
50 |
(25,000 new cases/year) |
Tropical Africa |
+ |
|
6. |
Leishmaniases |
350 |
12 million infected |
Asia/S.Europe/Africa/S. America |
? |
|
7. |
Dracunculiasis |
63 |
1 |
Tropics (Africa/Asia) |
0 |
|
Arboviral diseases |
|||||
|
8. |
Dengue |
1,500 |
Tropics/subtropics |
++ |
|
|
9. |
Yellow fever |
+++ |
Africa/L. America |
+ |
|
|
10. |
Japanese encephalitis |
+++ |
E/S.E. Asia |
+ |
|
|
11. |
Other arboviral diseases |
+++ |
+ |
||
a The numbers refer to explanations in the text. b Based on a world population estimated at 4.8 billion (1989).
0 = unlikely; + = likely; ++ = very likely; +++ = no estimate available; ? = not known.
Worldwide, malaria is the most prevalent vector-borne disease and causes one to two million deaths annually. An estimated one million additional annual fatalities may arise from climate change by the middle of the next century, according to Martens et al. (1995). The Anopheline mosquito which carries malaria can extend to the 16 °C winter isotherm, since parasite development does not occur below this temperature (Gilles and Warrell 1993). Epidemics occurring at higher altitudes generally coincide with above average temperatures (Loevinsohn 1994). Deforestation also affects malaria, since cleared areas provide an abundance of freshwater pools in which Anopheline larvae can develop (see “Species extinction, biodiversity loss and human health” in this chapter).
Over the past two decades, efforts to control malaria have made only marginal gains. Treatment has not improved as drug-resistance has become a major problem for the most virulent strain, Plasmodium falciparum, and antimalarial vaccines have shown only limited efficacy (Institute of Medicine 1991). Great capacity for antigenic variation of protozoans has thus far prevented acquisition of effective vaccines for malaria and sleeping sickness, leaving little optimism for readily available new pharmaceutical agents against these diseases. Diseases which involve intermediate reservoir hosts (e.g., deer and rodents in the case of Lyme disease) make human herd immunity from vaccination programmes essentially unattainable, representing another hurdle to preventive medical intervention.
As climate change alters habitat, causing a potential reduction of biodiversity, insect vectors will be forced to find new hosts (see “Species extinction, biodiversity loss and human health”). In Honduras, for example, blood-seeking insects such as the assassin beetle, which carries incurable Chagas’ disease (or American Trypanosomiasis), has been forced to seek human hosts as biodiversity decreases from deforestation. Of 10,601 Hondurans studied in endemic regions, 23.5% are now seropositive for Chagas’ disease (Sharp 1994). Zoonotic diseases are frequently the source of human infections, and generally affect man after an environmental change or alteration of human activity (Institute of Medicine l992). Many “newly emerging” diseases in humans are actually long-standing zoonoses of animal host species. For example, Hantavirus, recently found to be the cause of human fatalities in the southwest United States, has long been established in rodents and the recent outbreak was felt to be related to climatic/ecological conditions (Wenzel 1994).
Marine effects
Climate change may further impact public health through effects on harmful marine phytoplankton (or algae) blooms. Increases in phytoplankton globally has been a consequence of poor erosion control management, liberal agricultural application of fertilizers, and coastal sewage release, all resulting in effluents rich in nutrients which promote algae growth. Conditions that favour this growth could be augmented by warmer sea surface temperatures expected with global warming. Overharvesting of fish and shellfish (algae consumers) coupled with widespread pesticide use toxic to fish, further contribute to plankton overgrowth (Epstein 1995).
Red tides causing diarrhoeal and paralytic diseases and amnesic shellfish poisoning are prime examples of diseases stemming from algal overgrowth. Vibrio cholera has been found to be harboured by marine phytoplankton; thus blooms could represent an expanded reservoir from which cholera epidemics may initiate (Huq et al. 1990).
Food supply and human nutrition
Malnutrition is a major cause of infant mortality and childhood morbidity due to immunosuppression (see “Food and agriculture”). Climate change could adversely affect agriculture both by long-term changes, such as reducing soil moisture through evapotranspiration, and, more immediately, by extreme weather events such as droughts, flooding (and erosion) and tropical storms. Plants may initially benefit from “CO2 fertilization”, which can enhance photosynthesis (IPCC 1990). Even accounting for this, agriculture in developing countries will suffer most, and it is estimated that in these nations, 40-300 million additional people will be at risk from hunger due to climate change (Sharp 1994).
Indirect ecological changes affecting crops will need to be considered as well, since agricultural pests may change in distribution (IPCC 1992) (see “Food and agriculture”). Considering complex ecosystem dynamics, complete assessment will need to extend beyond the direct impacts of changing atmospheric and/or soil conditions.
Health Effects of Weather Disasters and Sea Level Rise
Thermal expansion of oceans may cause sea level to rise at a relatively rapid rate of two to four centimetres per decade, and projected extremes of the hydrologic cycle are expected to produce more severe weather patterns and storms. Such events would directly disrupt dwellings and public health infrastructures, such as sanitation systems and stormwater drainage (IPCC 1992). Vulnerable populations in low-lying coastal areas and small islands would be forced to migrate to safer locations. Resulting overcrowding and poor sanitation among these environmental refugees could amplify the spread of infectious diseases such as cholera, and vector-borne disease transmission rates would escalate due to crowding and potential influxes of infected individuals (WHO 1990d). Flooded drainage systems may further exacerbate the situation, and psychological impacts must also be considered from post-traumatic stress syndrome following major storms.
Fresh water supply would diminish due to saline intrusion of coastal aquifers and coastal farmland lost to salination or outright inundation. For example, a sea-level rise of one metre would destroy 15% and 20% of agriculture in Egypt and Bangladesh respectively (IPCC 1990). As for droughts, adaptive irrigation methods could affect arthropod and invertebrate breeding sites of vectors (e.g., similar to schistosomiasis in Egypt), but cost/benefit evaluation of such impacts will be difficult.
Health Effects of Stratospheric Ozone Depletion
Direct health effects of ultravioletB radiation
Ozone specifically blocks the penetration of ultravioletB radiation, which contains the most biologically destructive wavelengths of 290-320 nanometres. UVB induces the formation of pyrimidine dimers within DNA molecules, which if unrepaired can evolve to cancer (IARC 1992). Non-melanoma skin cancer (squamous and basal cell carcinoma) and superficial spreading melanoma are correlated with sunlight exposure. In Western populations, melanoma incidence has increased by 20 to 50% every five years over the past two decades (Coleman et al. 1993). While there is no direct relationship between cumulative ultraviolet exposure and melanoma, excessive UV exposure during childhood is associated with incidence. For a sustained 10% decline in the stratospheric ozone layer, non-melanoma skin cancer cases could rise by 26%, or 300,000 globally per year; melanoma could increase by 20%, or 4,500 more cases annually (UNEP 1991a).
Eye cataract formation causes half of the world’s blindness (17 million cases annually) and is associated with UVB radiation in a dose-response relationship (Taylor 1990). Amino acids and membrane transport systems in the lens of the eye are especially prone to photo oxidation by oxygen radicals generated by UVB irradiation (IARC 1992). A doubling of UVB exposure could cause a 60% increase in cortical cataracts over current levels (Taylor et al. 1988). UNEP estimates that a 10% sustained loss of stratospheric ozone would result in nearly 1.75 million extra cataracts annually (UNEP 1991a). Other ocular effects of UVB exposure include photokeratitis, photokerato-conjunctivitis, pinguecula and pterygium (or overgrowth of the conjunctival epithelium) and climatic droplet keratopathy (IARC 1992).
The ability of the immune system to function effectively depends on “local” antigen processing and presentation to T-cells, as well as augmentation of the “systemic” response via lymphokine (biochemical messenger) production and resultant T-helper/T-suppressor cell ratios. UVB causes immunosuppression at both levels. UVB in animal studies can affect the course of infectious skin diseases, such as onchocerciasis, leishmaniasis and dermatophytosis, and impair immunosurveillance of transformed, precancerous epidermal cells. Preliminary studies further show an influence on vaccine efficacy (Kripke and Morison 1986; IARC 1992).
Indirect public health effects of UVB
Historically, terrestrial plants became established only after the formation of the shielding ozone layer, since UVB inhibits photosynthesis (UNEP 1991a). Weakening of food crops susceptible to UVB damage could further extend the impacts on agriculture due to climate changes and sea-level rise.
Phytoplankton are at the foundation of the marine food chain and also serve as an important carbon dioxide “sink”. UV damage to these algae in polar regions, therefore, would detrimentally affect the marine food chain and exacerbate the greenhouse effect. UNEP estimates that a 10% loss of marine phytoplankton would limit the oceans’ annual CO2 uptake by five gigatonnes, which equals the yearly anthropogenic emissions from fossil fuel combustion (UNEP 1991a).
Occupational Hazards and Control Strategies
Occupational hazards
With regard to reduction in GHG emissions from fossil fuels, alternate renewable energy sources will need to be expanded. The public and occupational hazards of nuclear energy are well known, and safeguarding plants, workers and spent fuel will be necessary. Methanol may serve to replace much gasoline usage; however, formaldehyde emission from these sources will present a new environmental hazard. Superconducting materials for energy efficient electricity transfer are mostly ceramics comprised of calcium, strontium, barium, bismuth, thallium and yttrium (WHO in press).
Less is known about the occupational safety in the manufacturing units for solar energy capture. Silicon, gallium, indium, thallium, arsenic and antimony are the primary elements used to build photovoltaic cells (WHO in press). Silicon and arsenic adversely affect the lungs; gallium is concentrated in the kidney, liver, and bone; and ionic forms of indium are nephrotoxic.
The destructive effects of CFCs on the stratospheric ozone layer were recognized in the 1970s, and the US EPA banned these inert propellants in aerosols in 1978. By 1985, widespread concern erupted when an Antarctic-based British team discovered the “hole” in the ozone layer (Farman, Gardiner and Shanklin 1985). Subsequent passage of the Montreal Protocol in 1987, with amendments in 1990 and 1992, has already mandated sharp cuts in CFC production.
The replacement chemicals for CFCs are the hydrochlorofluorocarbons (HCFCs) and the hydrofluorocarbons (HFCs). The presence of the hydrogen atom may more readily subject these compounds to degradation by hydroxyl radicals (OH–) in the troposphere, thus reducing potential stratospheric ozone depletion. These CFC replacement chemicals are, however, more biologically reactive than CFCs. The nature of a C-H bond makes these chemicals prone to oxidation via the cytochrome P-450 system (WHO in press).
Mitigation and adaptation
Meeting the public health challenges presented by global climate change will require (1) an integrated ecological approach; (2) reduction of greenhouse gases through industrial emission control, land use policies to maximize the extent of CO2 “sinks” and population policies to achieve both; (3) monitoring of biological indicators on both regional and global scales; (4) adaptive public health strategies to minimize the impacts from unavoidable climate change; and (5) cooperation between developed and developing nations. In short, increased integration of environmental and public health policies must be promoted.
Climate change and ozone depletion present a vast number of health risks at multiple levels and underscore the important relationship between ecosystem dynamics and sustained human health. Preventive measures must therefore be systems based, and must anticipate significant ecological responses to climate change as well as the direct physical hazards predicted. Some key elements to consider in an ecological risk assessment will include spatial and temporal variations, feedback mechanisms and use of lower level organisms as early biological indicators.
Reduction of greenhouse gases by diverting from fossil fuels to renewable energy resources represents primary prevention of climate change. Similarly, strategic land use planning and stabilization of population stress on the environment will preserve important natural greenhouse gas sinks.
Because some climate change may be unavoidable, secondary prevention through early detection by monitoring of health parameters will require unprecedented coordination. For the first time in history, attempts are being made to monitor the earth system in its entirety. The Global Climate Observing System incorporates the World Weather Watch and Global Atmosphere Watch of the World Meteorological Organization (WMO) with parts of UNEP’s Global Environmental Monitoring System. The Global Ocean Observing System is a new joint endeavour by the Intergovernmental Oceanographic Commission of UN Educational, Scientific and Cultural Organization (UNESCO), WMO and the International Council of Scientific Unions (ICSU). Both satellite and underwater measurements will be utilized to monitor changes in marine systems. The Global Terrestrial Observing System is a new system sponsored by UNEP, UNESCO, WMO, ICSU and the Food and Agricultural Organization (FAO), and will provide the terrestrial component of the Global Climate Observing System (WMO 1992).
Adaptive options to reduce unavoidable health consequences include disaster preparedness programmes; urban planning to reduce the “heat island” effect and improve housing; land use planning to minimize erosion, flash flooding and unnecessary deforestation (e.g., halting the creation of rangeland for meat exportation); personal adaptive behaviours, such as avoiding sun exposure; and vector-control and expanded vaccination efforts. Unintended costs of adaptive control measures of, for example, increased pesticide use will require consideration. Over-dependence on pesticides not only leads to insect resistance but also eliminates natural, beneficial, predatory organisms. The adverse effect on public health and the environment due to current pesticide use is estimated to be between US$100 billion and US$200 billion annually (Institute of Medicine 1991).
Developing countries will suffer disproportionately more from the consequences of climate change, though industrialized nations are presently more responsible for GHGs in the atmosphere. In the future poorer countries will influence the course of global warming significantly more, both through the technologies they choose to adopt as their development accelerates, and by land use practices. Developed nations will need to embrace more environmentally sound energy policies and promptly transfer new (and affordable) technology to developing countries.
Case Study: Mosquito-borne viruses
Mosquito-borne encephalitis and dengue fever are prime examples of vector-borne diseases whose distributions are limited by climate. Epidemics of St. Louis encephalitis (SLE), the most common arboviral encephalitis in the United States, generally occur south of the 22°C June isotherm, but northerly outbreaks have occurred during unseasonably warm years. Human outbreaks are highly correlated with several-day periods when temperature exceeds 27°C (Shope 1990).
Field studies on SLE indicate that a 1°C increase in temperature significantly shortens the elapsed time between a mosquito blood-meal and viral replication to the point of infectivity within the vector, or the extrinsic incubation period. Adjusting for reduced adult mosquito survival at elevated temperatures, a 3 to 5 °C temperature increase is predicted to cause a significant northern shift of SLE outbreaks (Reeves et al. 1994).
The range of the primary mosquito vector of dengue (and yellow fever), Aedes aegypti, extends to 35° latitude because freezing temperatures kill both larvae and adults. Dengue is widespread in the Caribbean, tropical America, Oceania, Asia, Africa and Australia. Over the past 15 years, dengue epidemics have increased in both numbers and severity, especially in tropical urban centres. Dengue haemorrhagic fever now ranks as one of the leading causes for hospitalization and mortality of children in Southeast Asia (Institute of Medicine 1992). The same increasing pattern observed in Asia 20 years ago is now occurring in the Americas.
Climate change can potentially alter dengue transmission. In Mexico in 1986, the most important predictor of dengue transmission was found to be the median temperature during the rainy season, with an adjusted fourfold risk observed between 17 °C and 30 °C (Koopman et al. 1991). Lab studies support these field data. In vitro, the extrinsic incubation period for dengue type-2 virus was 12 days at 30 °C and only seven days at 32 to 35 °C (Watts et al. 1987). This temperature effect of shortening the incubation period by five days translates to a potentially threefold higher transmission rate of disease (Koopman et al. 1991). Finally, warmer temperatures result in the hatching of smaller adults, which must bite more frequently to develop an egg batch. In summary, increased temperatures can lead to more infectious mosquitoes that bite more frequently (Focks et al. 1995).
More...
Species Extinction, Biodiversity Loss and Human Health
This article is adapted with permission from Chivian, E. 1993. Species Extinction and Biodiversity Loss: The Implications for Human Health. In “Critical Condition: Human Health and the Environment”, edited by E Chivian, M McCally, H Hu and A Haines. Cambridge, Mass. and London, England: MIT Press. With thanks to EO Wilson, Richard Schultes, Stephen Morse, Andrew Spielman, Paul Epstein, David Potter, Nan Vance, Rodney Fujita, Michael Balick, Suzan Strobel and Edson Albuquerque.
Human activity is causing the extinction of animal, plant and microbial species at rates that are a thousand times greater than those which would have occurred naturally (Wilson l992), approximating the largest extinctions in geological history. When homo sapiens evolved, some l00 thousand years ago, the number of species that existed was the largest ever to inhabit the Earth (Wilson l989). Current rates of species loss are reducing these levels to the lowest since the end of the Age of Dinosaurs, 65 million years ago, with estimates that one-fourth of all species will become extinct in the next 50 years (Ehrlich and Wilson l99l).
In addition to the ethical issues involved - that we have no right to kill off countless other organisms, many of which came into being tens of millions of years prior to our arrival - this behaviour is ultimately self-destructive, upsetting the delicate ecological balance on which all life depends, including our own, and destroying the biological diversity that makes soils fertile, creates the air we breathe and provides food and other life-sustaining natural products, most of which remain to be discovered.
The exponential growth in human population coupled with an even greater rise in the consumption of resources and in the production of wastes, are the main factors endangering the survival of other species. Global warming, acid rain, the depletion of stratospheric ozone and the discharge of toxic chemicals into the air, soil and fresh- and salt-water ecosystems - all these ultimately lead to a loss of biodiversity. But it is habitat destruction by human activities, particularly deforestation, that is the greatest destroyer.
This is especially the case for tropical rainforests. Less than 50% of the area originally covered by prehistoric tropical rainforests remains, but they are still being cut and burned at a rate of approximately l42,000 square kilometres each year, equal in area to the countries of Switzerland and the Netherlands combined; this is a loss of forest cover each second the size of a football field (Wilson l992). It is this destruction which is primarily responsible for the mass extinction of the world’s species.
It has been estimated that there are somewhere between l0 million and l00 million different species on Earth. Even if a conservative estimate of 20 million total world species is used, then l0 million species would be found in tropical rainforests, and at current rates of tropical deforestation, this would mean 27,000 species would be lost in tropical rainforests alone each year, or more than seventy-four per day, three each hour (Wilson l992).
This article examines the human health implications resulting from this widespread loss of biological diversity. It is the author’s belief that if people fully comprehended the effect these massive species extinctions will have - in foreclosing the possibility of understanding and treating many incurable diseases, and ultimately, perhaps, in threatening human survival - then they would recognize that the current rates of biodiversity loss represent nothing less than a slowly evolving medical emergency and would demand that efforts to preserve species and ecosystems be given the highest priority.
The Loss of Medical Models
Three groups of endangered animals, far apart in the animal kingdom - dart-poison frogs, bears and sharks - offer striking examples of how important models for biomedical science are in danger of being squandered by humans.
Dart-poison frogs
The entire family of dart-poison frogs, the Dendrobatidae, found in the American tropics, is threatened by destruction of its habitats - the lowland tropical rainforests of Central and South America (Brody l990). These brightly coloured frogs, which include more than l00 species, are particularly sensitive to deforestation, as they often live only in very specific areas of the forest and cannot live naturally anywhere else. Scientists have come to understand that the toxins they produce, used for centuries to poison arrows and blowgun darts by Central and South American Indians, are among the deadliest natural substances known. They are also enormously useful to medicine. The active ingredients of the toxins are alkaloids, nitrogen-containing ring compounds almost exclusively found in plants (morphine, caffeine, nicotine and cocaine are examples). The alkaloids bind selectively to specific ion channels and pumps in nerve and muscle membranes. Without them, knowledge of these basic units of membrane function, found throughout the animal kingdom, would be very incomplete.
In addition to their value in basic neurophysiological research, dart-poison frogs also offer valuable biochemical clues for the production of new and potent analgesics that have a mechanism of action different from that of morphine, of new medicines for cardiac arrhythmias and of new treatments for the alleviation of some neurological diseases such as Alzheimer’s disease, myasthenia gravis and amyotrophic lateral sclerosis (Brody l990). If rainforest destruction continues at its present rate in Central and South America, these extremely valuable frogs will be lost.
Bears
The growing black market trade in Asia for bear parts, with bear gallbladders being sold for their reputed medicinal value (worth l8 times their weight in gold), and paws for gourmet food (Montgomery l992), coupled with continued hunting and the destruction of habitats, has imperilled bear populations in many parts of the world. If some species of bears become extinct, we will all be the poorer, not only because they are beautiful, fascinating creatures that fill important ecological niches, but also because some species possess several unique physiological processes that may provide important clues for treating various human disorders. “Hibernating” (or, more accurately, “denning”) black bears, for example, are immobile for up to five months in the winter, yet do not lose bone mass (Rosenthal 1993). (True hibernators, like the marmot, woodchuck and ground squirrel, show a marked lowering of body temperature during hibernation and are not easily aroused. Black bears, by contrast, “hibernate” at near normal body temperatures and can be fully responsive to defend themselves instantly.) In contrast to humans, who would lose almost one-fourth of their bone mass during a similar period of immobility (or lack of weight bearing), bears continue to lay down new bone, making use of circulating calcium in their blood (Floyd, Nelson and Wynne 1990). Understanding the mechanisms of how they accomplish this feat may lead to effective ways of preventing and treating osteoporosis in the elderly (an enormous problem leading to fractures, pain and disability), in those confined to bedrest for long periods and in astronauts subject to prolonged states of weightlessness.
In addition, “hibernating” bears do not urinate for months. Humans who cannot excrete their waste products in urine for several days build up high levels of urea in their blood and die from its toxicity. Somehow bears recycle their urea to make new proteins, including those in muscle (Nelson 1973). If we could determine the mechanism of this process, it might lead to successful, long-term treatments for those with kidney failure, who must now rely on regular detoxification by kidney dialysis machines, or on transplantation.
Sharks
Like bears, many species of sharks are being decimated because of the demand for shark meat, especially in Asia, where shark fins for soup command prices as high as $l00 a pound (Stevens l992). Because sharks produce few offspring, grow slowly and take years to mature, they are highly vulnerable to overfishing.
Sharks have been around for almost 400 million years and have evolved highly specialized organs and physiological functions that have protected them against virtually all threats, except slaughter by humans. The wiping out of populations and extinction of some of the 350 species may become a major disaster for human beings.
The immune systems of sharks (and of their relatives, skates and rays) seem to have evolved so that the animals are almost invulnerable to developing cancers and infections. While tumours are often seen in other fish and molluscs (Tucker l985), they are rare in sharks. Preliminary investigations have supported this finding. It has proved impossible, for example, to produce tumour growth in Nurse Sharks with repeated injections of known potent carcinogenic substances (Stevens l992). And researchers at the Massachusetts Institute of Technology have isolated a substance, present in large amounts, from Basking Shark cartilage (Lee and Langer l983) that strongly inhibits the growth of new blood vessels towards solid tumours, and thereby prevents tumour growth.
Sharks may also provide valuable models for developing new types of medications to treat infections, especially important at the present time when infectious agents are developing increasing resistance to currently available antibiotics.
Other models
Countless other examples could be mentioned of unique plants, animals and micro-organisms holding the secrets of billions of evolutionary experiments that are increasingly threatened by human activity and in danger of being lost forever to medical science.
The Loss of New Medicines
Plant, animal and microbial species are themselves the sources for some of today’s most important medicines and make up a significant proportion of the total pharmacopoeia. Farnsworth (1990), for example, has found that 25% of all prescriptions dispensed from community pharmacies in the United States from l959 to l980 contained active ingredients extracted from higher plants. A much higher percentage is found in the developing world. As many as 80% of all people living in developing countries, or roughly two thirds of the world’s population, rely almost exclusively on traditional medicines using natural substances, mostly derived from plants.
The knowledge held by traditional healers, often passed down orally over centuries, has led to the discovery of many medicines that are widely used today - quinine, physostigmine,
d-tubocurarine, pilocarpine and ephedrine, to name a few (Farnsworth et al. l985). But that knowledge is fast disappearing, particularly in the Amazon, as native healers die out and are replaced by more modern medical practitioners. Botanists and pharmacologists are racing to learn these ancient practices, which, like the forest plants they employ, are also endangered (Farnsworth l990; Schultes l99l; Balick l990).
Scientists have analysed the chemistry of less than 1% of known rainforest plants for biologically active substances (Gottlieb and Mors l980) - as well as a similar proportion of temperate plants (Schultes l992) and even smaller percentages of known animals, fungi and microbes. But there may be tens of millions of species as yet undiscovered in the forests, in soils, and in lakes and oceans. With the massive extinctions currently in progress, we may be destroying new cures for incurable cancers, for AIDS, for arteriosclerotic heart disease and for other illnesses that cause enormous human suffering.
Disturbing Ecosystem Equilibria
Finally, the loss of species and the destruction of habitats may upset delicate equilibria among ecosystems on which all life depends, including our own.
Food supplies
Food supplies, for one, may be seriously threatened. Deforestation, for example, can result in significantly reduced rainfall in adjacent agricultural areas and even in regions at some distance (Wilson l988; Shulka, Nobre and Sellers l990), compromising crop productivity. The loss of topsoil from erosion, another consequence of deforestation, can have an irreversible negative impact on crops in forested regions, particularly in areas of hilly terrain, such as in regions of Nepal, Madagascar and the Philippines.
Bats and birds, among the major predators of insects that infest or eat crops, are being lost in record numbers (Brody l99l; Terborgh 1980), with untold consequences for agriculture.
Infectious diseases
Recently in Brazil, malaria has reached epidemic proportions as a consequence of massive settlement and environmental disruption of the Amazon basin. Largely under control in Brazil during the l960s, malaria has exploded 20 years later, with 560,000 cases reported in l988, 500,000 in Amazonia alone (Kingman l989). In large part, this epidemic was a consequence of the influx of huge numbers of people who had little or no immunity to malaria, who lived in make-shift shelters and wore little protective clothing. But it was also an outgrowth of their disturbing the environment of the rainforest, creating in their wake stagnant pools of water everywhere - from road construction, from silt runoff secondary to land clearing, and from open mining - pools where Anopheles darlingi, the most important malaria vector in the area, could multiply unchecked (Kingman l989).
The story of “emerging” viral illnesses may hold valuable clues for understanding the effects of habitat destruction on human beings. Argentine haemorrhagic fever, for example, a painful viral disease having a mortality of between 3 and l5% (Sanford 1991) has occurred in epidemic proportions since l958 as a result of the widespread clearing of the pampas of central Argentina and the planting of corn (Kingman l989).
The emerging viral illness which has had the greatest impact on human health, and which may be a harbinger of future viral outbreaks, is AIDS, caused by the human immunodeficiency virus - types l (HIV-l) and 2 (HIV-2). There is general agreement that the current AIDS epidemic originated from non-human primates in Africa, which have acted as natural, asymptomatic hosts and reservoirs for a family of immunodeficiency viruses (Allan l992). Good genetic evidence exists for the links of HIV-l to a simian immunodeficiency virus in African chimpanzees (Huet and Cheynier l990) and of HIV-2 to another simian virus in African sooty mangabeys (Hirsch and Olmsted l989; Gao and Yue l992). Are these cross-species viral transmissions from primates to humans the result of human encroachment into degraded forest environments?
If this is the case, we may be witnessing with AIDS the beginning of a series of viral epidemics originating from tropical rainforests where there may be thousands of viruses that could infect humans, some of which may be as lethal as AIDS (approaching l00%) but spread more easily, for instance by airborne droplets. These potential viral diseases could become the most serious public health consequence from environmental disruption of the rainforests.
Other effects
But it may be the disruption of other interrelationships among organisms, ecosystems and the global environment, about which almost nothing is known, that may prove the most catastrophic of all for human beings. What will happen to global climate and to the concentration of atmospheric gases, for example, when some critical threshold of deforestation has been reached? Forests play crucial roles in the maintenance of global precipitation patterns and in the stability of atmospheric gases.
What will be the effects on marine life if increased ultraviolet radiation causes massive ocean phytoplankton kills, particularly in the rich seas beneath the Antarctic ozone “hole”? These organisms, which are at the base of the entire marine food chain and which produce a significant portion of the world’s oxygen and consume a significant portion of its carbon dioxide, are highly vulnerable to ultraviolet damage (Schneider l99l; Roberts l989; Bridigare l989).
What will be the consequences for plant growth if acid rain and toxic chemicals poison soil fungi and bacteria essential for soil fertility? There has already been a 40-50% loss in species of fungi in Western Europe during the past 60 years, including many symbiotic mycorhizal fungi (Wilson l992), crucial to the absorption of nutrients by plants. No one understands what the effects of this loss will be.
Scientists do not know the answers to these and other critically important questions. But there are worrisome biological signals which suggest that major damage to global ecosystems has already occurred. The rapid simultaneous drop in populations of many species of frogs worldwide, even in pristine environments far from people, indicates that they may be dying as a consequence of some global environmental change (Blakeslee l990). Recent studies (Blaustein 1994) suggest that increased ultraviolet-B radiation from thinning of the ozone layer may be the cause in some of these cases.
Closer to humans, marine mammals such as striped dolphins in the Mediterranean, European harbour seals off the coast of Scandinavia and of northern Ireland, and Beluga whales in the Saint Lawrence River are also dying in record numbers. In the case of the dolphins and the seals, some of the deaths seem to be due to infections by morbilli viruses (the family of viruses including measles and canine distemper virus) causing pneumonias and encephalitides (Domingo and Ferrer l990; Kennedy and Smyth l988), perhaps also the consequence of compromised immune systems. In the case of the whales, chemical pollutants such as DDT, the insecticide Mirex, PCBs, lead and mercury seem to be involved, suppressing the Belugas’ fertility and causing their deaths ultimately by a variety of tumours and pneumonias (Dold l992). The Beluga carcasses were often so filled with these pollutants that they could be classified as hazardous waste.
Are these “indicator species”, like canaries that die in coal mines containing poisonous gases, warning us that we are upsetting fragile ecosystem balances that support all life, including our own? The 50% drop in sperm counts in healthy men worldwide during the period l938-l990 (Carlsen et al. l992), the marked increases in the rate of congenital malformations of the external genitalia in males in England and Wales from l964 to l983 (Matlai and Beral l985), the dramatic rise in some cancer incidence rates for white children from l973 to l988 (Angier l99l) and for white adults from l973 to l987 (Davis, Dinse and Hoel l994) in the United States, and the steady growth in the mortality rates for several cancers worldwide for the last three to four decades (Kurihara, Aoki and Tominaga l984; Davis and Hoel l990a, 1990b; Hoel l992) all suggest that environmental degradation may be starting to compromise not only the survival of frogs, marine mammals and other animal, plant and microbial species, but that of the human species as well.
Summary
Human activity is causing the extinction of animal, plant and microbial organisms at rates that may well eliminate one-fourth of all species on Earth within the next 50 years. There are incalculable human health consequences from this destruction:
- the loss of medical models to understand human physiology and disease
- the loss of new medicines that may successfully treat incurable cancers, AIDS, arteriosclerosis and other diseases that cause great human suffering.
Overview: Occupational Safety and Health and the Environment - Two Sides of the Same Coin
This is the first edition of the Encyclopaedia of Occupational Health and Safety to explicitly integrate relevant environmental issues within its scope. This chapter highlights a number of basic environmental policy issues which are increasingly linked to occupational safety and health. Other specialized environmental chapters include Environmental Health Hazards and Environmental Pollution Control. In addition, a special effort has been made to include sections concerning environment within each of the chapters on key industrial sectors. When first considering whether such a strategy to integrate environmental issues was indeed warranted in the Encyclopaedia, we began with the very limited perspective of including only a single chapter which would serve as a useful “cross-reference” demonstrating how occupational safety and health issues and the working environment have become increasingly linked to environmental issues. As the ILO has been stating for the past twenty-plus years: the working environment and the general environment represent “two sides of the same coin”.
It is also blatantly clear, however, that the magnitude and scope of the challenges this “two-sided coin” represents for the workers of this world are grossly underestimated and under-targeted for action. The meritable successes which receive legitimate attention and praise in this Encyclopaedia risk leading us towards a dangerous and false sense of security and confidence as regards the present state of the art in occupational safety and health and the environment. The very best of our technologies, management practices and tools have indeed made impressive strides towards remediating and preventing problems in a number of key sectors, particularly in industrialized countries. But it is also true that the global reach of these technologies, management practices and tools is indeed insufficient and limited, especially in developing countries and in transition economies.
This chapter describes a few of the most useful tools and practices available to deal with occupational health and safety and environmental problems and challenges, although it would be misleading to suggest that these are already in fact widely applied throughout the world. It is important, however, that occupational health and safety practitioners all over the world learn more about these tools and practices as a step towards their greater application and practical adaptation to different economic and social conditions.
The first article in this chapter provides a brief review of inter-relationships between occupational safety and health and the working environment, policies and issues related to the general environment and the concept of “sustainable development”. This concept became the guiding principle for Agenda 21, the action plan for the 21st century adopted at the United Nations Conference on Environment and Development (UNCED) in Rio de Janeiro in June 1992. The past comfortable—and yet seriously misleading—view that it was not only possible but essential to differentiate problems and responses between those that deal with action at the workplace and those that deal with what occurs outside the gates of the enterprise has become blurred. In fact, today both workers and employers and their organizations have begun to recognize explicitly that the enterprise gate is far from impermeable to the effects of policies and problems encountered on both sides of that gate.
Given the growing recognition that occupational safety and health issues may have been treated in too isolated a manner in the past, this chapter provides a series of brief descriptions of a number of environmental policy issues which occupational safety and health practitioners may find particularly relevant to their own activities and concerns. The chapter contains two articles on environmental law and regulations which describe the present state of the art as regards the rapid expansion of international and national legal responses to existing and potential future environmental problems and concerns.
The chapter contains four articles describing some of the most important environmental policy tools being used today to improve environmental performance not only in industry, but also in all other sectors of our economy and throughout our societies. The articles focus upon environmental impact assessments, life-cycle analysis, risk assessment and communication and environmental auditing. The final section of this chapter provides two perspectives on pollution prevention and control: one focusing on making pollution prevention a corporate priority and the other providing a trade union perspective of pollution prevention and cleaner production technologies.
The overall objective of this chapter is to enable the reader to better perceive and understand the growing inter-relationships between occupational safety and health and the working environment, and the broader environmental issues beyond the workplace. A greater recognition of these linkages will hopefully also lead to more extensive and effective exchanges of experience and information between occupational health and safety and environmental specialists, with a view to enhancing our capacity to respond to challenges in the working environment and beyond.
Environment and the World of Work: An Integrated Approach to Sustainable Development, Environment and the Working Environment
It should come as no surprise to occupational health and safety practitioners that if one traces back from most of our present major environmental problems—one arrives at a workplace! Likewise, the serious occupational health and safety consequences of some chemicals and substances have become an early warning system of potential environmental health consequences far beyond the workplace.
Despite the obvious inter-relationship between the working environment and the environment, many governments, employers and workers continue to respond to the causes and consequences of both working environment and environment issues in very disparate and isolated ways. (Given the importance of distinguishing between the working environment and those broader environmental perspectives represented by such adjectives as physical, general or external, this article will use the term working environment to encompass all occupational health, safety and environment issues within the workplace and the term environment to encompass those environmental issues beyond the workplace.) The goal of this article is to draw attention to the significant advantages which may arise from responding to the environment—within and outside the workplace—in a more integrated and strategic fashion. This is true not only for industrialized countries, which have made significant progress regarding both occupational safety and health and environment, but as well in transition economies and developing countries, which have a much broader and overwhelming challenge yet before them.
As this article has been specifically prepared for the Fourth Edition of the Encyclopaedia of Occupational Health and Safety it does not attempt to review the full range of occupational health and safety (OHS) issues related to the environment, many of which are reflected in other chapters of the Encyclopaedia. In fact, occupational health and safety is an integral part of every enterprise’s “environmental” performance. This is not to suggest that OHS and environmental protection are always totally compatible and mutually reinforcing; occasionally they may also be antagonistic. Nevertheless, the objective should be to find ways to protect both workers’ health and safety and the broader environment, and to avoid options which suggest that one needs to choose one or the other. The identification of environmental problems and response strategies has too often led to the creation of false dichotomies—environmental protection versus worker safety or environmental protection versus job security. While such conflicts may indeed exist in very specific and special circumstances, the majority of situations require a series of trade-offs and careful longer-term approaches for meeting both environmental and worker protection and employment objectives. This leads to a corollary thesis that worker-employer collaboration is a critical factor necessary for improved performance regarding both OHS and environment.
This perspective on environment and the world of work is especially evident if one assumes that OHS performance at the workplace should be driven by a focus on prevention rather than simply on control and remediation. The concept of prevention is fundamental to future improvements in OHS and the environment. Early in the 20th century in industrialized countries, OHS was often driven by a simplistic focus on control—the protection of workers from exposure to health and safety risks. Special emphasis was given to engineering solutions to limit accidents by improving machinery—for example, by introducing protective devices. As our knowledge of the health consequences related to the exposure of workers to certain chemicals and substances expanded, the “logical” response strategy was often first to protect the worker from exposure by improving ventilation systems or the wearing of protective devices. While important early exceptions exist, particularly in industrialized countries, it is a relatively recent phenomenon of the past few decades that so much public attention is being increasingly devoted in a number of key industrial sectors to eliminating or replacing the dangerous or toxic chemicals/substances with those which are significantly less harmful. It is interesting to note that this growing emphasis on prevention of the emission itself, or the use of specific chemicals, has grown at the same time as the public has become increasingly aware of and actively involved in environmental challenges.
This new environmental awareness has stressed both the immediate and longer-term consequences of environmental degradation for our societies and our economies. Such public interest in the environment appears to have also supported workers’ ongoing efforts to collaborate with employers to improve occupational safety and health. Nevertheless, it is blatantly clear that serious action to date regarding OHS and environment represents only a tip of the proverbial iceberg of OHS and environmental problems evident on our planet, and even more dramatically evident in developing countries and transition economies.
Environmental priorities and policies in industrialized countries have travelled a very similar path from control to prevention strategies, albeit in a much shorter time span than that of OHS. Concern for the environment in its early stages was in fact limited to a concern about “pollution”. Attention was focused primarily on emissions to air, water and soils generated by the production process. Therefore, response strategies similarly often focused on “end-of-pipe” strategies to deal with the problem of local emissions. Citing just one rather simple example, this narrow approach led to solutions such as taller chimneys, which unfortunately did not eliminate the pollution but rather dispersed it far beyond the enterprise gate and the local community. While this often satisfied the local community and the workers who lived and worked there, new environmental problems were created—long-distance and even transboundary air pollution, which in some cases leads to what has been called “acid rain”. Once the secondary effects of this end-of-pipe solution became evident, there followed considerable delay before some of the relevant stakeholders accepted that there were indeed other serious negative consequences created by the tall-chimney solution. The next innovative step in this process was to add on a sophisticated filtering system to trap the problem emissions before they left the chimney. As this example demonstrates, the focus of policy-makers was not on the prevention of the emissions but rather on various actions to control those emissions. Today, increasing efforts are being made to prevent the emissions by changing fuels and improving combustion technologies, as well as changing the production process itself through the introduction of so-called cleaner production technologies.
This preventive approach—which also requires a more holistic approach—has at least four significant advantages for the world of work and the environment:
- Unlike end-of-pipe technologies, which create additional costs for the production process without usually providing improvements in productivity or economic return, cleaner production technologies often lead to improvements in productivity and in measurable economic returns. In other words, end-of-pipe technologies clean up the environment but usually do not help the balance sheet. Cleaner production technologies prevent environmental degradation while also creating viable economic benefits.
- Cleaner production technologies often lead to significant improvements in the efficient use of natural resources and energy (i.e., use less natural resources to achieve comparable outputs) and also often lead to decreases in the amount of—and the toxicity of—the wastes generated.
- Efforts to introduce cleaner production technologies can and should explicitly identify measures to also improve OHS performance within the enterprise.
- Worker involvement concerning the protection of health, safety and environment as part of the cleaner technology process will lead to improvements in worker morale, understanding and job performance—all of which are well-documented factors in achieving good quality production.
Environmental policies, legislation and regulation have evolved and are leading—or at least are trying to keep up with—this process of transition from control-based approaches to prevention-centred strategies.
Both end-of-pipe and cleaner production strategies, however, have direct consequences for employment protection and creation. It is clear that in many parts of the world, particularly in industrialized countries and transition economies, there are major opportunities for job creation related to clean-up and remediation activities. At the same time, cleaner production technologies also represent a vibrant new industry which will lead to the creation of new job opportunities and, of course, will require new efforts to meet skill and training requirements. This is particularly evident in the dire need to ensure that those workers involved in meeting the challenge of environmental remediation receive effective OHS and environmental training. While much attention is being given to the potential negative impact on employment of increased regulations and controls, in the field of environment, regulation and controls, if properly developed, can lead to the creation of new jobs and promote improved environmental and OHS performance.
Another critical change in perspective towards the environment has occurred since the 1960s: a shift from an exclusive focus on production processes to give attention also to the environmental consequences of the products themselves. The most obvious example is the automobile, where considerable efforts have been made to improve its environmental “efficiency”, although much animated debate remains over whether a more efficient car should be complemented by an efficient public transport system. But clearly, all products have some environmental implications—if not in their production or use, most certainly in their eventual disposal. This shift in emphasis has led to an increasing number of environmental laws and regulations concerning the use and disposal of products, even the restriction or elimination of certain products. It also has led to new analytical techniques such as environmental impact assessments, life-cycle analysis, risk assessment and environmental auditing (see the articles later in this chapter). These new, broader perspectives on environment have implications as well for the world of work—for example, upon conditions of work for those involved in the safe disposal of products and on future employment prospects for those involved in the manufacture, sale and servicing of prohibited and restricted products.
Another driving force for environmental policy has been the rather dramatic number and scope of major industrial accidents, particularly since the Bhopal disaster in 1984. Bhopal and other major accidents like Chernobyl and the Exxon Valdez, demonstrated to the world—the public, politicians, employers and workers—that the traditional view that what happened within the gates of the workplace could not or would not affect the external environment, the general public or the health and livelihood of surrounding communities, is false. While major accidents had occurred before, the global, visual coverage of these events shocked wide segments of the public in developed and developing countries and transitional economies into a new awareness and support for environmental protection which would also protect workers and the public. It should be noted, however, that this provides another similarity to the history of action to improve occupational health and safety laws and regulations, which was also significantly promoted, for example, following early major factory fires and mining disasters.
One of the most obvious examples of the effects of these environmental driving forces, and particularly recent major “environmental” accidents, may be seen within the ILO itself, as reflected in recent decisions by its tripartite constituents. For example, the ILO has significantly enhanced its activities related to environment and the world of work. Most importantly, since 1990 three major sets of ILO working environment Conventions and Recommendations have been adopted:
- Convention No. 170 and Recommendation No. 177 concerning Safety in the Use of Chemicals at Work (1990)
- Convention No. 174 and Recommendation No. 181 concerning the Prevention of Major Industrial Accidents (1992)
- Convention No. 176 and Recommendation No. 183 concerning Safety and Health in Mines (1995).
These standards reflect an explicit extension of the traditional ILO scope from that of an exclusive focus on worker protection to also include a more holistic approach to these matters by references in the preambular or operative paragraphs to relevant aspects of the protection of the public and the environment. For example, Article 3 of Convention No. 174 states that the term major accident means “a sudden occurrence leading to a serious danger to workers, the public or environment, whether immediate or delayed”, and Article 4 states: “each Member shall formulate, implement and periodically review a coherent national policy concerning the protection of workers, the public and the environment against risk of major accidents.” The ILO’s wide range of Conventions and Recommendations related to the working environment provides a very useful source of guidance for countries working to improve their OHS and environmental performance. In this regard, it may also be useful to note that the ILO provides advisory assistance and support to its tripartite constituents with a view to helping them to ratify and implement relevant ILO standards.
In addition to these driving forces, however, there is a wide range of other factors which significantly influence the relationship between the working environment and the general environment. Clearly one of the most obvious is that despite many common concerns and issues (e.g., chemicals, accidents, health) the OHS and environmental aspects are often governed by different government ministries, different legislation, regulations and standards, and different enforcement and inspection mechanisms. These differences lead to considerable confusion, possibly additional costs as a result of duplication and, most disconcerting, to the existence of possible gaps which may lead to serious omissions concerning the protection of workers, the public and the environment. For example, recent reviews of a number of national inspectorates have drawn attention to potential problems of duplication, gaps and inconsistencies in the responsibilities assigned to factory, labour and environmental inspectorates. These reviews have also cited examples of situations in which labour inspectorates have been assigned new environmental inspection responsibilities without receiving adequate new staff and financial resources or specialized training. This has tended to deflect existing staff away from fully meeting their OHS inspection responsibilities. In addition, in many countries these legislative and inspectorate responsibilities still remain extremely limited and are not receiving adequate political and financial support. More emphasis will need to be given to developing a more integrated approach to the monitoring, enforcement and dispute settlement mechanisms related to OHS and environment regulations and standards.
While inspectorates will be essential components in any OHS and environmental protection system, by themselves they can never be sufficient. Workplace health and safety and the link between environment and the world of work will need to remain largely the responsibility of those at the enterprise level. The best way to ensure optimal performance is to ensure optimum confidence and collaboration between the workforce and management. This will need to be supported by effective training of workers and management as well as efficient joint mechanisms to support collaboration. These efforts at the enterprise level will be all the more successful if they are supported by good relations with, and access to, an adequately financed, well-trained and independent inspectorate.
The present wave of support for deregulation and structural adjustment, particularly within the public sector, if properly designed and implemented could lead to the more effective and efficient management of occupational safety and health and environmental protection. However, there are very troubling signs that suggest that this process may also lead to a deterioration of both OHS and environmental performance if governments, employers, workers and the public do not give adequate priority to these issues. All too often, OHS and environment are seen as issues which can be dealt with “later”, once more immediate economic requirements have been met. Experience suggests, however, that today’s short-term savings may lead to expensive remediation activities in the future to rectify the problems which could have been prevented at lower costs today. OHS and environment should not simply be seen as end-of-pipe and unproductive costs but rather as critical and productive social, environmental and economic investments.
Collaborative action between employers and workers at the workplace to deal with OHS issues has a long history and has clearly demonstrated its value. It is interesting to note that initially OHS issues were considered the exclusive prerogative of employers. Nevertheless, today, following very extensive efforts by the social partners, OHS issues are now seen as a matter of bipartite and/or tripartite collaboration in most countries throughout the world. In fact, many countries have established legislation requiring the creation of joint occupational health and safety committees at the workplace.
Here again, however, similar paths of development between OHS and environment are evident. When workers and their trade unions first raised issues of occupational health and safety as issues of direct concern to them, they were often dismissed as not having the knowledge and technical competence to understand or to deal with these issues. It has taken decades of dedicated effort for workers and their unions to demonstrate their fundamental role in understanding and effectively responding to these issues at the enterprise level. Workers had to insist that it was their health and safety and that they had a right to be involved in the process leading to decisions, and a positive contribution to make. Similarly, many employers and their organizations have come to recognize the benefits which have come from this collaborative process. Today, workers and their trade unions are often confronted with similar dismissive attitudes by some employers as regards their capacity and right to contribute to environmental protection. It should also be noted, however, that it is again the far-sighted and responsible employers in a limited number of high-profile sectors who are in the forefront of recognizing the talent, experience and practical common sense approach which workers can provide to improving environmental performance, and who support a well-trained, well-motivated, fully informed and fully involved workforce.
Nevertheless, some employers still argue that environment is an exclusive management responsibility and have opposed the establishment of joint safety, health and environment committees or separate joint environmental committees. Others have recognized the very critical and practical contribution that collaborative employer/worker action can make to ensuring that enterprises set and meet appropriate environmental performance standards. Such standards are no longer restricted to simply meeting mandatory legal requirements, but also include voluntary action to respond to the needs of local communities, global competitiveness, green marketing and so on. Voluntary environmental performance policies and programmes within individual enterprises or through sectoral associations (e.g., the chemical industries Responsible Care programme) often explicitly integrate both OHS and environmental considerations. Similarly, specialized and often voluntary standards prepared by organizations such as the International Organization for Standardization (ISO) also have had an increasing influence on both OHS and environmental protection.
The positive experience with collaboration between employers’ and workers’ organizations has also led to new collaborative partnerships and alliances which go beyond the workplace to ensure that all the stakeholders concerned with safety, health and environment are able to constructively participate in the process. Within the ILO we have called this new effort to expand collaborative links beyond the workplace to local community groups, environmental NGOs and other institutions involved in helping to make improvements in the world of work, “tripartite-plus” collaboration.
Several emerging issues are on the horizon which may lead to special challenges and opportunities for more effective linkages between OHS and environment. Two sectors which have been particularly difficult to reach as regards both OHS and environmental performance are small- and medium-sized enterprises (SMEs) and the urban informal sector. This is especially relevant as regards the awesome implications of one of the most critical environmental and developmental challenges of the 21st century: clean water and sanitation. New participatory approaches will need to be developed in order to better communicate the significant risks for workers and the environment related to many existing activities. Beyond the risks, however, there are also new opportunities to make improvements in productivity and to increase incomes from traditional activities, as well as the prospect of the creation of new income-generating activities directly related to the environment. Given the many direct and indirect linkages between the formal sector and SMEs and the urban informal sector, innovative approaches need to be designed which will facilitate the sharing of experiences on ways to improve OHS and environmental performance. Employers’ and workers’ organizations could play a very positive and practical role in this process.
Another emerging issue area is that of indoor air pollution. In the past we have tended to see large industrial establishments as the primary target to correct unhealthy working conditions. Today, however, there is growing recognition that many offices and commercial premises may also be encountering new occupational health problems due to indoor air pollution. This pollution is related to the increased use of chemicals and electronic equipment, intake of contaminated ambient air, the use of closed air recirculation and air conditioning systems, and the possible increased sensitivity of workers as a result of changing health patterns—for example, the growing number of cases of allergies and asthma. It may be expected that action to respond to indoor air pollution concerns will require a more integrated approach to both OHS and environmental factors than has been the case in the past.
Links to Sustainable Development
This article has so far briefly and superficially highlighted some of the past and potential future inter-relationships between OHS and the environment. This, however, already should be seen as a rather narrow perspective compared to the more holistic and integrated approach represented by the concept of sustainable development. This concept was the key—if not the “magic formula”—underlying the preparatory process to negotiate and endorse Agenda 21, the action plan for the 21st century adopted at the United Nations Conference on Environment and Development (UNCED) in Rio de Janeiro in June 1992 (see Robinson 1993). The concept of sustainable development is and will continue to be the subject of great discussion, debate and dispute. Much of this debate has been focused on semantics. For the purpose of this article, sustainable development represents both a goal and a process. As a goal, sustainable development implies development which equitably meets the needs of today’s and future generations. As a process, it means setting policies in such a way that they take into account not only economic factors but environmental and social factors as well.
If such a holistic concept is to be successfully operationalized, then the approach to all these factors will require new analysis and responses. It is essential that OHS issues become a fundamental factor in evaluating future investment and development decisions at all levels from the workplace to the negotiation of international standards. The protection of workers will need to be assessed not simply as one of the costs of doing business, but as a critical factor necessary to the achievement of economic, environmental and social objectives which are an integral part of sustainable development. This means that the protection of workers should be seen and calculated as an investment with a potentially positive rate of return within projects aimed at the achievement of environmental, social and economic objectives. The protection of workers as well cannot simply be seen as protecting them at their workplace, but should take into account the inter-relationship between their work, general health, living conditions (water, sanitation, housing), transport, culture and so on. It also implies that action to improve OHS is a prerequisite for meeting the basic economic and social development perspectives in developing countries, and not simply a luxury to be reserved for the rich countries.
As the Director-General of the ILO, Michel Hansenne, stated in his Report to the International Labour Conference in 1990:
There is in fact one central issue which pervades almost every environmental policy discussion—how to share equitably the costs and benefits of environmental action. “Who will pay for environmental improvements?” is a question which will need to be discussed and resolved at all levels, from the perspective of consumers, workers, employers, as well as from that of local, national, regional and international institutions.
For the ILO, the social and human implications of how these potential environmental costs and benefits are shared within society and between countries may be as important as the environmental actions themselves. An inequitable sharing of the social, economic and environmental costs and benefits of development, within and between countries, cannot lead to global sustainable development. Rather, it could accentuate poverty, injustice and division (ILO 1990).
In the past, and too frequently still today, workers have been called upon to pay an inequitable part of the costs of economic development through deplorable safety and health conditions (e.g., the tragic fire at the Kader Industrial Toy Company in Thailand, which took the lives of 188 workers), inadequate wages (insufficient income to meet basic family needs of food, shelter, education), lack of freedom of association and even the loss of human dignity (e.g., the use of bonded child labour). Similarly, workers and their local communities also have assumed much of the direct costs of day-to-day environmental degradation or decisions to close plants for environmental reasons. It also should be remembered that while most attention in industrialized countries has been focused on ways to avoid the potential loss of jobs as a result of environmental legislation and regulations, millions of people have already lost or have had their traditional livelihoods severely reduced as a result of ongoing desertification, deforestation, flooding and soil erosion.
Sustainable development implies that these environmental and social costs which have been “externalized” by industry and society in the past must now be internalized and reflected in the market costs of products and services. This internalization process is being encouraged by market forces and consumer groups, new laws and regulations including so-called economic instruments, as well as by decisions taken by the enterprises themselves. Nevertheless, to be successful this process of integrating the actual social and environmental costs of production and consumption will require new approaches to collaboration, communication and participation in decision-making processes. Workers’ and employers’ organizations have a critical stake in this process. They should also have a say in its design, implementation and monitoring.
In this context it may be useful to draw attention to the major diplomatic effort under way as part of the follow-up process of the UNCED Conference to facilitate an examination of the current imbalances in the global patterns of production and consumption. Chapter 4 of
Agenda 21, entitled “Changing Consumption Patterns”, indicates that action is needed to meet the following objectives:
(a) to promote patterns of consumption and production that reduce environmental stress and will meet the basic needs of humanity
(b) to develop a better understanding of the role of consumption and how to bring about more sustainable consumption patterns.
It also clearly encompasses the concept of the need for greatly expanding the basic consumption of millions of people in many parts of our world currently confronted with dire poverty and hardship. Ongoing negotiations and discussions within the framework of the Commission on Sustainable Development (CSD) may be expected to be very slow and complex. Nevertheless they could lead to significant changes in present production and consumption patterns, particularly in some of the most critical industrial sectors of our economies, including chemicals, energy and transport. They also will have significant repercussions on international trade and commerce. Such changes will no doubt also have important implications for OHS and environment practices in developed and developing countries and for many other areas of the world of work, especially employment, incomes and training.
Although these issues currently are being discussed primarily at the global level, it is obvious that it is at each workplace where they will need to be implemented. Therefore, it is essential that this global negotiation process reflect reality, that is, the constraints and opportunities at the workplace level all across our planet. With the globalization of our economies, and the rapid changes in the organization and structures of our workplaces (e.g., sub-contracting, part-time work, homeworkers, teleworking), and indeed changes in our perception of work, livelihoods and employment itself in the 21st century, this will be no easy task. If this process is to be successful, however, it will require the support of a tripartite collaborative process between governments and employers’ and workers’ organizations at all stages. Clearly such a bottom-up approach will play a vital role in guiding the national and global CSD process to achieve more sustainable production and consumption patterns in the future.
Conclusion
Articles in this chapter focus on action at the national and international levels as well as on practical policy tools to improve environmental performance. It is clear, however, that the most important environmental policies of the future will not be set at the national or international level or even by local communities—although each of these has an essential role to play. The real changes must and will come at the enterprise and workplace level. From the chief executive officer of large multinational corporations to the managers of small family businesses to rural farmers and independent workers in the informal sector will come the true impetus and commitment to follow through to achieve sustainable development. Change will be possible only through the growing awareness and joint action by employers and workers within enterprises and other relevant sectors (e.g., local communities, non-governmental organizations, etc.) to integrate OHS and environmental objectives within the overall objectives and priorities of the enterprise. Despite the magnitude of the challenge, one can foresee the range of formal and informal safety, health and environmental policies at the enterprise level developed, implemented and monitored by a collaborative process between management and workers and other stakeholders.
Occupational health and safety clearly has a significant impact on the achievement of our overall economic, environmental and social objectives. Therefore, OHS must be seen as a critical element to be included within the complex integration process to achieve sustainable development. Following the UNCED Conference, all national governments have been called upon to develop their own national Agenda 21 strategies and plans for sustainable development. Environmental objectives already are seen as an integral part of that process. Much work remains, however, before OHS and employment and social objectives and targets will become an explicit and intrinsic part of that process and the economic and political support necessary for the achievement of those objectives is mobilized.
The preparation of this article has been greatly facilitated by the technical support, useful advice and comments and regular encouragement from colleagues, governments, employers and workers from around the world who are keenly committed and competent in this field, but particularly key representatives from the International Federation of Chemical, Energy and General Workers’ Unions (ICEF); Canadian Labour Congress; the Communications, Energy and Paper Workers’ Unions of Canada; and the Labourers’ International Union of North America, who have stressed the urgent need for action in this field.
Laws and Regulations
The relationship between human health and the human environment has been recognized from time immemorial. This tenet of medicine can be traced back to Hippocrates, who taught his pupils to “attend to the airs, waters, and places” if they sought to understand the sources of health and diseases in their patients (Lloyd 1983).
This ancient view of the link between human health and the environment has persisted. The degree of a society’s acceptance of this link has been influenced by three factors: development of a scientific understanding of the human body; increased capacity to cure individual illnesses; and the evolution of parallel scientific, religious and cultural concepts.
Environmental factors as a cause of health or diseases of entire classes of people were given increased attention during the Industrial Revolution. The trend has continued to this day, assisted by the development of the environmental sciences and of techniques for determining causality and assessing risks.
It was in the workplace that causal links between health and the environment were first clearly established. It was also in the workplace that the consequences of the increase in the amount and variety of contaminants resulting from the diversification of industrial processes were first felt. Yet these contaminants cannot be confined to the occupational environment. Once released, their pathway may become difficult to follow or trace, but it inevitably ends in nature: environmental toxins are present in the soil, water and air of even the most remote environments. Human health, in turn, is affected by the pollution of the natural environment, whether of local, national or transboundary origin. Along with other types of environmental degradation, which cause worldwide depletion of natural resources, this accords a planetary dimension to the interaction between environmental conditions and public health.
The conclusion is inescapable that the quality of the work environment and of the natural environment are inextricably linked. Lasting solutions to either of these problems can be successful only if both are tackled in tandem.
Environmental Law: A Means to an End
The formulation of policies to maintain and improve both the natural and the work environment is a prerequisite to successful environmental management. Policies, however, remain a dead letter unless they are implemented. Such implementation is only achievable through the translation of policy principles into rules of law. From this perspective, law is at the service of policy, giving it concreteness and a degree of permanency through appropriate legislation.
Legislation, in turn, is a framework structure which is useful only if implemented and enforced. Implementation and enforcement are dependent on the political and social contexts in which they take place; if they are not backed by the public, they are likely to remain inefficient.
Therefore, enactment, implementation and enforcement of environmental legislation are, to a large extent, dependent on understanding and acceptance of the rules established by those to whom these rules are addressed—hence the importance of disseminating environmental information and knowledge to the public at large, as well as to specific target groups.
The Role of Environmental Law: Prevention and Cure
The role of law in the environmental field, as in many other fields, is twofold: first, to create rules and conditions which are conducive to the control or prevention of damage to the environment or human health; and, second, to offer remedies for situations where damage has occurred in spite of these rules and conditions.
Prevention through command techniques
Land use controls
The regulation of land use is a major element of environmental law, and a prerequisite to the control and guidance of land development and the utilization of natural resources. The issue is usually whether a particular environment may be put to another use, it being understood that non-use is also a type of land use.
Land use controls allow siting human activities where they are best located (or least damaging), and also subject contemplated activities to restrictions. These two goals are usually achieved by establishing a requirement for prior authorization.
Prior authorization
Prior authorization is a generic term for any form of permission (e.g., licence, permit) which must be obtained from a regulatory authority before certain activities may be undertaken.
The first step is to determine by law those private and public sector activities which are subject to prior authorization. Several approaches are possible and are not mutually exclusive:
Controls of sources. When a category of sources of environmental harm is clearly identifiable, it is usually subject to prior authorization as such (e.g., all classes of industrial facilities and motor vehicles).
Controls of substances. When a particular substance or class of substances is identified as potentially harmful to the environment, the use or release of these substances may be made subject to prior authorization.
Media-oriented controls, and integrated pollution control. Media-oriented controls are those which are directed at protecting a specific component of the environment (air, water, soil). Such controls may lead to shifting environmental harm from one medium to another, and thus fail to reduce (or may even increase) the overall degree of environmental harm. This has led to the development of coordinated prior authorization systems, whereby all pollution from one source and all recipient media are considered before one single, all-embracing authorization is granted.
Environmental standards
Environmental standards are maximum permissible limits which may be imposed directly by a law, or indirectly as conditions to obtain an authorization. These limits may be related either to the effects or the causes of environmental harm:
- Effect-related standards are those which take the target as a baseline. They include:
- (1) biological standards, (2) exposure standards and (3) environmental quality standards.
- Cause-related standards are those which take the cause of the possible environmental harm as a baseline. They include: (1) emission standards, (2) product standards and (3) process or operating standards.
A variety of factors, including the nature of the pollutant, the recipient media and the state of the art, determine which type of standard is most appropriate. Other considerations also play an important role: standard-setting provides a means to achieve a balance between what is environmentally desirable in a particular place at a particular point in time, and the socioeconomic feasibility of achieving a specific environmental goal.
It goes without saying that the stricter the standards are, the higher production costs become. Therefore, differing standards in different locations within a state or between states play an important role in determining competitive market advantages or disadvantages, and may constitute non-tariff barriers to trade—hence the desirability of seeking harmonization at the regional or global level.
Prevention through incentives and disincentives
Controls voluntarily submitted to may be used as flanking measures or as alternatives to command techniques. They usually consist of setting recommended (rather than compulsory) values, and of providing economic incentives or disincentives to achieve them.
The purpose of an incentive (e.g., accelerated depreciation allowance, tax benefit, subsidy) is to reward and, therefore, to generate, a specific environmentally friendly conduct or activity. Thus, instead of trying to achieve a certain emission level by the stick, the carrot of economic benefit is offered.
The purpose of a disincentive (e.g., fees, such as effluent or emission charge, tax or levy) is to induce environmentally friendly conduct so as to avoid paying the fee in question.
There are also other ways of inducing adherence to recommended values, for instance, through the creation of eco-label award schemes, or providing marketing advantages where consumers are sensitized to environmental concerns.
These so-called voluntary approaches are often referred to as alternatives to “legal” controls, forgetting that incentives and disincentives also have to be established by law!
Cure through sanctions or remedies
Sanctions imposed by the regulatory agency
In cases where environmental management measures may be prescribed by the regulatory agency (e.g., through a prior authorization mechanism), legal regimes usually also provide the agency with enforcement powers. A variety of techniques are available, ranging from the imposition of monetary sanctions (e.g., per day) until compliance with the requirement, to execution of the measures required (e.g., building filters) at the cost of the addressee, and finally to closure of the facility for non-compliance with administrative requirements, etc.
Each legal system provides for ways in which these measures may be challenged by those to whom they are applied. Equally important is to provide the possibility for other interested parties (e.g., NGOs representing the public interest) to challenge the decisions of the regulatory agency. In the latter case, it is not only the action of the administration which should be eligible for challenge, but also its inaction.
Penal sanctions
Legislation prescribing a certain environmental norm or conduct usually indicates that disregarding the established rules, whether intentionally or not, constitutes an offence, and determines the type of penal sanctions which are to be applied to each case. Penal sanctions may be monetary (fines) or, in serious cases, may entail incarceration, or a combination of both. Penal sanctions for environmental offences depend upon the penal system of each country. Thus, sanctions are often imposed in reference to the main body of criminal law in a particular country (e.g., a penal code), which may also include a chapter on environmental offences. Penal sanctions can be triggered by the administration or by an aggrieved party.
The legislation of many countries has been criticized for failing to declare certain environmental misconducts as penal offences, or for providing overly mild penalties for environmental offences. It has often been observed that if the quantum of the sanctions is less than the cost of internalizing environmental management measures, the culprits are likely to deliberately prefer the risk of a penal sanction, especially if this sanction may be only a fine. This is especially true when there is an enforcement deficit—that is, when the enforcement of environmental norms is lax or lenient, as is often the case.
Liability for damages
Each legal system’s rules applying to liability for damage naturally also apply to health and environmental damage. This usually means that compensation is due either in kind or specie only when the damage proves to have been caused directly by the fault of one or more originators.
In the environmental field, the difficulties in applying these principles are numerous, and have led to the enactment of sui generis environmental liability laws in an increasing number of countries. This has made it possible to provide for liability without fault, and, therefore, to allow for compensation independently of the circumstances which caused the damage. In such cases, however, a certain monetary ceiling is usually set with a view to permitting eligibility for insurance coverage, which may also be made compulsory by law.
These special regimes also attempt to better provide redress in cases of damage to the environment per se (ecological damage as opposed to economic damage), usually requiring the restoration of the environment to the status quo ante whenever the nature of the damage permits. In such a scenario, monetary damages are in order only if restoration is impossible.
Access to remedies
Not everyone may take action to generate sanctions or obtain remedies. These may traditionally be triggered only by the administration, or a physical or legal person directly affected by a certain situation. In cases where it is the environment that is affected, this is usually insufficient, since much environmental damage is not directly linked to individual human interests. Therefore, it is important for legal systems to grant “representatives” of the public interest the right to sue the administration for failure to act or for insufficient action, or to sue individuals or enterprises for breaking the law or causing damage to the environment. There are various ways in which this can be achieved: designated non-governmental organizations may be given this right; the legal system may provide for class action or citizens’ suits, etc. The right to sue in defence of the public interest, rather than only to defend a proprietary interest, is one of the most important elements of modern environmental legislation.
Conclusion
Good environmental legislation is a prerequisite to achieve and maintain the desired levels of quality in the natural, as well as in the work environment.
What “good” environmental legislation is, might be difficult to define. Some wish to see a decline in command and control methods, and their replacement by softer incitation techniques but, in practice, there is no standard formula to decide what the ingredients of the law should be. What is important, however, is to make legislation relevant to the particular situation of the country concerned, adapting available principles, methods and techniques to the needs, capacities and legal traditions of each country.
This is all the more true at a time when large numbers of developing nations and nations with economies in transition seek to equip themselves with “good” environmental legislation, or to retrofit legislation already in place. In striving towards this goal, however, legislation which is successful in a particular legal, economic and social context, frequently that of an industrialized country, is still too often imported as a model in countries and legal systems for which it is totally inappropriate.
“Particularizing” legislation is, therefore, perhaps the most important element in achieving the goal of effective environmental legislation.
" DISCLAIMER: The ILO does not take responsibility for content presented on this web portal that is presented in any language other than English, which is the language used for the initial production and peer-review of original content. Certain statistics have not been updated since the production of the 4th edition of the Encyclopaedia (1998)."